Cow Valve Replacements: 5 Important Facts
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: May 11, 2025
When heart valve disease progresses to the point that it is severe and the valve anatomy is un-repairable, the defective heart valve must be replaced. At that time, patients and their medical teams will need to decide what type of replacement valve should be used.

Typically, the choice is between mechanical heart valves and tissue heart valves. Mechanical valve replacements are made from very durable materials such as titanium and carbon. Tissue heart valve replacements, also known as biological or bioprosthetic valves, are harvested from pigs (porcine heart valves) or constructed from the tissue sac (the pericardium) surrounding the heart of a cow (bovine).
Both mechanical and tissue valves are designed to mimic the function of a natural, healthy heart valve
To hear “pig valve” or “cow valve” as a choice for heart valve replacement options can be quite peculiar, even alarming for a patient. In a strange twist of evolutionary coincidence, however, human valves and cow valves are very similar in tissue physiology, which makes them a frequent choice for heart valve replacement.
What is the process to create a heart valve replacement using the pericardium tissue of a cow? What are the pros and cons of cow valve replacements? To find out, keep reading below!
Harvesting the Cow Valve Tissue
Unlike a pig valve replacement, a cow valve uses the tissue of the cow’s heart – not the actual heart valve structure itself.
The size of an actual cow valve is too large compared to a human heart valve. A cow valve would not fit in a human heart.
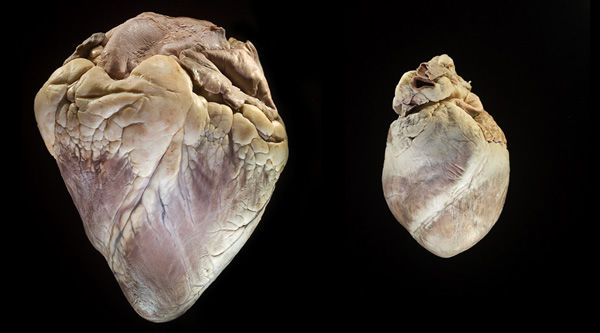
In fact, the bovine valve structure (e.g. the annulus) is actually not used at all. Instead, during a very sophisticated manufacturing process, the tissue from the cow’s pericardium (the tough tissue sac that surrounds the cow’s heart) is used to create the leaflets that open-and-close as blood flows through the new heart valve replacement.
Once the tissue sac is removed from the cow, it is processed into the proper shape and, for most valves, chemically treated with glutaraldehyde – a disinfectant used to kill germs – to preserve the tissue and remove any live cells that might cause the patient’s body to reject the valve after it is implanted in the human body.
The newly constructed cow valve may also treated with an anti-calcium building solution and/or process that helps reduce one of the main causes of heart valve disease known as stenosis.
For example, the INSPIRIS RESILIA heart valve by Edwards Lifesciences uses several novel technologies to enhance durability. This valve is not stored in glutaraldehyde.
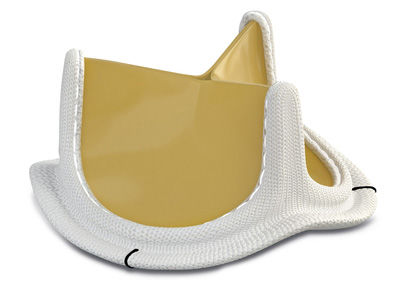
The FDA approved the Perceval Sutureless Aortic Valve by Corcym that can be delivered and fixed into the heart faster than traditional valves. Using this cow valve replacement, patients are often on the heart-lung machine for a shorter period of time.
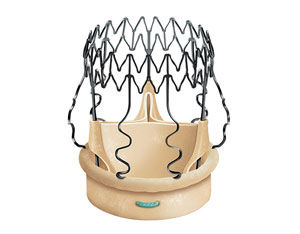
Prior to implant, cow valve replacements undergo rigorous quality testing to ensure the valve is durable enough to be used in surgery.
Cow Valve Replacement By Open Heart Surgery
The traditional approach to heart valve replacement is surgical valve replacement or “open heart” surgery.
The patient is put under a general anesthetic. The surgeon makes an incision in the chest to access the heart through a median sternotomy, which is the division and spreading of the sternum. Open heart surgery requires the use of a heart-lung machine to stop the heart. The heart-lung machine does the work for the heart while it is stopped. This allows the surgeon to access the diseased heart valve. The surgeon then removes the damaged valve and replaces it with the new valve.
After the valve is replaced, the heart is restarted and the incision is closed.
Cow Valve Replacement Surgery: Transcatheter Aortic Valve Replacement (TAVR)
During a TAVR procedure, the surgeon inserts a pencil-thin tube called a sheath into a femoral artery in the leg. Through that sheath, the surgeon uses image guidance to send a balloon catheter through the artery to the aortic valve. The balloon is inflated to open the damaged heart valve and then deflated and removed.
Next, the surgeon places the transcatheter heart valve over a deflated balloon on a very thin tube and threads it to the aortic valve. Once positioned in the aortic valve, the balloon is inflated, expanding the new valve within the diseased one.
Your surgeon removes your damaged heart valve and implants the bioprosthetic cow valve in its place. The implanted valve immediately starts opening and closing, allowing blood to leave the heart and preventing it from leaking back in. The balloon is then deflated and the delivery system is removed. The new heart valve begins to work immediately.
The patient’s heart beats throughout the entire procedure.
Here's the patient success story of Jean Frank, a yoga-enthusiast who recently received a TAVR.
Should I Go With a Mechanical or Tissue Valve?
A patient’s choice between a mechanical or tissue heart valve replacement involves weighing the major advantages and disadvantages of both valve types.
Your surgeon and medical team can help guide you based on several factors and criteria including: Health, unique heart and valve condition, age, gender, lifestyle and life expectancy.
 Mechanical Heart Valve Replacement
Mechanical Heart Valve Replacement
Some studies have shown that heart valve recipients report the same quality of life whether they receive a replacement mechanical or tissue valve.
What are the Advantages of Cow Valves?
One major advantage of tissue valves is that cow valve replacements usually do not require long-term blood-thinning medication (e.g. warfarin, Coumadin) to prevent the development of blood clots that can form on the new valve.
For most tissue valve patients, taking an aspirin a day may be sufficient therapy while other patients do not use any blood thinners.
Compared to mechanical valves, tissue valves do not increase the likelihood of blot clot formation and severe bleeding. This makes tissue valves more suitable for patients who have a high risk of clotting or bleeding.
Women who plan to have children also may prefer a tissue valve because, for most patients, warfarin use during pregnancy is not advised due to the risk of fetal malformations.
What are the Drawbacks of Cow Valves?
Durability is one of the key considerations for patients when selecting a heart valve replacement device. While new technologies are being designed and tested, cow valve replacements typically last between 10-20 years. The main advantage of mechanical valves is that they are very durable and expected to last the life of the patient.
Younger patients (under 65) who opt to have cow valve replacement surgery may need to have a re-operation at a future time. That durability makes mechanical valves preferred in younger patients who otherwise would likely require subsequent re-operations.
Another drawback for cow valve replacements is that animal tissue valves are often more susceptible to calcification on the valve leaflets following a heart valve replacement operation. This can lead to deterioriation.
Some cons cut across both mechanical and tissue valve replacements: For example, patients with replaced heart valves are at increased risk for developing an infection of the valve, known as endocarditis.
Cow Valve Replacements Can Be A Great Option for Patients
About 65,000 heart valve replacements are performed every year in the United States for conditions including aortic stenosis and mitral stenosis. Thanks to medical companies who are developing new valvular technologies and solutions, patients are offered an incredible variety of heart valve replacement options.
Cow valve replacements are a popular choice for patients. These bovine valves can restore blood flow in the heart which ultimately provides patients a wonderful possibility of returning to their normal lifestyle with a healthy heart.
Keep Learning About Heart Valve Replacements
To help educate and empower you about heart valve replacement devices, you may also like:
- Heart Valve Learning Center for Patients
- Mick Jagger's Heart Valve Surgery: 5 Facts To Know
- Meet Patients Like You In Our Community!
References:
American Heart Association, Options and Considerations for Heart Valve Surgery. heart.org/heartvalvesurgery
St. Jude Medical. https://www.sjm.com/en/patients/heart-valve-disease/treatment-options/heart-valve-replacement?clset=af584191-45c9-4201-8740-5409f4cf8bdd%3ab20716c1-c2a6-4e4c-844b-d0dd6899eb3a
Stanford Medicine. https://sm.stanford.edu/archive/stanmed/2014spring/article6.html
US National Library of Medicine National Institutes of Health. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4526499/ Very Well Health.
Very Well Health
https://www.verywellhealth.com/heart-valve-replacements-3156939
Claret Medical
https://www.claretmedical.com/intl-replacing-aortic-valve-savr-vs-tavi/
NCBI
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5808613/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMvfC4989657/ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5961329/
Your Health Plus. “How Cows Are Helping Save Hearts.” https://yourhealthplus.suttereastbay.org/2012/08/02/heart-valves/
Microscopy UK
https://www.microscopy-uk.org.uk/mag/artnov10macro/Kaitlin_Corbin/KCorbin_heart_valves.html




