
Adam’s Heart Valve Surgery Blog
Get the latest news, patient advice and insights about heart valve surgery from Adam Pick, patient, author and website founder
From Palliative Care to a Life-Saving Miracle at Cleveland Clinic: Hannah’s Story
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 29, 2025
In 2020, Hannah Earls underwent a transcatheter aortic valve replacement (TAVR) to treat her severe aortic stenosis. For five years, Hannah lived a stable and fulfilling life. But in 2025, troubling symptoms returned — fluid retention and high blood pressure signaled that something was wrong.
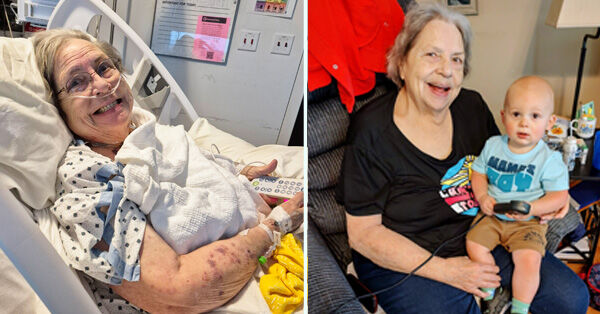
Part II: Elisabeth Completes Half-Marathon with Daughter After Ross Procedure
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 25, 2025
The inspirational patient success stories keep coming in from all over the world!
This time, we have our first “Part 2” of a patient success story from Elisabeth Boylan, a Ross Procedure patient from Quebec. (As you may recall, we initially featured Elisabeth’s efforts to raise heart disease awareness in 2020. Learn more here.)

Northwestern Medicine’s Bluhm Cardiovascular Institute Achieves 100th Ross Procedure!
Written By: Allison DeMajistre, BSN, RN, CCRN
Reviewed By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 21, 2025
Dr. Chris Malaisrie, and Dr. Christopher Mehta, cardiac surgeons at Northwestern Medicine Bluhm Cardiovascular Institute specialize in the treatment of aortic valve disease. Along with their team of experts at Northwestern Memorial Hospital, they recently performed their 100th successful Ross Procedure. “We’re happy to report that Northwestern Memorial Hospital has a 100 percent in-hospital survival rate for this complex procedure in addition to long-term durability,” said Dr. Malaisrie.
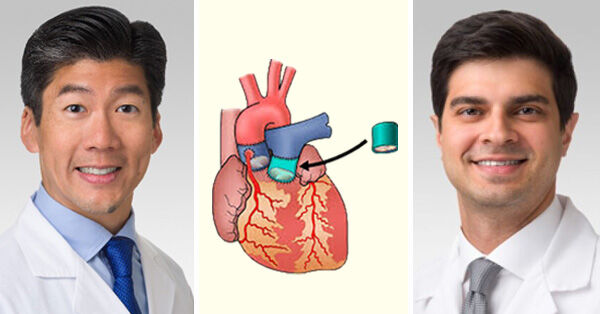
(Source: Northwestern Medicine)
Heart Warrior: Therese’s 50-Year Journey With Heart Valve Disease
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 12, 2025
If there is one thing that our patient community has learned over the years, it is that patients and their medical teams must consider the lifetime management of heart valve disease. While there are many great medical advances and treatment options for patients, the reality is that there are no guarantees that a heart valve repair or replacement will last forever.
As a result, patients may need a second, third, fourth or even fifth heart valve surgery. For example, I just heard from Therese Tilton, a heart valve patient who has been dealing with heart valve issues for over 50 years. This is her story…

Providence Little Company of Mary Medical Center Torrance Joins Our Community!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 10, 2025
I am very excited to announce that Providence Little Company of Mary Medical Center Torrance, a Keck School of Medicine of USC partner, just became the newest sponsor of HeartValveSurgery.com!

Patient Q&A: 4 Days After Jim’s Mitral Valve Repair
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Raymond Singer, MD, Jefferson Health Montgomery Hospital
Published: June 7, 2025
When Jim Makovetz moved to East Norrtion, Pennsylvania in July 2024, he began feeling unwell. After visiting a local urgent care, Jim learned that he had high blood pressure. Then, it was recommended that Jim get a transesophageal echocardiogram. The tests revealed severe mitral valve regurgitation due to Barlow’s syndrome, a condition Jim had no noticeable symptoms of at the time.
Deborah Heart and Lung Center Joins Our Community!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 2, 2025
I am thrilled to share that Deborah Heart and Lung Center has become the newest sponsor of HeartValveSurgery.com!

U2’s Bono Shares Deep Insights of Heart Surgery in “Stories of Surrender”
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: June 1, 2025
U2 is my favorite band. And, Bono is one of my heroes.
I’m not alone. For millions around the world, Bono is more than just the iconic frontman of U2 — he’s a voice for justice, humanity, and now, heart valve patients. Diagnosed with severe aortic valve disease and an aortic aneurysm, Bono needed emergency heart surgery in 2016. The complex procedure was performed by Dr. David Adams, the Cardiac Surgeon-in-Chief of Mount Sinai Hospital in New York City, who has successfully treated many patients in our community.
Now, Bono is sharing his life in a deeply personal way with his new film “Bono: Stories of Surrender,” that is streaming on Apple TV. Based on his bestselling memoir, Surrender: 40 Songs, One Story, the film explores Bono’s extraordinary journey, his near-death experience with heart disease, and the strength it takes to keep going — in music and in life.
Patient Webinar: Ask Dr. Gerdisch Anything!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: May 30, 2025
[May 30, 2025 Update: Great news! Our patient webinar, “Ask Dr. Gerdisch Anything”, with Dr. Marc Gerdisch was fantastic. You can now watch a video playback of the webinar below. You can also download the free eBook at this link.]
As many of you know, patients can be very confused about their diagnosis, their treatment options, and the lifetime management of heart valve disease.
For that reason, we are hosting a special FREE and LIVE webinar next Thursday, May 29, at 7pm EST. The webinar will provide you a unique opportunity to ask your questions to Dr. Marc Gerdisch, the Chief of Cardiac Surgery at Franciscan Health, who is a world-renowned, minimally-invasive expert having performed over 5,000 heart valve operations.
Also… If you have any questions you would like to send me in advance of the webinar, I will get them answered during the webinar. Please email your questions to adam@heartvalvesurgery.com.
I look forward to seeing you on this interactive webinar!
Keep on tickin,
Adam
New Dynamic “Patient News Feed” Launches!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: May 22, 2025
Hey Everybody,
Here’s a quick update regarding the launch of several new dynamic features at the Patient News Feed which is one of the most trafficked pages on our website.
If you would like to see the new updates at the Patient News Feed, click here.
John Warns You About Tissue Valve Complications
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: May 23, 2025
I received a very interesting note from John Bryan, a heart valve patient. I share John’s story not to scare you but rather to educate you specific to the realities of valvular defects, heart valve replacement durability, and cardiac monitoring.

After Ross Procedure, David Teaches Dr. El-Hamamsy the Harmonica
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: May 14, 2025
What happened after David Herzhaft, an aortic valve patient from Idaho, had a successful Ross Procedure performed by Dr. Ismail El-Hamamsy at Mount Sinai in New York City?
To answer that question, here is a really fun patient success story as told by David.

TAVR Powers Richard To Mount Whitney Peak
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: May 8, 2025
I LOVE getting inspirational updates from heart patients all over the world.
This time, Richard Godbey shared a big milestone for him after transcatheter aortic valve replacement (TAVR).

Patient Innovation: Will You Test Our New AI-Powered Heart Valve Chatbot?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: May 6, 2025
Great news! To educate patients, their families and friends, we just released the world’s first Heart Valve Chatbot powered by artificial intelligence. The Heart Valve Chatbot was created with the support of 100+ heart valve doctors and 1000s of patients.
Below is a quick video that describes the futuristic features of the Heart Valve Chatbot. After you watch the video, I would really appreciate it if you would use the Heart Valve Chatbot and provide your feedback.
>>> To test the Heart Valve Chatbot, simply click the “Blue Chat Icon” at the bottom-right section of this page. When you’re done using the Heart Valve Chatbot, please click the three vertical dots at the top of chatbot and select “End Chat” to complete the survey.
Ed Salutes Dr. Gillinov After Crossing Antarctic Circle
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: April 30, 2025
Hearing from patients about their heart valve surgery journey is my favorite part of running this website.
This time, we get to learn the amazing success story of Edward Rutkowski, a patient who underwent robotic heart valve surgery 15 years ago.

Tammi’s 10-Year Heart Valve Anniversary!
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: April 24, 2025
How good can life be 10 years after successful heart valve surgery by Dr. Robert Saeid Farivar?
Thanks to Tammi Gunwall, a patient who recently celebrated her 10th heart valve anniversary, we know that life can be pretty darn great.

How Does Blood Flow Through Your Heart Valves & Your Body?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: April 15, 2025
The patients and family members in our community never cease to amaze me.
This time, John Berner, did something quite amazing. To help educate himself, his wife (a heart valve patient), and our community, John took it upon himself to create a diagram that answers the very important question, “How does blood flow through your heart valves and your body?”
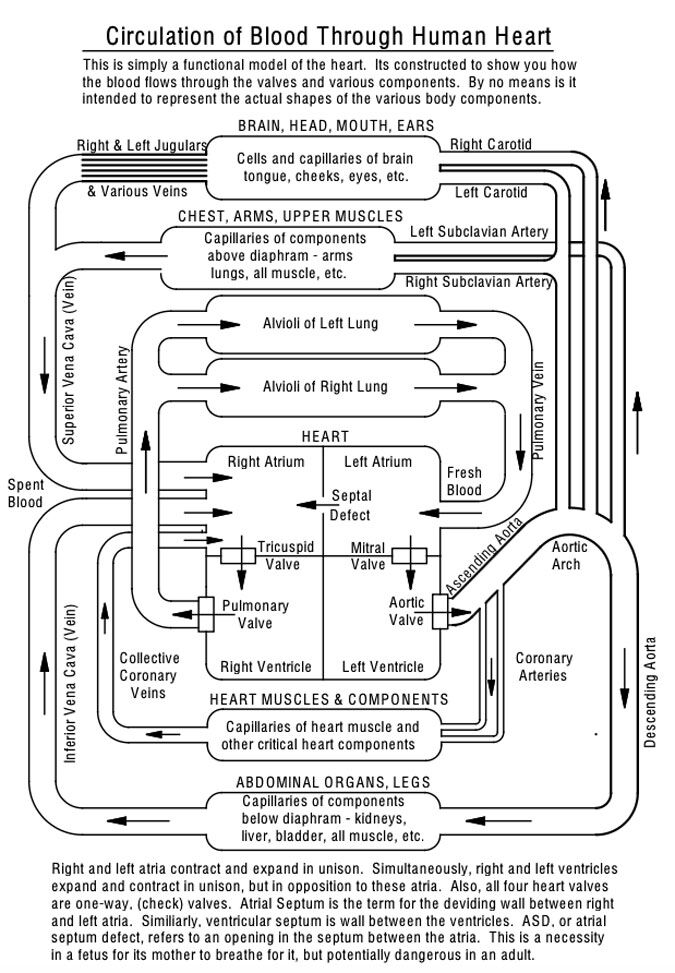
13 Questions To Ask Your Surgeon Before Heart Valve Surgery
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: April 6, 2025
During our recent webinar, “6 Expert Tips for Heart Valve Patients”, our expert panelists including Dr. Doug Johnston, Dr. Melissa Medina and Dr. Kevin Hodges of Northwestern Medicine got into a meaningful conversation about the 13 questions patients should ask their surgeons and heart teams before scheduling a procedure. (Click here to watch a video replay of this special webinar.)
Dottie’s Travel Alert for TAVR Patients
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: April 2, 2025
Are you planning to travel this spring or summer? If you are a transcatheter aortic valve replacement (TAVR) recipient, don’t be alarmed if you unexpectedly set off the airport security system.
Linda Travels to Germany for New JenaValve TAVR
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Published: March 27, 2025
Truly amazing. I just heard another extraordinary patient success story from our community.
As many of you know, transcatheter aortic valve replacement (TAVR) is often referred to as one of the greatest “medical breakthroughs” in valvular therapy. Using this minimally-invasive approach, cardiac surgeons and interventional cardiologists can replace a stenotic aortic valve without breaking the patient’s sternum or ribs. However, the use of TAVR has been limited to the treatment of aortic stenosis, a narrow valve. The utility of TAVR for aortic regurgitation (a leaky valve) has not received FDA-approval for the treatment of aortic regurgitation here in the United States.
Given the limited access to TAVR devices for aortic regurgitation, Linda Nolan, a patient with severe aortic regurgitation, had options. Linda could get open heart surgery here in the US. Or, Linda could transform into medical tourist and go abroad for a new type of TAVR called the JenaValve.







