Adam's Heart Valve Surgery Blog – Page 2
Surgeon Spotlight: Dr. Gyu Gang Gets His 200th Patient Testimonial!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: March 26, 2025
I am excited to share that Dr. Gyu Gang, a leading heart valve surgeon at the Northwestern Medicine Bluhm Cardiovascular Institute just received his 200th patient review at HeartValveSurgery.com!
This is a wonderful accomplishment for Dr. Gang who provides advanced valvular therapies to patients at Central DuPage Hospital and Delnor Hospital in the western suburbs of Chicago.

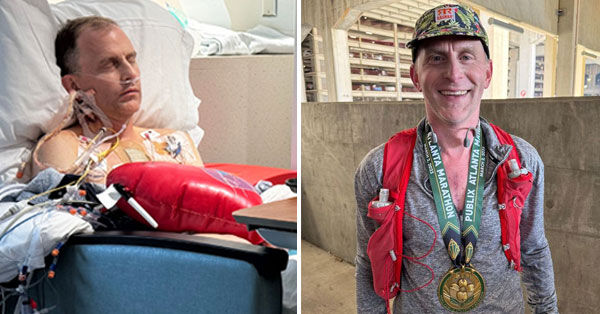
123 Days After Heart Valve Surgery, Justin Runs a Marathon!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: March 20, 2025
I’ve said it before and I look forward to saying it again… The patient success stories from the courageous members in our community are downright extraordinary.
This time, I am happy to share the story of Justin Chamblee, a heart valve patient from Georgia.
Inside Access: The Ross Procedure Wet Lab at USC
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: April 7, 2025
In case you missed it… Earlier today, we had special access to the Ross Procedure Training Course taught by Dr. Vaughn Starnes and Dr. Craig Baker. As you may know, Dr. Starnes performed the Ross Procedure on me in 2005. Nearly 20 years later, my heart is doing perfect and I do not take any medications or blood thinners.
This mazing event that was hosted by LifeNet Health, a special organization that provides the pulmonary donor valves used during the Ross Procedure.
Unfortunately, the video below was deleted following a Facebook Live policy change, effective February 19, 2025, which Facebook did not make us aware of. Prior to deletion, that Facebook Live video had been viewed over 87,000 times.)

Ross Procedure Patient Education Center Launches Now!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: March 12, 2025
As many of you know, I had a Ross Procedure performed by Dr. Vaughn Starnes in 2005. Since then, nearly 20 years ago, I have had no re-operations and I am not on any medications including blood thinners. While the Ross Procedure is not for everybody, I am getting many patient questions about this advanced form of aortic valve surgery given new research about patients who are experiencing (i) a return to normal life expectancy and (ii) long-term durability going out to the third post-operative decade.
For this reason, I am happy to announce that we just launched a new “Ross Procedure Patient Education Center” that was designed to educate patients about the Ross Procedure. Thankfully, many world-renowned Ross Procedure surgeons helped me build this educational resource.
Click here to experience the new Ross Procedure Patient Education Center.
NEW 3PM EST START TIME: Join Me LIVE In A Ross Procedure Training Course
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: March 7, 2025
Ready to experience something extraordinary?
This Friday, March 7, I will attend a live Ross Procedure Training Course taught by Dr. Vaughn Starnes, the Surgeon-in-Chief at Keck Medicine of USC. (So you know, Dr. Starnes performed a Ross Procedure on me in 2005. Since then, nearly 20 years later, my heart is perfect. I’ve had no re-operations. I am not on any medications or blood thinners. And, I am SCUBA diving again with my son.)
Here’s the fun part… Using Facebook Live, I’m going to broadcast several key moments from Dr. Starnes’ upcoming training that will include a “Wet Lab” in which cardiac surgeons practice the Ross Procedure using an actual pig heart.
To join me for this live event at Facebook, click here at 3pm EST on Friday, March 7.
After Lifelong Broken Heart, Kevin’s Mojo Returns
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: March 3, 2025
The patient stories in our community touch, move and inspire me. This time, it was the wonderful patient success story of Kevin Hornaday that got me. So you know, Kevin has been a lifelong cardiac patient who was born a cardiac electrical issue. Then, at 12 years of age, his heart broke in a different way when his mother suddenly passed away to a suspected aortic aneurysm.

45 Patient Questions Answered by Dr. Doug Johnston!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Doug Johnston, MD, Chief of Cardiac Surgery, Northwestern Medicine
Page last updated: March 3, 2025
Great news!
During our recent webinar, “6 Expert Tips for Heart Valve Patients”, I received 45 patient questions that we did not have time to answer during the live event.
Imagine my surprise (and thankfulness) when Dr. Doug Johnston, Chief of Cardiac Surgery at Northwestern Medicine and a featured speaker of the webinar, typed up answers to each patient question and asked me to post them to help educate our patient community.

It’s Heart Valve Disease Awareness Day!!!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: February 27, 2025
Today, on Heart Valve Disease Awareness Day, let’s raise awareness to this under-diagnosed disease and celebrate the life-saving heart valve surgery of Daphine, a courageous 12-year old girl from Uganda!

Join 950 Heart Valve Patients On Today’s Webinar!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: February 23, 2025
[Update: Great news! Our patient webinar, “6 Expert Tips for Heart Valve Patients” with Dr. Johnston, Dr. Medina and Dr. Hodges was fantastic. You can watch a video playback of the webinar below or at YouTube. You can also download a free eBook of the “6 Expert Tips for Heart Valve Patients” webinar at this link.]
I’m excited to announce that our LIVE and FREE patient education events continue today, Thursday, February 20th, at 6pm EST, with a special webinar, “6 Expert Tips for Heart Valve Patients”. The featured speakers are world-renowned heart valve experts including Dr. Doug Johnston, Dr. Melissa Medina and Dr. Kevin Hodges from Northwestern Medicine.
Also… During the webinar, an interactive “Questions & Answers” session will enable you to ask the experts your questions about heart valve disease.
Keep on tickin!
Adam
Happy Valentine’s Day From Chicago!!!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: February 14, 2025
As Heart Month continues to raise much-needed awareness to heart disease, I’m excited to be in Chicago today for a special celebration of the 20th Anniversary of the Bluhm Cardiovascular Institute at Northwestern Medicine in Chicago, Illinois.
Many of you know that Northwestern Medicine has provided extraordinary outcomes for over 700 patients of the HeartValveSurgery.com community. Here is a video I just posted from the party with world-renowned heart valve experts and their patients.
Let’s “Go Red” for Women’s Heart Health!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: February 7, 2025
Today, Friday, February 7, you are invited to join our community which is in full support of the “Go Red for Women” campaign. This wonderful initiative was created to raise awareness to women’s heart disease and unite communities that are fighting for the eradication of heart disease and stroke. As you can see below, heart valve experts from all over the United States are showing their support to fight cardiac disease which accounts for 1 in 3 female deaths every year.
That is Dr. Vaughn Starnes, my surgeon and the Surgeon-in-Chief of Keck Medicine of USC, and Dr. Craig Baker, Chief of Cardiac Surgery at Keck Medicine of USC in Los Angeles, California.
Join 300 Patients on Thursday’s Tricuspid Valve Webinar!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Experts: Wilson Szeto, MD and Paul Fiorilli, MD of Penn Medicine
Page Last Updated: February 1, 2025
[Update: Great news! Our patient webinar, “Advances in Tricuspid Valve Therapy” with Dr. Wilson Szeto and Dr. Paul Fiorilli, was fantastic. Click this link to see a video replay of the webinar or download a free copy of the new “Advances in Tricuspid Valve Therapy” eBook.]
I’m excited to announce that our LIVE and FREE patient education events continue Thursday, January 30th, at 6pm EST, with a special webinar, “Advances in Tricuspid Valve Therapy”. The featured speakers are Dr. Wilson Szeto, the Chief of Cardiac Surgery, and Dr. Paul Fiorilli, the Co-Director of the Transcatheter Heart Valve Program, at Penn Medicine.
Baptist Health South Florida Joins Our Community!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: January 16, 2025
I am very excited to announce that Baptist Health South Florida’s Miami Cardiac & Vascular Institute just became the newest sponsor of HeartValveSurgery.com.

Just 24 Hours After TAVR, Rick Says…
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: January 16, 2025
It’s been less than 24 hours since Rick Jerzak’s transcatheter aortic valve replacement (TAVR) and I just received this update from him.

Will You Recommend Your Interventional Cardiologist?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: January 13, 2025
Dear Patients and Friends,
As the use of minimally-invasive transcatheter devices continues to increase, I am getting lots of patient emails asking me, “Who should I go to for TAVR?” and “Which hospitals specialize in TMVR?”. For this reason, I just built a new Interventional Cardiologist Finder for heart valve patients. Similar to our Surgeon Finder, this tool is powered by your patient reviews.
So… My question to you is, “Would you recommend your interventional cardiologist?” If so, this is a great opportunity to celebrate your doctor and help future patients.
Click Here to Post Your Review!
Keep on tickin,
Adam
“What is Aorta Root Carving and Enlargement?” Asks Ellie
Written By: Adam Pick, Patient Advocate & Author
Medical Expert: Dr. Marc Gerdisch, Chief of Cardiac Surgery at Franciscan Health
Published: January 8, 2025
In response to this post about patient outcomes for heart valve reoperations, I received a very interesting question from Ellie about aorta carving and enlargement. In her email, Ellie wrote to me, “Hi Adam – Six months after I had a surgical aortic valve replacement, my medical team told me that the new bovine valve does not fit well. I am also being told that I need a redo with a possible root enlargement to place a larger tissue valve. What should I know about aortic root carving and enlargement?”
My 19th Heart Valve Surgery Anniversary!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: December 19, 2024
It’s hard to believe.
This coming Saturday, December 21, I will celebrate my 19th anniversary of heart valve surgery. I am so incredibly thankful that I had a successful Ross Procedure performed by Dr. Vaughn Starnes at Keck Medicine of USC in Los Angeles. Since my operation, I have had no cardiac issues. None. In fact, at my last echocardiogram, my technician said to me, “This is amazing. Your valves look perfect.”
Dressler’s Syndrome: What Does Steve Want All Patients To Know?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: June 12, 2025
As we have seen many times in our community, patients going through heart valve surgery often turn a metaphorical lemon into lemonade. We “pay it forward” as they say.
For this reason, I wanted to share the story of Steve Deller. Yes, Steve is a heart valve surgery patient. Yes, Steve experienced complications after surgery. And yes, Steve wants to help future patients learn about Dressler’s syndrome.

Join 400 Patients on Today’s Live Webinar With Dr. Emerson & Me!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page last updated: December 12, 2024
[Update: Wonderful news! Our patient webinar, “Minimally-Invasive Heart Valve Surgery” with Dr. Dominic Emerson, was fantastic. To see a video replay of the webinar, click this link. Or, you can download a copy of the new “Minimally-Invasive Heart Valve Surgery” eBook at this link.]
I’m excited to announce that our LIVE and FREE patient education events continue Thursday, December 12th, at 6pm EST, with a special webinar, “Minimally-Invasive Heart Valve Surgery”. The featured speaker is Dr. Dominic Emerson, a leading minimally-invasive cardiac surgeon at Cedars-Sinai Medical Center.
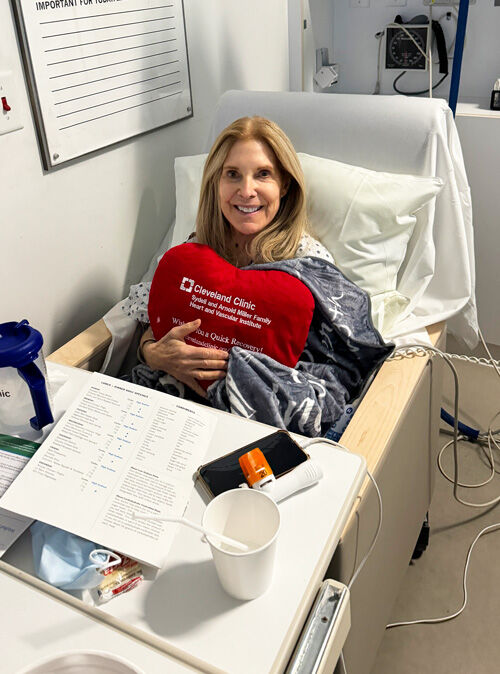
Suzi Goes From Asymptomatic Nerves To Another Dr. Gillinov Success Story!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: December 4, 2024
It is amazing to see the physical, emotional and spiritual transformation that occurs in patients before-and-after heart valve surgery. For example, here is the patient story of Suzi Epstein, an asymptomatic patient who was unexpectedly diagnosed with severe mitral regurgitation.