Adam's Heart Valve Surgery Blog – Page 13
Darian Overcomes Aortic Stenosis & Healthcare Inequity Thanks to Medtronic TAVR
Written By: Adam Pick, Patient Advocate & Author
Medical Expert: Mustafa Ahmed, MD, Interventional Cardiologist, UAB Medicine
Published: October 18, 2022
Aortic stenosis is a life-threatening disease that is under-diagnosed and under-treated. In fact, the survival rate is just 50% at two years for patients diagnosed with symptomatic severe aortic stenosis. To make matters worse, only 9% of patients that receive non-invasive transcatheter aortic valve replacement (TAVR) are minorities according to this research.
How is Medtronic, a leading TAVR manufacturer, changing this healthcare inequity to help aortic stenosis patients like Mrs. Darian Tymes? Watch this video to find out.
Patient Q&A: Leila’s Recovery From Heart Valve Surgery
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: October 12, 2022
I just had an insightful conversation with Leila Saeid, a mom, wife and dentist in Southern California, about her recovery from minimally-invasive heart valve surgery. We were also joined by Leila’s surgeon, Dr. Joanna Chikwe, the Chair of Cardiac Surgery at Cedars-Sinai Medical Center.
To watch this special interview with Leila and Dr. Chikwe, please click here.
Dr. Vaughn Starnes, My Surgeon, Gets 100 Patient Testimonials!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: October 10, 2022
I am very happy to announce that Dr. Vaughn Starnes, my surgeon, just became the sixth doctor to receive 100 patient reviews at HeartValveSurgery.com!
This is a wonderful milestone as Dr. Starnes and his team at Keck Medicine of USC in Los Angeles, California has successfully treated so many patients in our community with valvular diseases including aortic stenosis and mitral regurgitation.

Let’s Go Mike Gabler, Heart Valve Specialist, on Survivor!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: December 15, 2022
Survivor is one of my favorite television shows. I have watched most, if not all, of the episodes during the past forty-two seasons. I love everything about the show that many consider the “original” reality tv series.
Luckily, Robyn, my wife, and Ethan, my son, enjoy Survivor as well. When we recently watched the first episode of Survivor 43, Robyn shouted out, “Stop! Did you see that?”, when the show introduced a new contestant.
I looked at Robyn and said, “What? I missed it.” I then hit rewind. There, on the screen, I saw the name “Mike Gabler”. Next to his name, we saw the words, “Heart Valve Specialist”.
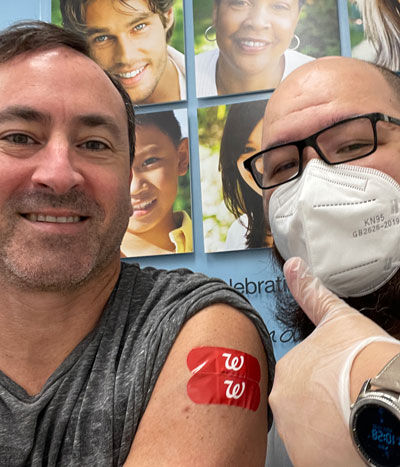
Yes, I Did Get the Bivalent Omicron COVID-19 Booster
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: October 8, 2022
I’ve received several patient questions about whether-or-not I got the bivalent COVID-19 booster. As you can see in the picture below, the answer to that question is yes.
Artivion Stops PROACT Xa Clinical Trial Evaluating On-X Mechanical Valve With Apixaban
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: November 29, 2022
Artivion has stopped the PROACT Xa Clinical Trial evaluating the safety-and-effectiveness of the On-X mechanical valve with apixaban as a blood thinner to prevent clotting. The PROACT Xa clinical trial was designed to evaluate whether patients could safely receive an On-X mechanical valve without the lifelong monitoring requirements of warfain, the only approved blood thinner for mechanical valves.

Ginny, Lisa & Randy Celebrate Their Fixed Hearts, Dr. Gillinov & Our Community!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: October 3, 2022
The patient stories in our community just keep getting better-and-better.
For example, a huge smile just crossed my face as I opened this email from Ginny Turner, a mitral valve patient. Here is what Ginny wrote to Dr. Marc Gillinov, her surgeon, and me:
Hi Dr. Gillinov and Adam,
Look what happened yesterday at a quaint lunch spot just outside of Austin, Texas!

“Can I Get Robotic Mitral Valve Surgery? Or, Do I Need A MitraClip?” asks Bodybuilder Rich
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Joanna Chikwe, MD, Chair of Cardiac Surgery at Cedars-Sinai Medical Center
Published: September 22, 2022
I just received a great question from Rich about mitral valve surgery. In his email, Rich asks, “Hi Adam, I’m a 63-year-old male who competes in natural bodybuilding. Three years ago, I had a mechanical aortic valve replacement. Now, I have severe mitral regurgitation with mild atrium dilation. I have only mild symptoms such as an occasional palpitation. Can I get the mitral valve repaired with a robotic procedure, or is the MitraClip the protocol given my risk factor?”
To provide Rich an expert response, I contacted Dr. Joanna Chikwe, the Chair of Cardiac Surgery at Cedars-Sinai Medical Center, who specializes in mitral valve surgery. As you may know, Dr. Chikwe has performed many successful mitral valve operations on patients in our community including Wendy Spector, Leila Saedi and Scott Wallace.
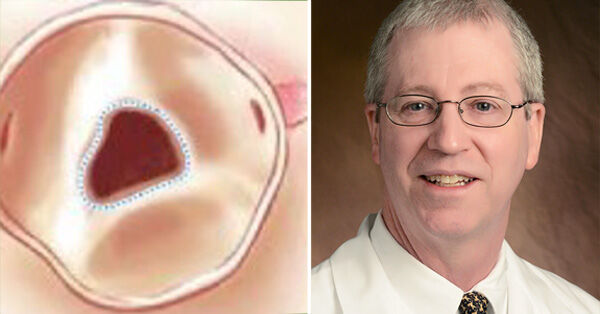
“What About Unicuspid Aortic Valves?” asks Leslie
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 20, 2022
I just received several interesting questions from Leslie about unicuspid aortic valves. She emailed me, “Hi Adam – What can you tell me about unicuspid aortic valves? How are they treated? Are they genetic? If so, should I have my family screened?”
To answer Leslie’s questions about this valvular defect in which the aortic valve has only one leaflet, I was lucky to interview Dr. Samuel Pollock, a leading cardiac surgeon at Baptist Health Louisville, who has performed over 12,000 cardiac procedures.
Click here to watch my interview with Dr. Pollock about unicuspid aortic valves.
In Philippines, Lilian Gets “Second Chance At Life” After Double Mechanical Valve Replacement
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 12, 2022
The patient success stories in our community are downright wonderful. For example, I just received this inspirational email from Lilian Pena of the Philippines which reads:
Hello Adam, I am so grateful that I found your website and can interact with patients from all over the world in the community section. So you know, I suffered from anxiety the moment I discovered that I needed to undergo open heart surgery. Now, I am 6 months post-op after a double mechanical valve replacement. I received two mechanical heart valves from St. Jude Medical (which is now Abbott).
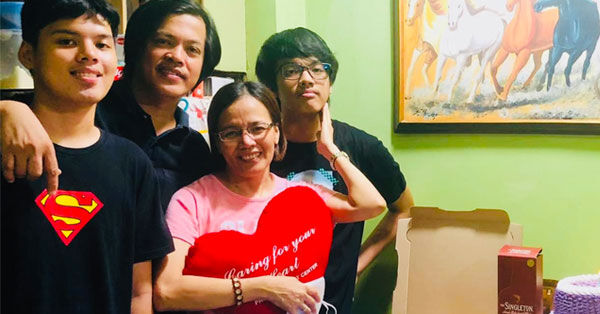
Cardiologist Q&A: What Should You Know About Heart Valve Clinical Trials in 2022?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 7, 2022
In case you missed it… I just posted a very interesting interview transcript with Dr. Samir Kapadia, Chairman of Cardiology at Cleveland Clinic.
Click here to read “Heart Valve Clinical Trials: What Should Patients Know?”.
Many thanks to Dr. Samir Kapadia for sharing his clinical experiences and research with our community. I also want thank Cleveland Clinic for taking such great care of our patients.
Keep on tickin!
Adam
Off Topic: Cool Down With a Genuine Disney Pineapple Dole Whip at Home!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 7, 2022
This is way off-topic… But, hopefully helpful and maybe even fun!
Like many parts of the planet, this summer has been really hot in Southern California where I live. Recently, however, Robyn (my wife), Ethan (my son), and I decided to brave the heat and go to Disneyland in Anaheim, California.

Baptist Health Louisville Joins Our Community!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 6, 2022
I am very excited to announce that Baptist Health Louisville just became the newest sponsor of HeartValveSurgery.com.

Patient Inspiration: Meet a Dog Who Learned to Walk Like a Human
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 29, 2022
It is VERY common for patients diagnosed with heart valve disease to feel alone, confused and frustrated. I can personally remember those and other emotions when my cardiologist said to me, “You need a new heart valve. And, you need it soon.”
As I learned about the safe-and-effective treatment options for my bicuspid aortic valve, my fear began to transform into something much more positive. In particular, I became inspired by many patient success stories that I found online.
Speaking of inspiration, I wanted to share this story about Dexter, an extraordinary dog from Colorado. As you will see, Dexter exemplifies the cliche, “It’s not how many times you get knocked down that counts. But, how many times you get back up.”
Thanks for the inspiration Dexter!!! You truly turned a lemon into lemonade!!!
Keep on tickin!
Adam
Patient Email: “Are Ross Procedure Patients at Higher Risk for Endocarditis?” asks Sara
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 26, 2022
I just received a fantastic question from Sara, a Ross Procedure patient, in response to an article about endocarditis and heart valve disease featuring comments from Dr. David Kaczorowski, a leading cardiac surgeon from UPMC. Her question is about the statement, “If you have an acquired valve disease, artificial heart valve, congenital heart disease, or have a history of valvular disease, monitoring your health for endocarditis symptoms is especially important.”
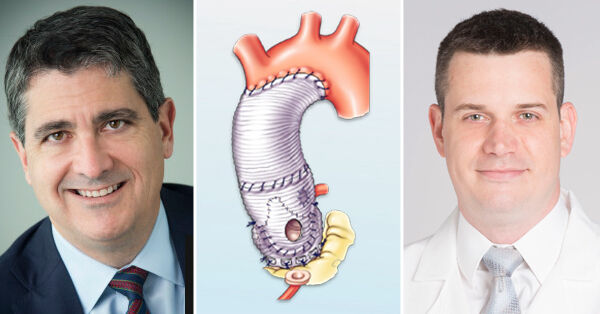
Valve Sparing Aortic Root Replacement vs. Bentall Procedure: What Should Patients Know?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 23, 2022
Patients with leaking aortic valves and aortic aneurysms are often confused about the treatment options available to them. To learn more about the different therapies available to these patients, we were very fortunate to film a “Surgeon Roundtable” with Dr. Eric Roselli and Dr. Marijan Koprivanac of the Cleveland Clinic. In this video, Drs. Roselli and Koprivanac, two leading cardiac surgeons who specialize in aortic valve surgery, share valuable insights specific to Valve Sparing Aortic Root Replacement and the Bentall Procedure.
Click here to watch “Surgeon Roundtable: Aortic Root Surgery for Aortic Valve Patients”.
Many thanks to Dr. Roselli and Dr. Koprivanac for sharing their clinical insights and research with our patient community. I would also like to thank the entire Cleveland Clinic team for taking such great care of heart valve patients!
Keep on tickin!
Adam
Yes, You Can Get Life Insurance After Heart Surgery! Call Gordon Conwell!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: July 12, 2025
Since launching HeartValveSurgery.com in 2006, I’ve received many patient questions about getting life insurance after heart surgery. I have also learned the struggles and challenges that patients can experience trying to get life insurance after a heart valve repair or a heart valve replacement operation.
For these reasons, I am very excited to share that Gordon Conwell, a heart surgery patient from our community, has offered his excellent services to help you get life insurance following heart valve surgery.

Dilated Aortic Root Progression: A Concern for Desmond?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: November 24, 2025
I recently jumped on a Zoom with Desmond, a 33-year-old patient from Ireland who was just diagnosed with a dilated aortic root. Given the life-threatening concerns of aortic aneurysms, Desmond had several important questions. One of those questions was, “Will my dilated aortic root progress to need surgery?”

To provide Desmond an expert opinion, I was very lucky to interview Dr. Luis Castro about this very sensitive topic. As you may know, Dr. Castro is a long-time supporter of this website who has successfully treated over 200 heart valve patients from our community. Here is Dr. Castro’s response to Desmond’s question:
Continue reading this post »
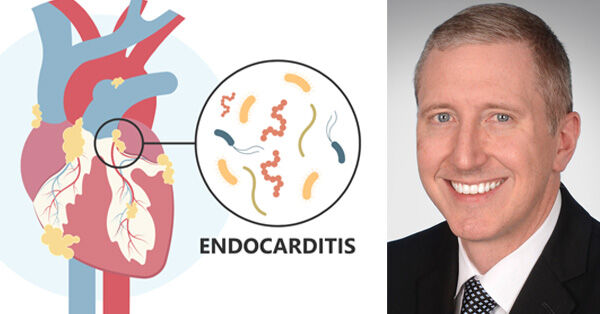
Heart Health Awareness: Endocarditis & Your Heart Valves
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 16, 2022
For patients diagnosed with endocarditis, a dangerous infection that can cause severe heart valve disease, I just posted a new article, Endocarditis: Top 7 Facts People Should Know. In this article, Dr. David Kaczorowski, Surgical Director of the UPMC Heart Transplant Program, provides several insights to help patients in our community.
Click here to read our new article about endocarditis and heart valve disease.
Keep on tickin!
Adam
Email Bag: “What About Stroke Risk, TAVR and Age?” asks Jeff
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 16, 2022
As a follow-up to our recent post about stroke risk, transcatheter aortic valve replacement (TAVR) and cerebral protection, I just received an interesting question from Jeff.

Jeff asked me, “Hi Adam – I am curious if there is a correlation between age and stroke risk when having a TAVR procedure. My father and father in-law both had TAVR procedures within 6 months of each other. They were 89 and 91 respectively. Both sustained transient ischemic attacks (TIAs) within a few weeks following the procedure. My father sustained several TIAs which eventually effected his ability to swallow which resulted in his recent passing. My father in-law is now doing well. Before this article, we were feeling this was not coincidental and this confirmed our suspicions. At no time did either doctor mention inherent stroke risks with TAVR. Thanks for your diligent work in this field which has shed so much light for so many people.”