Valve Clinic Tour: Dr. Adams & Dr. Stelzer Help Trigger Rankings Boost at Mount Sinai Hospital
By Adam Pick on July 27, 2010
When two, leading heart valve surgeons come together at an established cardiac care program, the expectations for success are high.
That said, it shouldn’t surprise you that Dr. David Adams and Dr. Paul Stelzer have transformed this hypothetical situation into reality at The Mount Sinai Hospital in New York City.

Since Dr. Adams took over the program in 2002 and Dr. Stelzer joined the staff in 2007, Mount Sinai’s heart program has soared 21 rankings in U.S. News and World Report’s annual survey of cardiac centers.
Most recently, Mount Sinai jumped 5 places to claim the 13th slot in the 2010 rankings just behind the University of Michigan and Barnes-Jewish Hospital / Washington University.
While these rankings provide independent and objective perspective, I tend to focus on patient success stories as a key indicator for program care. As many of you know, I have received countless patient testimonials for these heart valve specialists since launching this blog.
For these reasons, I was beyond excited when Dr. Adams and Dr. Stelzer invited me to tour Mount Sinai in New York City.
Dr. Stelzer And I Almost Bump Into Each Other…
The tour began at 7:30am when Dr. Stelzer and I simultaneously approached the entryway to Mount Sinai’s cardiac care center. I immediately recognized Dr. Stelzer’s warm smile from his online photos. Dr. Stelzer was already in scrubs and a red pair of Crocs shoes.
Within the heart valve community, Dr. Stelzer is best known for his vast experience with the Ross Procedure, a complex double valve replacement for patients suffering from aortic valve disease. To date, Dr. Stelzer has performed over 475 Ross Procedure surgeries – more than any other surgeon in the United States.
“The Ross Procedure has some great advantages for patients,” Dr. Stelzer said to me. “Interestingly, several surgical centers in Europe consider the Ross as the standard for aortic valve replacement. However, I always leave it up to the patient to make that call.”
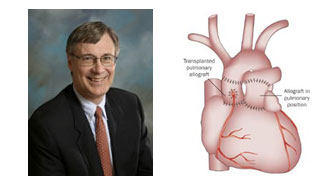
Dr. Paul Stelzer and a Ross Procedure Diagram
While Dr. Stelzer and I chatted about the Ross Procedure, I began to notice a familiar face in my peripheral vision. As I turned to the left, I saw Dr. David Adams, the Chairman of the Department of Cardiothoracic Surgery at Mount Sinai, standing next to me.
As you may know, Dr. Adams is widely known for his research and his clinical concentration on mitral valve repair. In fact, Dr. Adams just released a new book, Carpentier’s Reconstructive Valve Surgery, with heart valve legend, Dr. Alain Carpentier, and Dr. Farzan Filsoufi. Dr. Adams also runs a fantastic website dedicated to mitral valve repair at www.MitralValveRepair.com.
Coffee, Dr. Adams & Patient Education…
When Dr. Stelzer was called to the operating room, Dr. Adams and I sat down for a cup of coffee in the hospital lobby. There, we had an insightful discussion about many topics including patient education. In particular, we discussed the utility of the Internet and other technologies to enhance patient awareness.
“I really believe the web will become even more critical in the future – for patients, for caregivers, for cardiologists and for surgeons,” Dr. Adams said, “I think we have an extraordinary opportunity and responsibility to improve heart valve care through information that patients can apply and easily understand.”
In particular, Dr. Adams and I discussed the current need for patients to better understand critical diagnostic elements and milestones prior to surgery including echocardiography, “watchful waiting” and the American College of Cardiology (ACC) guidelines.
“I want patients to know why they need surgery,” Dr. Adams said to me, “I don’t think patients should enter the O.R. just because their cardiologist or surgeon says, ‘Trust me, I’ve been doing this for 20 years. You need surgery.’”
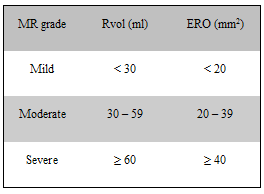
Together, we brainstormed several different possibilities for advancing patient education. In particular, we discussed the possibility of holding an online seminar on the web, or webinar, for patients and caregivers to better understand the diagnostic process.
Mount Sinai & Gift Of Life Nurture Cardiac Care In Developing Regions
Unbeknownst to me, Dr. Adams and I shared similar altruistic goals. Midway through our chat, I learned that Dr. Adams had an explicit interest in expanding cardiac care in developing regions.
For example, in 2009, Dr. Adams traveled to Hue City, Vietnam where he – and 11 other heart doctors, nurses and staff, including Dr. Khanh Nguyen – performed several valve repair surgeries on young patients.
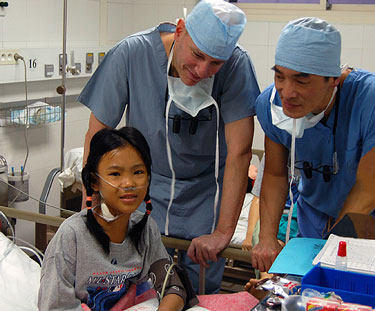
This medical mission was organized by Gift of Life — the same organization that we recently submitted a $5K donation to. Currently, Dr. Adams is planning another medical mission to the Dominican Republic.
In The ICU, I Meet John Cautela & Sherry Grabowski
Following coffee, Dr. Adams took me to the intensive care unit (ICU) where I saw and met several patients recovering from heart surgery. In particular, I was very touched by the story of John Cautela and his wife, Sherry Grabowski. Residents of Boise, Idaho, John had just come through a very complex, re-operation due to a leaking mitral valve replacement.
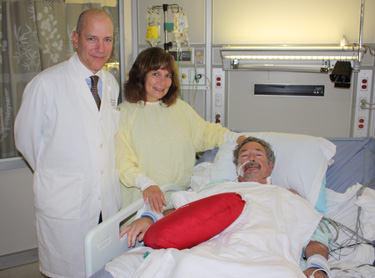
“We had to do John’s surgery in two steps,” Dr. Adam’s told me. “The process of opening his chest took three hours due to heavy scar tissue from prior surgeries in Idaho and California.”
I would later learn from Sherry, who manages the intensive care unit at St. Luke’s Hospital, that John has had five heart surgeries in the past three years.
“Before coming to Mount Sinai, the other doctors told me I should just let my husband go [die],” Sherry quietly shared with me. “But, John has 9 lives… He’s a fighter.”
Next Up… Dr. Stelzer’s Operating Room
As my time with Dr. Adams came to a close, I was invited into Dr. Stelzer’s operating room. There, in scrubs, a surgical mask and a bouffant cap, I watched Dr. Stelzer and his team perform an aortic valve and root replacement surgery. The patient suffered from aortic stenosis due to a bicuspid aortic valve which was severely calcified.
Upon entering the O.R., my visual and auditory senses were highly stimulated.
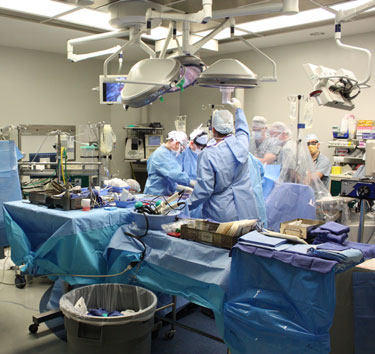
My eyes rapidly bounced from the patient to Dr. Stelzer to the medical professionals that supported this effort. The medical team consisted of two cardiac surgeons, a perfusionist (heart-lung operator), one physician’s assistant, three anesthesiologists, a cardiac nurse and an O.R. surgical technician.
As I approached the patient, I could see that a median sternotomy had been performed and the patient was already on bypass. Doctor Stelzer was in the process of removing the diseased aortic valve.
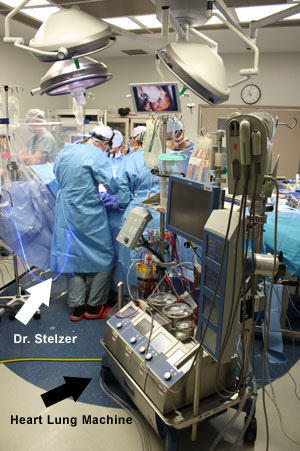
My ears were also stimulated in the operating room. On one hand, I was intrigued by the ongoing communication among Dr. Stelzer and his team. On the other hand, the surgical theater was an epicenter for beeps, blips, slurps and gurgles from the high-tech machines that powered this life-extending operation.
For me, highlights of the procedure included:
- Once the aortic valve was removed, Dr. Stelzer spent a good amount of time removing excess calcium from the inner parts of the heart that could inhibit valvular function going forward.
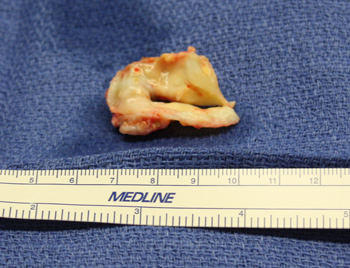
- For this procedure, the patient, who was in his late 40’s, chose to have a tissue valve replacement. As shown below, a porcine valve — the Medtronic Freestyle Bioprosthesis — was selected as the heart valve replacement device.
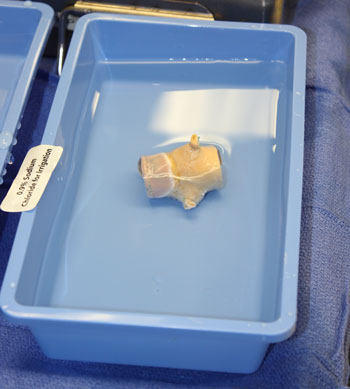
- The patient’s aortic root was also dilated. To prevent the possibility of an aortic aneurysm or aortic dissection, Dr. Stelzer also performed an aortic root replacement using a Dacron aortic graft. The graft was sutured directly onto the aortic valve replacement (see picture below).
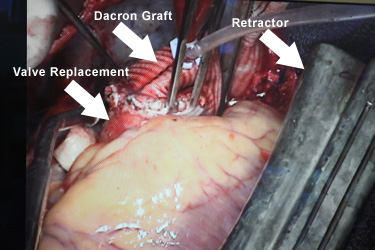
During the 4-hour procedure, I was able to discuss the operation with several members of Dr. Stelzer’s medical team, including Dr. David Reich, the Chair of the Department of Anesthesiology at Mount Sinai. Below, Dr. Reich showed me the pre-operative echocardiogram which showed the calcified leaflets.
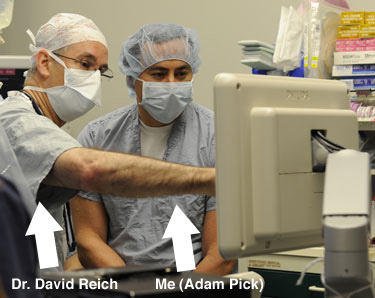
While I learned a lot about cardiac surgery during these discussions, I also learned a lot about the team’s appreciation for Dr. Stelzer.
Towards the end of the surgery, Dr. Joanna Chikwe, an attending cardiac surgeon who operated with Dr. Stelzer, pointed to the monitor and said to me, “I’ve seen this procedure done elsewhere a lot. But, not like Dr. Stelzer. Not as good as Dr. Stelzer, I mean. This is just as you see it in the textbooks… Perfect.”
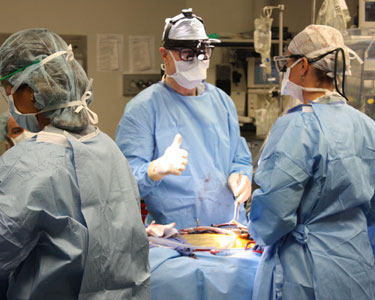
Beyond his surgical competency, Marjorie Leventhal, a cardiac nurse for the past 34 years at Mount Sinai, commented on Dr. Stelzer’s bedside manner. Marjorie said to me, “Dr. Stelzer’s more than a great surgeon, he’s a gentleman and a gentle man with the patients.”
As for the surgery I observed, I would later learn that the patient did not receive any blood transfusions or blood products and was released from the hospital three days after surgery.
Thanks To Mount Sinai!
When I started this blog, I never imagined that I would gain direct access to leading heart surgeons and cardiac care centers. That said, I would like to thank Dr. David Adams and Dr. Paul Stelzer for their support of my book and this website.
I would also like to thank everyone I met at Mount Sinai – both the medical staff and the administration teams.
In particular, a special thanks goes to Gideon Sims, Senior Director, Information Technology, who arranged my visit to Mount Sinai. So you know, Gideon has been incredibly helpful during the development and launch of the Heart Valve Surgeon Database and Heart Valve Journals.
Keep on tickin!
Adam
|
Shelby Hudgens says on July 27th, 2010 at 1:21 pm |
|
I’ve never met Dr. Stelzer, but he was instrumental in my decision to get a Ross Procedure. Faced with surgery, I spent a great deal of time researching doctors and hospitals. I sent him an email, and in less than one hour he had replied and answered every question I had. Although he didn’t perform my surgery, he knew my surgeon and could recommend him highly. His input was extremely helpful and comforting to me at a most difficult time. |
 |
|
al chameides says on July 27th, 2010 at 1:31 pm |
|
good article |
 |
|
Fran Zilko says on July 27th, 2010 at 1:53 pm |
|
Adam, thank you so much for bringing us this information. Although I had my surgery in March, I continue to follow what great doctors and hospitals can accomplish. By the way, Dr Gillinov at the Cleveland Clinic was my surgeon. Can’t say enough great things about him. |
 |
|
Eric Desbonnet says on July 27th, 2010 at 2:20 pm |
|
I had my mitral valve surgery at Mt Sinai in 10/09 by Dr. Adams. Nine months later I feel great and and have had no complications at all. I cannot say enough in the praise of Dr. Adams, the Heart Program at Mt. Sinai and the hospital itself. |
 |
|
Cindy says on July 27th, 2010 at 3:09 pm |
|
Hi Adam, |
 |
|
R. P. says on July 28th, 2010 at 2:25 am |
|
Dr. Khanh Nguyen was my surgeon(pulmonary valve replaced on 12/03/09 at Mount Sinai)! |
 |
|
Theresa Callanan says on July 28th, 2010 at 11:35 am |
|
I had my mitral repair surgery at Mt. Sinai in March 2010. Dr. Adams was my surgeon, and after meeting with him for my initial consultation, I knew I did not have to look further. Everyone at Mt. Sinai was helpful and kind..it was the best overall experience for a situation I did not want to be in. I had no recovery issues and am feeling great! I would highly recommend Dr. Adams and his team at Mt. Sinai to anyone that needs to undergo open heart surgery….He is a top notch surgeon with an outstanding record. |
 |
|
Mary Ferraro says on August 15th, 2010 at 12:21 am |
|
Dr. Adams repaired my mitral valve 10/28/08 and it was a huge success. That entire team is off-scale great. So glad to see 2 of my favorite people (Adam & Dr. Adams) meet and talk. Wonderful story. |
 |
|
Nancy Landers- FL says on August 29th, 2010 at 7:23 pm |
|
Dear Adam: I want to thank you so much for writing your book…I purchased it back in the Spring 2010 and it is now in the hands of my 3 sons, as they will be helping me through my surgery, I hope! It was so good to read all about your surgery and what to expect, but the one thing that I am scared to death about is, being put on the heart/lung machine and awaking with the tube down my throat. I am severly claustraphobic, especially when it comes to my mouth and breathing. I am petrified. I am ok with everything else, but not that. I have severe mitral valve prolapse with regurgitation. I was diagnosed in Jan of 2010 and had the echocardiogram and found out the beginning of March how bad it was. I have crappy insurance and it will not insure any cardiac surgeon in the country. I am having a hard time finding someplace to have it. I would love to have it at Mount Sinai, as two of my 3 sons live in North Jersey and I need them and their wives to help me recover. Since you have been there recently, do you know if they have charity care? I have done my research on the internet and found that I could have it at Mount Sinai or my Florida cardiologist’s almamater – NY Presbyterian/Columbia Hospital. Or Deborah Heart & Lung Hospital in Central NJ, or Thomas Jefferson Hospital in Phila. My other location is Jacksonville, Florida’s Mayo Clinic. This insurance is giving me a problem. I am poor and only have enough money to live on. Is there any suggestions that you can give me on all of this? Thank you and again thank you for writing the book, this is why my kids are reading it!! It was so detailed and informative. Nancy Landers, Hudson, Fl – which is north of Tampa. |
 |
|
Eder Avallone says on September 16th, 2010 at 9:29 am |
|
My name is Eder. Iam 47 y.o. and Iam from Brazil. Last month we find an ascending aortic aneurysms, just after my heart. My aortc valve is bicuspid. The aneurysms was 76 milimiters big. My surgeon was Mr. Stevan Krieger Martins, at Bandeirantes Hospital in São Paulo – Brazil. I had to open my chest. They remove the aneurusm and put dacron. My bicuspid valve was preserved, because Dr. Stevan said that it was in good conditions. Maybe in several years I have to change my valve to a mechanic one. Please, give me your opinion about my problem and my valve. I am on recovery and I would not like to make another surgery. I thank you so much for your attention. |
 |
|
Tim P says on September 21st, 2010 at 5:46 pm |
|
Nice writeup and photos. In Jan this year, Dr Stelzer replaced my a-valve &repaired the mitral valve. Had a severe case of endocarditis. This man saved my life |
 |
|
Meredith Torchio-Andresen says on October 15th, 2010 at 8:51 am |
|
9 years ago today, October 15,2001, I had a Ross Procedure done at Beth Israel Hospital by Dr Paul Stelzer. I was Ross Procedure #306 for Dr. Stelzer on that day. What a great man with a great God given talent to master such a extensive surgery. I’m not on any medicine & am in the best of health with no limitations. I tell everyone about him possibly needs aortic valve replacement. I’m so glad my cardiologist recommended this procedure & Dr Stelzer to me! Happy Re-Birthday to me! Meredith Torchio Andresen |
 |
|
Lyndon Peck says on November 2nd, 2010 at 12:49 pm |
|
I just found this article, and have read numerous other articles and forum posts all within the past several months now – I’m one day home from a visit to Dr Stelzer down at Mt Sinai Hospital. Last Wednesday I became his 480th Ross procedure. I just wanted to let everyone know that I am certainly new to all of this; being my first surgery ever at 35 yrs old- but Dr Stelzer is the nicest person you’ll meet and excellent at what he does. I’m can honestly say I had no idea I’d feel this well only 6 days after surgery. I cannot express my thanks enough! Lyndon Peck |
 |













