Facts About TAVR

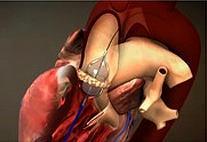
Transcatheter aortic valve replacement (TAVR) is a non-invasive treatment for severe aortic stenosis patients that does not require open-heart surgery or an incision to the patient’s chest.
Watch Video