Adam's Heart Valve Surgery Blog – Page 21
HeartValveSurgery.com Facebook Page Reaches 300,000 Patient & Caregiver Members!
By Adam Pick on October 9, 2019
Unexpected and wonderful!!!
Thanks to your extraordinary support and your “Likes”, I am happy to announce that the HeartValveSurgery.com Facebook page just reached 300,000 members.
“Is Congestive Heart Failure Common After Heart Valve Surgery?” asks Shae
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Craig Smith, MD, Chief of Cardiac Surgery, NewYork-Presbyterian / Columbia University Medical Center
Page Last Updated: June 7, 2025
I just received a great question from Shae, a patient, about congestive heart failure after heart valve surgery.
Shae writes to me, “Hi Adam – How often is it that patients develop congestive heart failure years after having the mitral valve replaced (with a cow valve) and having the tricuspid valve fixed? I had my valves fixed and replaced in 2012. Now, I just had a surprise diagnosis of congestive heart failure (CHF). Apparently, doctors know this can happen but I was never informed about this.”
Clinical Trial Update: TRILUMINATE Launches to Rescue “Forgotten” Tricuspid Valve
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: September 9, 2019
Big, big, big news!
Earlier today, Abbott announced the launch of the world’s first pivotal clinical trial for the catheter-based treatment of tricuspid valve regurgitation. The trial, which is called TRILUMINATE, will evaluate the safety and effectiveness of the TriClip transcatheter valve repair system for leaky tricuspid valves. The TriClip does not require an incision to the patient’s sternum or ribs.

Patient Advice to a Doctor?
By Adam Pick on September 6, 2019
As heart disease patients, we receive advice – from our friends, from our family and, most importantly, from our medical team.
But… What advice can patients give their doctors to help us through the surgical process?
I found the answer when I came across the Facebook post below. After reading “Advice from a Patient”, I smiled and thought, “Wow! That is fantastic, authentic, true and completely accurate”.
So you know, this was posted by Dr. Sloane Guy, a robotic mitral valve specialist, who I have been fortunate to work with for several years. How great! A surgeon sharing this with other surgeons!

Great, right?
Keep on tickin!
Adam
Why Did 50 Patients Get a Standing Ovation at “Patient Experience 2019” at Edwards Lifesciences?
By Adam Pick on August 6, 2019 - This blog is sponsored by Edwards Lifesciences.
Something special recently happened! More than 50 patients and their care partners traveled to Edwards Lifesciences, a leading heart valve manufacturer in Irvine, California, to meet each other, to share their stories and drive helpful insights for Edwards, and to inspire action within our community – the heart valve patient community.
The event, which was previously called “Patient Day”, is now called… “The Patient Experience”. Luckily, Edwards hired us to film the wonderful moments of this unique event that included:
- Meet-and-greets with the heart valve assembly teams
- A look at Edwards’ 60+ years of pioneering work in structural heart disease and critical care technology
- Panel and group discussions
- A campus and manufacturing tour including Edwards’ Heart Valve Museum
One of my favorite parts of the day was watching patients meet the Edwards employees who actually hand-crafted their individual heart valves.
Ready to see what happened at Patient Experience 2019? Watch the video below…
(This video was sponsored by Edwards Lifesciences.)
Tennis Enthusiast, John Persinger, Celebrates Surgeon with “Team Gerdisch” T-Shirts!
By Adam Pick on August 6, 2019
Shortly after sharing this post about a cow valve replacement t-shirt, our Facebook page went bonkers with over 1,600 Facebook Likes.
Then, my inbox swelled with questions about where to buy the t-shirt. Thankfully, the actual t-shirt designer emailed me a link to his Amazon store. Next… Back on Facebook, I started seeing bunches of new t-shirt designs for patients commemorating their heart valve surgery. It’s been so fun to see our community come together like this!

Phil Can Breathe Freely Thanks to the MitraClip!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: August 1, 2019
The patient story of Phil Yalowitz is very personal for me.
A retired urologist, who spent many years practicing at Cedars-Sinai in Los Angeles, Phil is my dad’s cousin. So you know, my dad and Phil grew up together on the south side of Chicago and moved to Los Angeles in the 1970s to pursue their interest in medicine. Phil and my dad had a special bond. They acted and laughed together like brothers, so I always considered Phil my uncle.

Susan & Her INSPIRIS RESILIA Valve Go Viral!
By Adam Pick on August 1, 2019
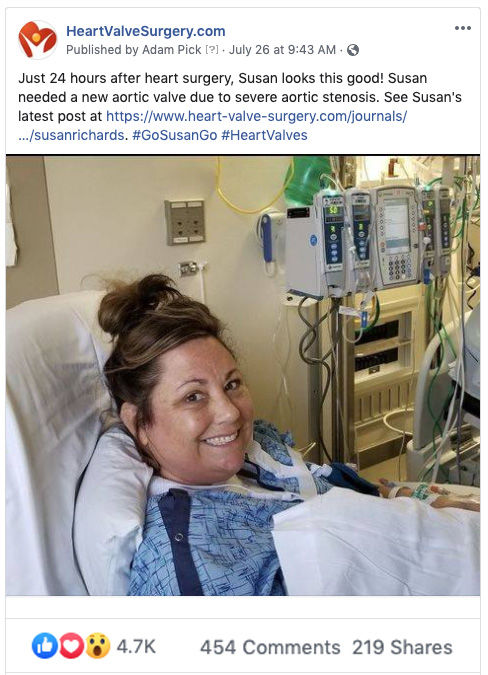
The support and the encouragement that the patients in our community provide each other is simply amazing!
For example, I recently posted a post-op picture of Susan Richards at our Facebook page. As you may know, Susan recently received a new INSPIRIS RESILIA aortic valve due to a bicuspid aortic valve and aortic stenosis. Within seconds of posting her picture, the patients at Facebook rallied around Susan. As you can see below, Susan’s photo received over 4,700 Likes, 454 Comments and 219 Timeline Shares!
No More “Walking Time Bomb” for Tom After Valve-Sparing Aortic Root Replacement
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Chris Malaisrie, MD, Northwestern Medicine
Published: July 12, 2019
Being diagnosed with severe heart disease can be incredibly dislocating for patients, their family and friends. That dislocation is often amplified when the diagnosis is unexpected and the patient is asymptomatic.
Tom Tansor – a father, husband and little league coach from Chicago – describes the unexpected and anxious experience of being diagnosed with a severe aortic aneurysm as feeling like a “walking time bomb”. Tom knew the situation was bad. Tom knew the aneurysm needed to be replaced. But, after meeting with Dr. Chris Malaisrie, Tom was hopeful he could keep his own aortic valve in a complex procedure known as a “valve-sparing aortic root replacement”.
This is Tom’s story…
11 Weeks After TAVR, Mick Jagger Wows 60,000 Fans in Chicago!!!
By Adam Pick on June 25, 2019
It’s been 11 quick weeks since Mick Jagger had a transcatheter aortic valve replacement (TAVR) to treat severe aortic stenosis, a deadly form of heart disease that is under-diagnosed and under-treated.
During his recovery, Mick has been seen walking in Central Park and practicing his infamous dance moves in an empty studio. However… On Friday night, Mick demonstrated – in front of 60,000 people – just how transformative non-invasive TAVR can be. That’s right. Mick, 75, took to the stage for the first time since his TAVR as the Rolling Stones’ 2019 No Filter tour kicked-off at Chicago’s Soldier Field.

Move Over Taylor Swift! David Sets New Fashion Trend!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: January 10, 2026
Ya just gotta see it… To love it.
Here is David Russ modeling a new t-shirt that is setting fashion trends from Milan to Paris to Los Angeles. That’s right. After his aortic valve replacement by Dr. Kevin Accola at AdventHealth, David took to Facebook to show off a fantastic, post-op smile and an awesome t-shirt featuring a cow standing on top of a heart rhythm.

“Every Heartbeat Matters” to Impact 1.5 Million Underserved People! Go Amanda!
By Adam Pick on June 5, 2019
I love hearing about great people at responsible companies doing extraordinary things!
That said… I want…. I need… I must… Congratulate Amanda Fowler, the Executive Director of the Edwards Lifesciences Foundation, for leading the Every Heartbeat Matters charitable initiative. This global campaign, which involves the education, the screening, and the treatment of heart valve disease is on track to reach 1.5 million underserved people by 2020. The original estimate was 1 million people by 2020.

Screening Patients in the Dominican Republic with Empowering Action
Reflecting on this wonderful achievement, Amanda shared, “Since the Every Heartbeat Matters initiative began five years ago, we have made substantial progress in building a global community that is addressing the burden of heart valve disease for underserved people. This year, we plan to continue growing our giving focus on Every Heartbeat Matters and deepening our partners’ impact with the engagement of our talented and dedicated employees around the world.”
Bicuspid Aortic Valve Patient Symposium Announced for June 12 in Chicago!
By Adam Pick on May 28, 2019
Mark your calendars!
I just learned there is a Bicuspid Aortic Valve Symposium for patients happening in Chicago, Illinois on Wednesday, June 12 from 6-8pm at Northwestern Memorial Hospital.
During this special live event, you will learn about the latest bicuspid aortic valve research and treatment options from leading doctors and scientists including Dr. Paul Fedak, Dr. Joshua Robinson, Dr. Chris Malaisre, Dr. Jyothi Puthumana and Dr. Michael Markl.
2019 Atrial Fibrillation Patient Conference Announced!
By Adam Pick on May 28, 2019
As up to 35% of patients with heart valve disease are diagnosed with atrial fibrillation, I wanted to make sure you knew about the upcoming “Get in Rhythm! Stay in Rhythm” conference to be held in Dallas, Texas on August 9 to August 11.
This patient conference is hosted by StopAFib.org, a great patient education website managed by Melanie True Hills, an extraordinary patient advocate. During the event, you will learn the most up-to-date research and treatment approaches that may help you get rid of AFib!
Mick Jagger Dances 6 Weeks After TAVR on Instagram
By Adam Pick on May 22, 2019
Ya gotta love this…
Just 6 weeks after transcatheter aortic valve replacement surgery, Mick Jagger posts this video at Instagram. As you will see in the video, Jagger is strutting all the great dance moves he has entertained us with for the past 57 years as the lead singer of The Rolling Stones.
Congratulations to Dr. Vaughn Starnes, My Surgeon, For Becoming the 100th President of the AATS!
By Adam Pick on May 18, 2019
As one of his many patients, I am excited to announce that Dr. Vaughn Starnes just became the 100th President of the American Association for Thoracic Surgery (AATS). Doctor Starnes succeeded another celebrated surgeon here at HeartValveSurgery.com, Dr. David Adams, at the recent AATS Meeting in Toronto, Canada.
Dr. Starnes is more than a heart valve specialist… He’s a heart valve guru!
He performs complex surgery on both adults and children. Some of his former patients include Arnold Schwarzenegger, Max Page and Jimmy Kimmel’s son, Billy.

Dr. Starnes practices here in my home town of Los Angeles. At the Keck School of Medicine of USC, Dr. Starnes is the Chair of the Department of Surgery. He is also the Co-Director of the Heart Institute at Children’s Hospital Los Angeles. Under his leadership, USC surgeons have conducted more than 50,000 adult and pediatric open heart surgeries to treat heart valves, perform coronary artery bypass grafts, and to repair complex adult and congenital heart defects.
Yoga Enthusiast, Jean Frank, Is Our 1st Low-Risk TAVR Patient Success Story!
By Adam Pick on May 16, 2019
With all the great results coming out about the low-risk TAVR clinical trials, I am very excited to share the patient success story of Jean Frank.
Jean, who is from Island Lake, Illinois, suffered from severe aortic stenosis symptoms including shortness of breath and fatigue. As her aortic stenosis progressed, Jean often became dizzy. Ultimately, Jean could no longer enjoy yoga because her valve had calcified. Then, Jean heard about the low-risk TAVR clinical trial conducted by Dr. Charles Davidson and Dr. Chris Malaisrie at Northwestern Medicine in Chicago, Illinois, a sponsor of HeartValveSurgey.com.
This is Jean’s story…
True or False: 70% of Patients Use Online Reviews to Select Heart Surgeons
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: December 30, 2024
Last week… In my heart valve surgery newsletter, I asked our patient community a very simple question, “Would you recommend your heart surgeon?”
If so, patients could instantly provide their reviews at our online surgeon recommendation form. Ultimately, the patient recommendations would help current and future patients find and learn about their potential heart surgeons.
I was not prepared for what happened next….

Within hours, I received 400+ surgeon recommendations from patients all over the world!!! The patient reviews are still coming in.
As I’m writing this, I just received a patient recommendation for Dr. Marc Gillinov at the Cleveland Clinic and Dr. David Adams at Mount Sinai Hospital. Next up, I’m getting ready to post this question at our Facebook page that has over 285,000 members.
If you’re curious, our top three heart surgeons to receive patient reviews are:
Yum! A Healthy Lemon & Herb Rotisserie Chicken Recipe!
By Adam Pick on May 16, 2019
I don’t know about you… But, I can’t leave Costco without getting a hot rotisserie chicken. And, it’s not just Costco. I’m into all types of rotisserie chicken from different grocery stores and ethnic restaurants. I simply love the taste and different flavors.
The other day I thought, “Hmmm… Can I make a rotisserie chicken?”
So you know, I never used a rotisserie before. But, I remembered that my barbecue came with a rotisserie kit. I headed out to the garage and found the rotisserie kit which had a little electronic crank, a spit and two forks. Next, I did what Ethan, my 10-year old son, would do. I typed, “Chicken Rotisserie Recipe” into YouTube. Yep! I instantly saw thousands of recipes. However, a video for a “Lemon & Herb Rotisserie Chicken” looked yummy.
With purpose, Robyn and I went to Ralphs, our local grocery store. We got the ingredients. We came home. Then, I went to work.

Will You Recommend Your Heart Surgeon?
By Adam Pick on May 10, 2019
It’s been 10 wonderful years since we launched the Surgeon Finder at HeartValveSurgery.com. You might remember that we launched the Surgeon Finder to quickly help patients locate and research patient-recommended surgeons. In the last three years alone, the Surgeon Finder had over 756,000 page views. Amazing!
To help future patients… My question to patients who already had surgery is, “Will you recommend your heart surgeon?” If so, this is your opportunity to celebrate him or her by posting a review. To post your review, click here!