Technology Update: FDA Approves Perceval Sutureless Heart Valve; 7 Facts You Need To Know
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Experts: Eric Roselli, MD; Gorav Ailawadi, MD; Niv Ad, MD
Page Last Updated: July 16, 2025
The Perceval Sutureless Heart Valve just received a Food & Drug Administration (FDA) approval on January 11, 2016. This was really big news as the Perceval is the first rapid-deployment, sutureless heart valve for patients with aortic stenosis.
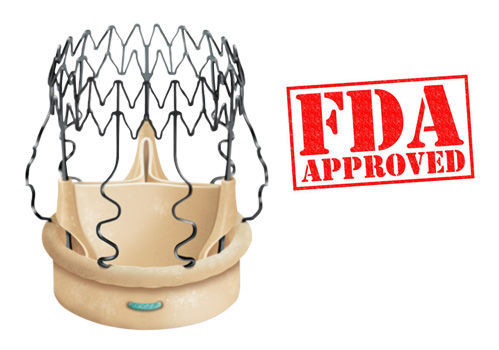
To educate our patient community about the significant implications of the Perceval’s FDA approval, I contacted three leading cardiac surgeons who were part of the clinical trials which led to Perceval’s FDA approval – Dr. Niv Ad, Dr. Gorav Ailawadi and Dr. Eric Roselli.

1. Why is the FDA approval of the Perceval Sutureless Valve important for the evolution of valve therapy?
Dr. Eric Roselli, who is the Director of the Aortic Center at the Cleveland Clinic, wrote to me, “Most simply, it provides us another option in the surgical treatment of aortic valve disease. As a sutureless device it can be delivered and fixed into the heart faster than a conventional sutured repair. Because it is collapsible, it may facilitate the use of less invasive approaches like mini right thoracotomy which is currently only offered at a few centers. It is somewhat of a hybrid approach with benefits of simplicity like TAVR while maintaining the benefits of surgical AVR like excision of the native aortic valve and a very low rate of perivalvular leak.
Dr. Niv Ad shared in an interview with me, “This is a new generation of aortic valves that have clear advantages over the traditional stented valves that requires sutures. The valve can be used with patients who are at high risk, especially the younger ones, in which we’re not so certain regarding the durability of TAVR.”
2. What do you see as the number one patient benefit of the Perceval valve?
Dr. Gorav Ailawadi noted, “For the patient, there is shorter time on the heart-lung machine, particularly with the heart stopped, which is the greatest benefit. Fortunately, nowadays, there is little damage to being on the heart-lung machine. Nevertheless, we as surgeons like to minimize this time for our patients.”
Dr. Niv Ad shared with me, “I think that what impressed me the most is the hemodynamic performance of the Perceval sutureless valve — meaning the valve has a very low gradient comparable to a TAVR, which is going to allow very good recovery of the left ventricle and reverse remodeling to be normal, or near normal, and obviously the function of the patients and the ability to exercise is going to be impacted somewhat because of this excellent very low gradient.”
Dr. Roselli says, “For now, the results of the US trial and previously published experiences have demonstrated the safety and early efficacy of the device. Based on the standardized bench top testing it has demonstrated mechanical durability, time will tell us how durable it is in people. Having said that, in the short term it seems to be comparable to the standard surgical valves and may offer the benefit of allowing lesser invasive approaches and may also offer the advantage of safety for patients who are at risk during longer or more complex operations. One example of these latter patients are those who have had a previous valve replacement that has degenerated, especially those who had a previous homograft or stentless root replacement.”
3. Is the valve really “sutureless”? How does it anchor into place? Can it move after implant?
Dr. Ailawadi wrote to me, “It is completely sutureless in how it stays in place. In none of the patients in various clinical trials, did the valve embolize, or pop out.”
Dr. Roselli said, “Yes, it is truly sutureless. During the procedure we use three sutures to guide the device into position, and then they are removed after deployment. It is anchored by the radial, or outward, force from the stent to which the new valve cusps are sewn to. Because of its elegant shape, when it is placed in the properly selected patient it will not move or migrate. One group of patients who are important to be aware of are those with aortopathy or the risk of developing an aortic aneurysm. Theoretically, if the aortic root grows too big because of this aneurysmal process, then the device could migrate, but the device typically is not selected for these patients and even most patients with aneurysm develop them in the more downstream ascending aorta and not the root.”
4. Are all patients candidates for Perceval? Or, is the valve reserved for certain patient segments (high risk, inoperable)?
Dr. Roselli says, “It really could be used in any patient with aortic valve disease except those with the propensity for developing aortic root aneurysms as described above.”
Specific to patients needing multiple cardiac procedures at the time of surgery, Dr. Ad shared, “I think this is an excellent point. If we have a patient that will require, let’s say, coronary bypass surgery, then the sutureless valve will allow us to move in those complex patients much quicker with the aortic valve being done very, very quickly together.”
5. What is your clinical experience with Perceval? How are your patients doing?
Dr. Ad says, “We were a very active site, and we did close to 40 patients during the study and the continuous enrollment period. During the study period, we didn’t have any unique problems associated with the valve.”
Dr. Roselli says, “We were one of the 18 centers that participated in the US trial, and one of the leading enrollers in the study. We have used the device in patients of all ages, with tricuspid and bicuspid valves, and all of the isolated valve replacement cases (without the need for coronary bypass grafting or other concomitant procedures) the procedures were done with a minimally invasive approach including mini sternotomy and right anterior thoracotomy. Dr. Doug Johnston was the other participating surgeon in our group.”
Dr. Ailawadi says, “As one of the top enrollers, we implanted the Perceval valve in over 30 patients in the initial trial in the USA (Perceval trial). Our patients are still being followed yearly per the study protocol and they feel well with the vast majority having returned to activity levels better than prior to surgery.”
6. What is the number one advantage that Perceval offers cardiac surgeons like yourself?
Dr. Ailawadi says, “For surgeons, the Perceval valve makes minimally invasive aortic valve replacement much easier for the surgeon by avoiding having to put sutures in and tie them down. This is ultimately a benefit to the patient if a surgeon is already comfortable with minimally invasive surgery, this valve makes it simpler and potentially safer for the patient.”
Dr. Roselli says, “As the treatment options expand and evolve, so does our understanding of the aortic valve diseases we treat. It is becoming increasingly important for us to tailor the treatment we deliver to the individual patient and their particular disease. This is no longer a treatment fits all world. A collapsible sutureless valve offers another treatment option that we can tailor to our patients’ needs.”
Dr. Ad noted, “It’s a very short learning curve for surgeons. Unlike other valves, this valve is very intuitive to implant. You have all the control of the implantation process despite the fact this is a sutureless valve. The placement of the device is easy and quick, and we were very pleased.”
7. Is sutureless technology going to expand from the aortic valve to other valves? What do you see as the future of this technology?
Dr. Roselli says, “Currently there are no active trials to apply this therapy in other valves, but I believe this could be particularly helpful in patients with multi-valve disease especially those with severe mitral calcification or degenerated valves.”
Dr. Ailawadi wrote, “Sutureless valve technology is being developed in other valves; in particular, the mitral valve. In terms of the future, with TAVR and transcatheter mitral valve replacement changing the scope of our practice, it is possible these sutureless technologies may become mainstream for low risk patients undergoing surgery, for those patients who need multiple valves corrected with or without bypass surgery, or those with extremely complex disease that cannot be treated via transcatheter approach. The hope is that this first approved valve is on the forefront of other valves and technologies for years to come.”
Well… I hope that helped you learn more about the Perceval Sutureless Valve and its innovative use for patients with aortic stenosis. I would like to extend a huge thank you to Drs. Ad, Ailawadi and Roselli for taking the time to share their clinical experiences and research with our patient community.
Related Links:
- Medtronic Low-Risk TAVR Patient Education Center
- Breakthrough Innovation: Inspiris Resilia Tissue Valve
- Linda Travels to Germany for New JenaValve TAVR
Keep on tickin!
Adam
|
paddler1 says on January 27th, 2016 at 2:51 pm |
|
Does this valve require the patient to be on anticoagulants post-op? Will this valve be a possible replacement for a worn or otherwise defective tissue valve, such as the Edwards bovine valve, which has previously been implanted? |
 |
|
Adam says on January 27th, 2016 at 3:25 pm |
|
Hey there, Great questions! The Perceval sutureless heart valve does not require the patients to be on blood thinners. And… Yes, the Perceval can be used for surgical re-operations. I hope that helps! |
 |