Aortic Valve Disorders
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: February 14, 2026
Within the heart, four valves function as trapdoors to ensure a one-way flow of blood. Flaps, also known as cusps or leaflets, on the valves open to let blood through and then close tightly to prevent backflow. If the valves cannot open fully or close completely, the heart may receive an insufficient supply of blood in the chamber where it is needed.
Experts estimate that aortic stenosis is present in approximately two percent of those who are over 65, three percent of those over 75, and four percent of those over 85. Some patients with aortic valve stenosis, like me, are never aware of any symptoms.
Types of Aortic Valve Disorders
There are a few types of aortic valve disorder.
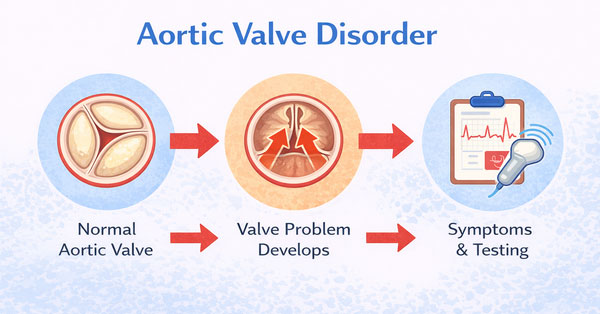
- Aortic valve stenosis is a narrowing or obstruction of the valve. As shown below, the flaps on the valve cannot open widely enough for sufficient blood to pass. This condition accounts for the largest number of surgeries to correct a damaged heart valve.
- The second type of malfunction is aortic regurgitation. In this condition, the valve leaks, allowing blood to flow back into the left ventricle from the aorta.
Aortic stenosis is most often caused by calcium deposits building up on the flaps of the aortic valve. This normally occurs in older patients. The second most common cause is a congenital heart defect known as a bicuspid aortic valve. A normal aortic valve has three heart valve flaps, but some babies are born with an aortic valve that has only two flaps. The cause of this defect is not known, but there is no evidence that it can be prevented during pregnancy. Although cases of rheumatic fever, a complication of a strep infection, have been virtually eliminated in the United States, many older individuals or those from other countries may have suffered damage to the heart from the disease. Calcium deposits account for roughly half of all aortic stenosis cases. If the calcification occurs on a bicuspid aortic valve, symptoms will likely manifest during middle age.
Aortic Valve Disorder Symptoms & Diagnosis
With a normal valve, the patient may remain asymptomatic until his seventies or eighties. However, other conditions, such as diabetes or high blood pressure, can hasten the process.
Aortic stenosis disease can progress quickly, and, once it worsens, surgery is normally required. Typically, patients will develop symptoms that include:
- Chest pain
- Shortness of breath
- Fainting episodes
- Atrial fibrillation
- Swollen ankles
Typically, patients with aortic regurgitation remain symptom-free until they are middle-aged. They may experience chest pain, or, in severe cases, heart failure. Normally, however, the condition is caught during a visit to the doctor for a physical or unrelated reason. The physician may hear a murmur when listening to the patient's heart with a stethoscope.
This sound is caused by the abnormal flow of blood moving across the valve. Hypertension, endocarditis, and congenital defects are all associated with the development of aortic regurgitation. Treatment for aortic valve disorders depends on the patient's age, health, and the impact the disorder has on normal functioning of the heart as well as the cause of the disorder. The physician has several tests at his disposal to confirm a preliminary diagnosis and to evaluate the degree of dysfunction. He will likely ask the patient to submit to one or more tests prior to recommending a treatment plan. The standard diagnostic test for heart disease has long been the electrocardiogram, or ECG.
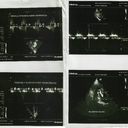
Abnormalities in the ECG are often clues to an aortic valve disorder, but the ECG may not be conclusive in and of itself. An ultrasound test known as an echocardiogram is the preferred non-invasive method of evaluating the aortic valve. Calcification and, in advanced cases, an enlargement of the heart, may be present in a chest X-ray. The physician may also perform cardiac catheterization. This procedure provides an accurate measurement of the pressure being exerted on each side of the aortic valve, which can be useful in determining treatment.
Surgical Treatment of Aortic Valve Disorders
If necessary, the aortic valve can be repaired or replaced with a synthetic or biological valve. Patients receiving a biological valve replacement may need to take anticoagulants for a short time after surgery, but those receiving a synthetic, or mechanical valve replacement, must take blood thinners (e.g. Coumadin) on a permanent basis.
It is sometimes possible to repair a defective valve, particular if it is bicuspid. An infant or child with aortic stenosis may benefit from a procedure where a deflated balloon is threaded through an artery to the valve and then inflated to stretch the stenotic valve. Medications are generally ineffective in treating a disorder, but may sometimes be used to alleviate the patient's symptoms or control other conditions that may aggravate the disorder.
Transcatheter Aortic Valve Replacement
You should also know that there are transcatheter heart valve therapies that treat aortic valve defects without breaking the patient's chest or ribs. Transcatheter aortic valve replacement (TAVR), is a unique procedure that replaces with the patient's defective valve without the need of the heart-lung machine and the patient is not always required to go under general anesthesia. To learn more about TAVR, click here.
You May Also Like
To help you learn more about aortic valve disorders and treatment options, you may like: