Surgeon Q&A: What 5 Facts Should You Know About Pediatric Heart Valve Surgery?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Dr. Sameh Said, Pediatric Cardiac Surgeon
Published: July 16, 2020
Since launching HeartValveSurgery.com in 2006, we have struggled creating educational resources for parents of children with heart valve disease.
Today, I am happy to report that our struggle may be coming to an end. Over the next several months, we will be posting content specifically for parents of children with valvular defects that impact the aortic, mitral, tricuspid and pulmonary valves.

For our first post, I was fortunate to connect with Dr. Sameh Said, the Associate Professor of Surgery and Pediatrics, Division of Pediatric Cardiovascular Surgery, Masonic Children’s Hospital at the University of Minnesota, in Minneapolis, Minnesota. As you can see here, Dr. Said has successfully treated many patients in the heart valve community.
 Dr. Sameh Said
Dr. Sameh Said
Here are the important highlights from my interview with Dr. Said:
Fact 1: What should parents know about the key determinants for timing heart valve surgery in children?
Dr. Said: This is a very important question for parents to know given the complex progression of heart valve disease. The key determinants for timing interventions include:
- Ability of the child to grow and feed normally. Children especially infants – unlike adults – have this amazing ability to remain asymptomatic even with a severe degree of valvular dysfunction. However, one of the earliest signs that draws the attention of the pediatricians, and pediatric cardiologists – especially in infants – is their growth curve pattern and the ability to gain weight appropriately. Lack of proper growth/weight gain compared to peers tells us: it is time to do something.
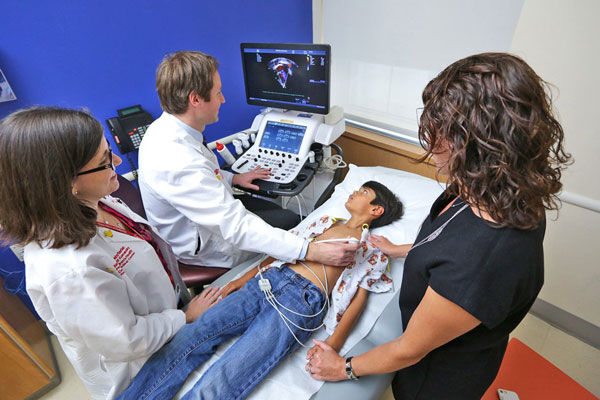 Child Having An Echocardiogram
Child Having An Echocardiogram
- Echocardiographic parameters. The use of echocardiograms (ultrasound) enable surgeons to obtain a great amount of information about the condition and the functioning of a child’s heart. When surgeons evaluate the timing of an intervention, the parameters we closely look at include:
- Ventricular chamber size. As valve disease progresses, there are changes that start to affect the related cardiac chamber (pumping chambers) which we can see on echocardiography. The ventricle size may enlarge or the wall thickness may increase. This signals the progression of the valve pathology and may indicate timing to intervene.
- Heart function. As the valve disease progresses, the next changes that affect the heart will be reflected in its function. Heart function is an important parameter that determines the timing of valvular intervention, and ideally, it is better to intervene prior to any drop that occurs in the heart function. This is an important prognostic factor for outcomes after surgery as well and below normal function continues to be one of the important risk factors for poor outcomes after surgery.
- Associated defects. Sometimes the child may have a less severe leakage or narrowing in a particular valve that does not per se meet criteria for intervention, however there are other concomitant heart defects that need to be fixed such as a large hole in the heart that requires closure. This my push doctors to evaluate the valve at the same time and try to repair it so as long the child will be in the operating room anyway.
Fact 2: Is there a preferred treatment for children with heart valve disease?
Dr. Said: When possible, we always prefer to repair, or reconstruct, a defective valve instead of replacing it. Children’s valve diseases are treated differently compared to adults from several aspects. In children, we think a lot about quality of life, difficulty in managing blood thinners, activity restriction, and more importantly growth. These factors affect the timing of interventions, choice of technique of repair, or type of prosthesis that will be used if we are forced to replace the valve.
As an example: if we don’t have options for repair, we may delay intervention on the valve or delay a big operation such as Ross Procedure until the child is a bit bigger where we can have more options. We may also accept less than perfect results in repairing the valve to avoid the drawbacks of replacement.
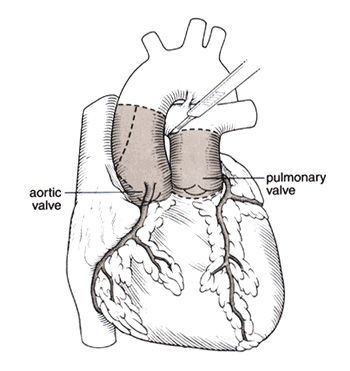 Ross Procedure
Ross Procedure
Fact 3: How should parents think about managing heart valve disease during their child’s life?
Dr. Said: As referenced above, prosthetic heart valve replacements have major limitations due to impairment of growth potential. For this reason, there is an increased need for repeat interventions/operations especially in infants and smaller children.
As parents consider the lifetime management of heart valve disease, it is important for them to:
- Follow-up and consistency are the keys to success. Regardless of repair or replacement and even prior to any interventions, it is important to follow-up with your cardiologist and adhere to his/her recommendations and to the medications. This way, interventions are done on time and before irreversible changes occur in your child’s heart.
- Parents also should request a visit with the surgeon. Parents do not have to wait until the cardiologist refers them. Meeting with the surgeon does not mean that the child has to have surgery. However, it is important to listen to the surgeon and understand his/her strategy of addressing the valve problem when the time comes. Discussion about the surgeon’s approach and results are always helpful to alleviate a lot of the anxiety and stress when the time for surgery comes.
- After replacement with a prosthesis… If there is a need for blood thinner use, as an example, parents have to follow the instructions related to timing of anticoagulant administration, and the need for a blood test to adjust the dose of the blood thinners appropriately.
 Dr. Sameh Said with Patient
Dr. Sameh Said with Patient
Fact 4: How have transcatheter procedures helped children with heart valve disease?
Dr. Said: Transcatheter options are valuable for the right patient and can be used as a primary treatment modality or go hand-in-hand with the surgical interventions to minimize the number of future re-operations for children.
Transcatheter valvular interventions play a major role these days in the following scenarios:
- Children born with narrow (stenotic) aortic or pulmonary valves, where balloon dilation can be done with good results which relieves the obstruction and buys more time prior to any surgical interventions.
- Transcatheter valve replacement can be performed in the pulmonary position either as a primary procedure or after previous placement of a pulmonary prosthesis. Such as patients who underwent previous repair of tetralogy of Fallot as infants.
- The “valve-in-valve” technology is available for those children who underwent surgical valve replacement with biological valves and now require re-interventions. Transcatheter therapy can be done in these cases to delay the timing of repeat operation. I have done transapical (limited incision in the left chest) to expose the apex of the heart and deliver a transcatheter valve in the mitral position in children who had previous mitral valve replacement with biological valves. This can be a good alternative to children with small groin vessels that do not allow a completely transcatheter approach.
A result of these non-invasive, transcatheter procedures, patients typically experience less pain, shorter time in the hospital, and an accelerated recovery.
Outcomes for transcatheter procedures in children have been excellent with very low risk of major complications and satisfactory results.
Fact 5: Are there any emerging technologies that parents should know about?
Dr. Said: Yes, there are emerging heart valve replacement devices that may have the potential for growth with the child, which may delay the next operative intervention.
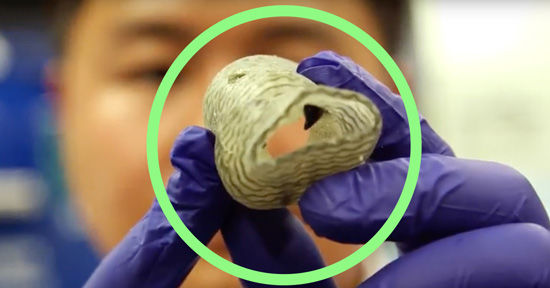 3D Bio-Printed Heart Valve
3D Bio-Printed Heart Valve
We always think about children’s growth when time comes for valve interventions. In general, we try to minimize or avoid the use of prosthetic materials that do not have the potential for growth or restrict the growth of the child.
- There are recent devices that we use as adjuncts during repair of the heart valves that have the potential for growth but we do not have robust long-term data yet.
- There are procedures such as the Ozaki and Ross for aortic valve replacement that are reserved for children due to the potential for growth.
- Technology of 3D bio-printing is already available and it has the potential for creating valves and conduits that has the potential to grow. The future is already here.
Thanks Parents! Thanks Dr. Said!
Many thanks to the parents of children with heart valve disease for reading and learning from this post. We are hopeful that this information helps you learn more about the management and treatment of heart valve disease for your children.
I would also like to extend a mighty “Thank You!” to Dr. Sameh Said for taking the time to share his clinical experiences and research with our community. It is great to have a pediatric cardiac surgeon on the HeartValveSurgery.com team!!!
Related links:
- Top 8 Facts About Pediatric Aortic Valve Surgery
- To see patient reviews and a lecture by Dr. Sameh Said, click here.
- FDA Approves Smallest Heart Valve Replacement for Children
Keep on tickin!
Adam





