"Is Stroke A Risk During Valve Surgery?" Asks Debbie
Page Last Updated: May 12, 2025
I just received a very, very, very interesting question from Debbie about stroke and heart surgery.
Debbie writes, "Adam - My mom is having open heart surgery next week due to severe regurgitation from a mitral valve prolapse. I have heard that stroke is a risk for patients during cardiac surgery. Is that true?"
So you know... Debbie's question brings back a distinct and touching memory for me as I prepared for my own heart valve surgery.
It was December 20, 2005, the day before my aortic and pulmonary valve replacement surgery. I was at USC Medical Center in Los Angeles, California. My pre-operative tests were almost complete when it came time to discuss the surgical consent form.
Dr. Lee, the surgical resident, sat me down to explain all the risk factors associated with heart surgery. My palms began to sweat and my heart began to race as Dr. Lee reviewed each risk one-by-one.
My mother, Donna, was with me at the hospital that day. I don't know how, but she could sense the fear-and-anxiety growing in me as Dr. Lee continued down the list. To comfort me, she put her arms around my shoulders and hugged me lovingly. Needless to say, it was an epic moment for a mother-and-son to share.
Then... Being the optimist that I am... I pushed the fear-and-anxiety aside. I remembered all the research and due diligence which supported a confident selection of my surgical procedure and my surgeon, Doctor Vaughn Starnes. My life, my future, my heart would be in his hands. I signed the consent form knowing that I had found one of the most qualified surgeons for the job. Doctor Starnes would fix me.
Now, back to Debbie's question... (Sorry for the trip down memory lane.)
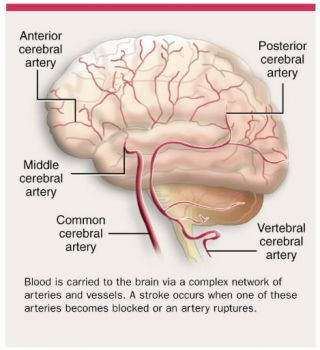
Yes, stroke is one of the risks that Dr. Lee discussed with me. According to the Mayo Clinic, "There are two main causes of stroke. An ischemic stroke is caused by a blocked artery in the brain. A hemorrhagic stroke is caused by leaking or bursting of a blood vessel in the brain. Some people may have only a temporary disruption of blood flow to the brain, known as a transient ischemic attack (TIA). A TIA doesn't cause lasting symptoms."
Reports suggest, "A major concern with cardiac surgery is the incidence of neurological damage. Stroke occurs in 2-3% of all people undergoing cardiac surgery and is higher in patients at risk for stroke." So you know, stroke can occur during or after heart surgery.
When I think about that statistical risk, I don't perceive it as overwhelmingly significant. Yes, stroke does occur for some cardiac surgery patients. But, as we have previously discussed, there is risk in almost everything we do, every day of our lives - driving our cars, walking across the street, even eating peanut butter these days. Come to think of it... Life is, to some extent, a risky situation.
However, risk can be mitigated. That is why I am such an advocate of extensive surgeon research prior to heart surgery. Patients need to be 100% confident in their surgeons and their medical team. I'll never forget what Dr. Lee, the surgical resident, said to me about stroke. He said, "Stroke is a possibility, but luckily, you found Dr. Starnes. He is one of the best out there. If anyone can prevent a stroke from happening, it's Dr. Starnes."
Related Links :
I hope that helps explain a little more about the risks of stroke and cardiac surgery.
Keep on tickin!
Adam
Written by Adam Pick
Patient & Website Founder

Written by Adam Pick - Patient & Website Founder
Adam Pick is a heart valve patient and author of The Patient's Guide To Heart Valve Surgery. In 2006, Adam founded HeartValveSurgery.com to educate and empower patients. This award-winning website has helped over 10 million people fight heart valve disease. Adam has been featured by the American Heart Association and Medical News Today.
Comments
Adam's Newest Blogs
New Community Posts
Blog Categories
- Adam's Updates
- Aneurysms
- Aortic Stenosis
- Aortic Valve Repair
- Aortic Valve Replacement
- Atrial Fibrillation
- Before Surgery
- Bicuspid Aortic Valve
- Heart Valve Replacement
- Medical Technology
- Mitral Regurgitation
- Mitral Valve Repair
- Patient Stories
- Pulmonary Valve
- Recovery
- Ross Procedure
- Surgeons & Hospitals
- Tricuspid Valve
Adam's Newest Blogs
Blog Categories
- Adam's Updates
- Aneurysms
- Aortic Stenosis
- Aortic Valve Repair
- Aortic Valve Replacement
- Atrial Fibrillation
- Before Surgery
- Bicuspid Aortic Valve
- Heart Valve Replacement
- Medical Technology
- Mitral Regurgitation
- Mitral Valve Repair
- Patient Stories
- Pulmonary Valve
- Recovery
- Ross Procedure
- Surgeons & Hospitals
- Tricuspid Valve
Blog Categories
- Adam's Updates
- Aneurysms
- Aortic Stenosis
- Aortic Valve Repair
- Aortic Valve Replacement
- Atrial Fibrillation
- Before Surgery
- Bicuspid Aortic Valve
- Heart Valve Replacement
- Medical Technology
- Mitral Regurgitation
- Mitral Valve Repair
- Patient Stories
- Pulmonary Valve
- Recovery
- Ross Procedure
- Surgeons & Hospitals
- Tricuspid Valve
Surgeon Spotlight
Dr. Christopher Heid is a leading cardiac surgeon at UT Southwestern in Dallas, Texas who specializes in heart valve repair and replacement operations.
Adam's Video Library
Learn about heart valve surgery and patient success stories at Adam's video library.
New Posts From Our Community

Ercan Afacan from
Montreal, Canada
6 Months Post-op!! Completed Rehab. For those going through recovery, hang...
Meet Ercan
Heather Leigh from
Brooklyn, New York
Hi all!! Surgery went well- robotics worked so it was just...
Meet Heather
Find Heart Valve Surgeons
Search 1,500 patient-recommended surgeons
Surgeon Spotlight
Dr. Christopher Heid is a leading cardiac surgeon at UT Southwestern in Dallas, Texas who specializes in heart valve repair and replacement operations.
Adam's Video Library
Learn about heart valve surgery and patient success stories at Adam's video library.