Surgeon Q&A: Dr. T. Sloane Guy Helps Kerrigan, Simone & Tina
By Adam Pick on December 19, 2012
Lately, my inbox has been filled with great questions from patients all over the world. For example, Kerrigan, Simone and Tina just asked me about tissue valve replacement selection, Coumadin and atrial fibrillation.
To answers these questions, I was very fortunate to connect with Dr. T. Sloane Guy, who is the Chief of Cardiothoracic Surgery at Temple University Hospital in Philadelphia, Pennsylvania. During his career, Dr. Guy has performed over 2,000 cardiac procedures of which 50% included either heart valve replacement operations or heart valve repair therapy. As you can read below, Dr. Guy took the time to respond to each question from Kerrigan, Simone and Tina.

Dr. T. Sloane Guy – Heart Valve Surgeon
Question #1 – Kerrigan asks, “Have porcine aortic replacement valves fallen out of favor with bovine valves taking the lead? It seems like we are hearing about bovine these days and not porcine as the valve of choice for aortic valve replacements. What, if any, are the advantages of bovine valves over porcine valves?”
Response from Dr. T. Sloane Guy: Modern bioprosthetic valves are made of a variety of different tissues including cow (bovine) pericardium, actual pig (porcine) valves, and horse pericardium as well. All tissue valves are subject to degeneration over time and degenerate more quickly in younger patients which is why the American Heart Association guidelines recommend tissue valves for patients 65 years and older. Whether one type of tissue or another is “better” is very debatable and, in my opinion, unclear. Of course, the various companies that sell the valves promote the notion that their valve is superior. The truth is that they all have slightly different features but in order to get approved by the FDA had to go through incredibly rigorous testing and may in fact not be as different as suggested.
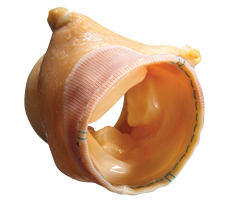
Response from Dr. T. Sloane Guy: In my practice, I tend toward porcine valves because I feel they are less susceptible to distortion, have solid long term outcome data, and their mode of failure is insufficiency (leaking) rather than stenosis (narrowed) which is a more dangerous condition. That being said, pericardial valves also have great data to support their use and I know good surgeons I would trust my family with who use both types of valves.
Question #2 – Simone asks, “What is the latest update regarding mechanical valves and Coumadin? Will it always be necessary to take blood thinners if I choose a mechanical valve?”
Response from Dr. T. Sloane Guy: At this point, the answer would be yes. There has been some work done in taking low risk patients and putting them on anti-platelet agents alone. Other studies have explored lower INR’s (measure of blood “thinness” with some promising results. So the answer may change in the near future but I would caution that if you have a mechanical valve you should plan on needing coumadin.
Valve thrombosis (clotting) or stroke are very serious. Probably more important to patients will be to get home INR testing capability and follow the literature to determine the target INR goals.
Question #3 – Tina asks, “I’ve been told I need a mitral valve repair. I also have afib. I’ve read that a procedure can be done simultaneously to fix these disorders. But, can it be done with the robot at one time?”
Response from Dr. T. Sloane Guy: Absolutely. In my practice, we perform totally endoscopic mitral valve procedures routinely and often add a procedure to treat the atrial fibrillation. That procedure is called the Cox-MAZE procedure and involves creating electrical “guardrails” that block re-entrant electrical circuits sustaining atrial fibrillation. The original Cox-MAZE procedure, designed by Dr. Jim Cox, involved cutting atrial tissue to establish these lines that block electrical circuits. We use cryothermy to accomplish the same thing and many groups use radiofrequency ablation.
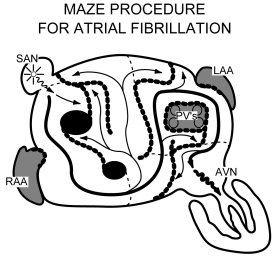
Perhaps the most important part of the procedure involved ligating or oversewing the left atrial appendage which is thought to be the source of strokes associated with atrial fibrillation. Adding the Cox-MAZE procedure to a robotic mitral repair adds an additional 30 minutes or so of operative time and is not difficult. The lesion set (pattern of the blocks or “guardrails” is also important and extremely variable. We believe the best results are obtained with performance of a Cox-MAZE IV procedure with cryothermy applied to both right and left atrium. This is debatable but is our opinion. Hope this helps.
Many thanks to Kerrigan, Simone and Tina for their questions and a special thanks to Dr. T. Sloane Guy for sharing his clinical experiences with our patient and caregiver community. To learn more about Dr. Guy, click here.
Keep on tickin!
Adam
|
Kerrigan says on December 20th, 2012 at 7:24 pm |
|
Thank you to you Adam, and the surgeons, for taking the time to reply to my question. Settles many issues in my mind; again, thanks for your wonderful website!! |
 |
|
Ralph Gilliam says on January 8th, 2013 at 2:33 pm |
|
What is the normal size opening of an aortic valve? |
 |