“When I Wake Up In The ICU, How Many Tubes Will Be Sticking Out Of Me?” Asks Gwen
By Adam Pick on September 1, 2009
I just received a fantastic question from Gwen about waking up in the intensive care unit after heart valve surgery.
She writes, “Adam – Thanks so much for all your help. While I’m still anxious, your support has made me feel somewhat ready for my upcoming heart valve operation. I have one more question for you about the intensive care unit. When I wake up from surgery, exactly how many tubes are going to be sticking in/out of me? Keep on tickin! Gwen”
Interestingly enough, this question triggered a very, very, very unique memory for me.
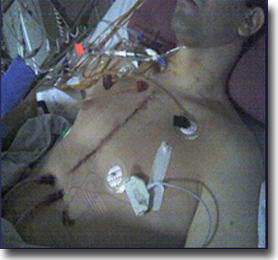
Me (Adam) In The Intensive Care Unit
So you know… My doctors and nurses did not explicitly detail the patient experience within the intensive care unit. Looking back on it, that would have really helped manage my expectation as I came out of general anesthesia.
The first thing I noticed when I woke up from my heart valve surgery was, in fact, a tube… the ventilator tube. (Yes, I was one of the lucky patients that woke up with the vent tube still in place.)
Then, as I continued to regain consciousness, I continued to see more-and-more tubes. As the picture above shows, even after the vent tube was removed, there were two chest tubes, my I.V. drip and another tube sticking out of my neck.
In total, I remember five tubes.
Whoops. Wait. I’m wrong. There was one more tube.
How on Earth could I forget the urinary catheter? 🙂
Ok. The count just increased to six tubes. There you have it. In my experience, there were six tubes sticking in/out of my body after heart surgery.
But, please remember, in addition to the tubes… There will also be several important wires scattered on-and-around your body as you wake up. To illustrate this point, here is a great picture I just received from Charles. FYI, Charles appropriately titled this picture, You Figure It Out!
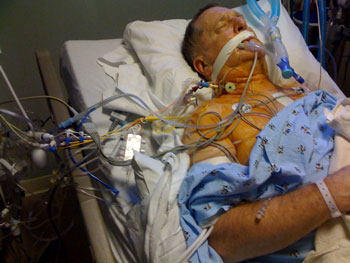
Charles In The Intensive Care Unit
I hope this helps Gwen (and perhaps you) learn a little more about the reality of waking up in the intensive care unit after heart surgery.
Keep on tickin!
Adam
|
Midge says on September 1st, 2009 at 11:34 pm |
|
I had my husband take a photo of me a few hours after surgery while in the CICU and agree with Adam that 6 looks to be about right…..but this does not include all the electrical connections for the heart monitor, BP, pulse, etc. It is just tubes. By the time I would have cared about how many tubes I had, they were gone except for maybe the Foley catheter. I think once the ventilator tube is gone, the rest are not very annoying and not painful to remove. Midge |
 |
|
Dawn says on September 2nd, 2009 at 1:23 pm |
|
Maybe you will be lucky like me and not remember intensive care or the vent tube at all. I woke up in my room and did still have a couple of wires and tubes, but not much. |
 |
|
Heather says on September 2nd, 2009 at 1:41 pm |
|
What does it feel like to have the ventilator tube taken out? |
 |
|
Rita says on September 2nd, 2009 at 1:43 pm |
|
Hi Gwen I know my surgeon was very nice – he knew that I was not to be awake till the throat tube is out and he agreed. Other than that due to issues of stabilization I had a total of 13 iv lines and tubes and wires. My daughter was shocked but I truly can say other than the urinary catheter I honestly felt one of them. |
 |
|
Carol Lang says on September 2nd, 2009 at 2:02 pm |
|
Being a former ICU nurse I can tell you that Charles has a few other tube “issues” going on from his picture. Anyway, that about sums it up. But, they each have a purpose & a meaning and do come out in rapid succession. Don’t want to risk any infections by having them in longer then needed. |
 |
|
Adam Pick says on September 2nd, 2009 at 2:08 pm |
|
Carol, Thank you! Thank you! Thank you! Your comments will be incredibly helpful to us all!!!! Keep on tickin! Adam |
 |
|
Rosie says on September 2nd, 2009 at 2:34 pm |
|
Gwen!! |
 |
|
Cindy McGinn says on September 2nd, 2009 at 2:55 pm |
|
Hi All, Heather, I was awake when my ventilator tube came out. I could feel them pulling on it but it was more a sense of relief that it was gone and that part was over with then painful. I remember the nurses telling me that I did good and that wasn’t so bad. I told them I had watched to many episodes of the TV show ER and they all laughed. Gwen, Hang in there and try to relax. I know the anticipation is hard, but soon the hospital stay will be a blur. I’m 7 months post valve replacement and doing great. Like Rosie said, stay positive and it will be fine. Wishing the best for you. |
 |
|
Robin Hirsch says on September 2nd, 2009 at 3:27 pm |
|
You wake up in ICU really happy to be alive. Then you begin to take account of yourself. They have a breathing tube stuffed down your throat, every part of your body hurts like hell, the first time you sit up your head spins so bad you have to lie down, and everybody there is telling you that you’re doing great. It is amazing how quickly you go from that to feeling better. Less than 24 after surgery I was up and walking around, I was tansferred out of ICU on to a cardiac floor, and was eating solid food. Push yourself hard and you will get results. Four days after surgery I was home. |
 |
|
Rose M. says on September 2nd, 2009 at 3:42 pm |
|
Helen asked on 9/13/09 regarding the vent. tube. I had a Ross Procedure on July 01, 2009 and I remember the ICU staff telling me that the vent tube will be removed. They informed me that they would be removing the tubing and all I had to do was cough really hard. I remember the whole ordeal vividly. I remember the staff saying, “ok, were going to start and COUGH!” as they pulled the tubing out, I began coughing as much as I could and as hard as I could because I wanted the tubing out so I could talk. Pain? I dont remember it being painful as they pulled, but I could feel somthing being pulled out and seeing them pulling the tubing out even though I was partially awake. Thank goodness, it was easier to breath on my own than with the tubing down your throat. |
 |
|
Matt says on September 2nd, 2009 at 3:55 pm |
|
I’m in the hospital as I write this. I just had my bicuspid aortic valve replaced with a St. Jude mech. I’m 32 & very healthy, I ran a 10k on Monday and had the surgery yesterday. The doctor said everything went perfect & I practicly lepped of the operating table when it was over. I had a minimally invasive proceedure & only ended up with a 2 inch incision. This morning I got rid of 2 tubes, one being the urinary cath, that little sucker stung coming out, but once again was over in a matter of seconds. Tomorrow they will take out the 2 chest tubes and the pulmonary neck cath. This will leave me with only the arm I. V. |
 |
|
Rose M. says on September 2nd, 2009 at 3:57 pm |
|
Gwen, the anticipation of surgery is high, however I agree with Cindy and Rosie’s response. YOU NEED TO STAY POSITIVE!! Be well informed of what is expected post surgery and YOU WILL BE OKAY. I had a lot of anxiety prior to surgery also. Just remember why you need the surgery and benefits or positive aspects of the outcomes…Wishing you the best! |
 |
|
Rebecca Roberts says on September 2nd, 2009 at 7:25 pm |
|
Gwen: I had a mitral valve repair 8 months ago. I, too, have pictures of myself in the ICU, and they are frightening to look at! The good thing is that I did not have to look at myself in the ICU! I certainly did not feel nearly as bad as I looked! |
 |
|
Ann Crouch says on September 2nd, 2009 at 9:39 pm |
|
Gwen, I could not tell you how many tubes if my life depended on it. I have such a limited memory of when I was in intensive care that I could tell you anything about it for sure. I don’t even remember seeing my family. Actually I don’t remember too much at all about the days after my surgery. I guess everyone is different and reacts to meds differently. |
 |
|
Gail Kapcsandi says on September 2nd, 2009 at 10:37 pm |
|
Gwen/ Heather – I have very little recollection about ICU except for having the remote control in my hand trying to catch The Bachelorette and |
 |
|
Midge says on September 2nd, 2009 at 11:04 pm |
|
Glad to see so many of you without any memory of the ICU. I tell everybody that God reached down and gently kissed my eyes closed as I was going into surgery and let me sleep without a memory or care for 3 days. I don’t even remember making it to surgery….I went nighty night on the way out of the surgery prep area and woke up three days later in my regular cardiac care room. Had no after effects of sleeping for so long, as I was up walking around and getting to the bathroom by myself by the end of that day. Feel like my body had a good, long rest to get the healing process going strong. Midge |
 |
|
Rick Parks says on September 3rd, 2009 at 1:05 am |
|
Gwen, I had a section of aorta and my aortic valve replaced on August 3, 2009. Generally, I found the whole experience much easier and less painful than I have been anticipating over the last 25 years of knowing that someday I was going to have surgery if something else didn’t get me first. I was surprised at the time between being told by my cardiologist on June 11 and flying out to Cleveland for surgery on August 3 that anxiety never welled up much at all. Maybe knowing that this was most likely coming made the actual event more of a celebration of moving on and getting my health back. That said, and specifically to you’re question about tubes, I agree and can relate to most everything that has been posted before me–its a half dozen or more and for me having the tubes and then their removal was mostly painless with the exception of the urinary catheter which stung for a few seconds during removal. Removal of the pacing wires from my heart was startling but painless. Unlike some who slept through ICU I was awake early on and with the breathing tube for an hour or so before they pulled it. They did ask my to give a big cough as they pulled it and while removal of the tube itself was painless the cough made me acutely aware that my split sternum was on the mend. Going beyond your question about tubes, I attribute my success and lack of anxiety to getting prepared by reading Adam Pick’s blog and book Heart Valve Surgery, learning all I could about bicuspid aortic valve disease, being in could shape prior to surgery, having long term health goals, practicing visualization techniques to prepare for before and after surgery (don’t know about other hospitals but Mayo Clinic and Cleveland Clinic emphasize and provide visualization technique training in hospital and on CDs prior to admittence), and finally my decision to have Dr. Gosta Pettersson at Cleveland Clinic lead the team to make me better. Its been a positive experiance exceeding my expectatins. I am very thankful for eveyones contributions to my success and I hope your eperience is as good or better. Rick |
 |
|
Debbie Shipley says on September 3rd, 2009 at 5:49 am |
|
I just wanted to write and tell you that I bought your book. The help and support it gave my partner and my family was great! |
 |
|
Sandy Marks says on September 3rd, 2009 at 8:00 am |
|
My husband is scheduled for this surgery soon, and my ability to be off with him is limited. I would like to know when he will most need me, of course I plan to be at the hospital the day of surgery, but beyond that will he need me in the initial days ensuing surgery or after he’s released and returns home. |
 |
|
Marion says on September 3rd, 2009 at 1:55 pm |
|
Hi Gwen I had my surgery at the Royal Jubillee Hospital in Victoria Bc and they have an excellent pre-surgery information orientation session which all patients have to attend the day before. During that session they take the patient and their immediate carer into the ICU so they can see first hand patients wired up and recovering. At that time we could ask questions. I was not shocked by any of this because I had read Adams book but my husband and daughter reeled a bit with shock but later said it was invaluable. In my case I was not conscious when the breathing tube was removed and as for all the wires and monitors they were actually placed behind me and therefore I could not see them. Gradually by the time I left intensive care some 18 hours later some of wires and tubes were removed so that when I reached my room on the ward I was not worried about any of them. (Remember your time in the ICU is a haze because you are drifting in and out of consciousness at that time). I am still in awe of how easy a time I had. After the first few days I only took Tylenol ES and was off them completely at 2 weeks post surgery. The only problems I encountered were rolling in and out of bed and getting up from a chair or toilet without using my arms to steady me. I also had to wear a bra day and night for six weeks because I am well endoured in that area and when lying flat on my back my breasts would have pulled against the cut in my sternum. As such the bra rubbed and pulled on my scar. And that is all I have had to deal with except the extreme tiredness of course. Stay positive. Ask endless questions. Don’t worry and good luck to you with your op. Marion |
 |
|
Dan Burk says on September 3rd, 2009 at 2:02 pm |
|
Thanks everyone for your comments, stories, suggestions, etc. I think all this information is great stuff! |
 |
|
Barbara J. says on September 7th, 2009 at 7:13 am |
|
For Rick Parks or anyone who has traveled a long way for their sugery– |
 |
|
jennifer mc cabe says on June 18th, 2010 at 10:36 am |
|
hi adam my name is jennifer mc cabe i am 19 years of age and on wensday coming i am due to have the ross procedure done i have had the ballon done 3 times in my life and they all went fine. but this one is different im not sure what way i will react afterwards, i have a little boy he is 15 months now and i dont want to be away from him for to long or not be able to hold him. i was told it will take 2 months to recovery but does it really. |
 |
|
Julie says on June 22nd, 2010 at 9:09 pm |
|
Hi i had aortic valve replacement on 29th april 2010 due to severe aortic stenosis from bicuspid valve.although they give you books to read on before cardic surgery and also after cardiac surgery i was still terrified, i have big breasts and had a bit of trouble could not wear a bra for support because my wound between my boobs at the bottom and also the drain hole and the 2 wires into the heart so had to go without so they could heal.so my chest is still a little sore along with everthing else sholders neck back etc, i remember the ventilator tube as i gagged on it a couple of times they said would take it out when my oxygen readings were normal my family just looked at me in icu and started to cry because of all the attached tubes etc thank god i did’t see.still can’t sleep properly as well as having hot flushes from change of life still have neck and back pain, have had some physio lately is helping hopefully i will be ok before i go back to work. |
 |
|
Dan says on June 24th, 2010 at 9:19 am |
|
WOW! My best friend bought your book for me last week. I have read it cover to cover. My surgery is set for 7:30 am tomorrow. (bicuspid valve relacement and an aortic root aneurysm). THANK YOU ! |
 |
|
Louise says on June 24th, 2010 at 1:26 pm |
|
The comment above was left by my baby brother….DAN….. Adam your book has been invaluable in his pre-op phase,sharing your story has been helpfu ,I’m sure, to so many…. And I want to thank you for your efforts, A GOD send to many….”everything’s gonna be alright”… don;t worry JuDY….;) |
 |
|
Gary Loveland says on July 1st, 2010 at 10:50 pm |
|
To whom all are that are having heart surgery. Fist I’ve never had heart surgery but my dear wife has had four. The first in 1975 which back then was a rare thing. You didn’t even talk about it because you new the outcome could be bad. Back when my wife had her first we where ignorant to what was going on but it wasn’t pleasent and it was more of a reseach thing then now. They didn;t talk about it back then ,it was just done. Now everyone talks about heart surgery. Which can be better depending on how you look at things. Heart surgery patients meaning bypass patients tend to do farely well and tend to get out of the hopsital quicker then valve surgery patients. They tend to stay a couple of days longer. As far as pain every person is different and also how well you doctors are on top of this. Feel freely to tell them your concerns and fears because it helps them to treat you. My wife feared the vent tubes and struggeled with them therefore had to be tired down some. Which frustrated her, but I new they where protecting her and even tried keeping her heavily sedated. It was a long and hard battle the forth time. People what they never tell you and this is the honest gods truth once a heart surgery your more then likely to have another. Each time seems to be a little harder then the last. This is where I say have a good heart surgeon. My wifes was Todd Dewey at Medical City Dallas and he was incredible. She had complicatoins, seizures etc, etc, life support – ICU AND NICU and even in critical care, etc. Bottom line is everyone needs to be open and honest and have a understanding of your desires. My wife and I clearly did with the surgeons and above all they where very supportive of her wishes. She was always a strong person at heart but when your having heart surgery and all the drugs sometimes your fears over come you while you are medicated. I stayed with her a lot this forth time and understood her better then anyone else and thats the main reason she made it. She couldn’t talk because of all the tubes, the vent machine etc, etc. but what she could do was see I was there and always being caring and supportive which helped a lot. If the patient sees you get scare they get scared. Believe me at times I could have been if only you new what we dealth with but my final say is “god was the get through person”. She was on life support much longer the we’d like, etc, but god has his hand in all things – we took it for the better. I saw stressed doctors, stressed nurses but always remember to ask god to keep his hand on all of them, including yourselves. My advise is to have good listeners and caring people around. We didn’t have that, there was no one. But we are blessed because we know ours hearts and forgive others. Because we want others to forgive us. I’ll say keep focused on your god and loved ones – we all need them and god be with you all. Rememebr each person is different and outcomes and reactions will be different for everyone. Be pateint and be strong and take in as much love as you can get……….. |
 |
|
Meigs says on July 3rd, 2010 at 12:16 am |
|
I had mitral valve surgery last Dec. When I woke up, The only “tube” I was aware of was the vent tube- but I found that easy to deal with. I knew that they would want me to be calm. I enjoyed being very still and listening in on the nurses conversations. They told me they were waiting for some value- I think it was blood pressure before removing it- I did feel assured that they would remove it as soon as they could. I asked and asnwered by writing on the chalk board they held for me. As I had meds in me from the surgery still- it was not like I was entirely awake as I am now- analyzing – it was very easy to go with the flow. I did not feel or care to count any other tubes then. By the next day when I was more aware and the tube gone (which was no problem going) – I could notice the ivs and the wires and catheter- but I was most interested in being happy it was over and went well, seeing my family was there and sleeping… Meigs |
 |
|
wendy suchinski says on August 12th, 2011 at 12:26 pm |
|
The tubes are short lived. I am 3 weeks post op aortic valve replacement and am still finding remnants of all the sticky stuff that holds all those tubes,lines,and telemetry in place. I think it will be awhile before it’s all gone. |
 |