Pulmonary Valve Regurgitation
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: May 14, 2025
Pulmonary regurgitation is an incredibly common condition – in fact, up to 90 percent of Americans have some form of it, according to the Children's Heart Specialists of Kentucky.
That said, most people don't show any symptoms of pulmonary regurgitation and don't need any type of treatment. Severe cases, though, require regular monitoring, medications to relieve symptoms and even surgery to insert an artificial valve or tube.
What is Pulmonary Valve Regurgitation?
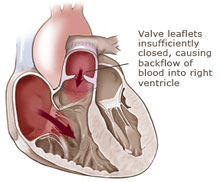
Pulmonary regurgitation occurs when the pulmonary valve in the heart doesn't operate properly. During a regular heartbeat, the lower right chamber of the heart, called the right ventricle, pushes blood through the pulmonary artery into the lungs. If the valve in the pulmonary artery doesn't close completely, blood can leak back from lungs into the heart between heartbeats.
Most people don't exhibit symptoms of pulmonary regurgitation, and infants or children born with the condition typically don't show signs of it until they are older. Many of the more severe cases of the disorder appear in people who have had heart surgery to insert an artificial conduit between the right ventricle and pulmonary artery. People who do exhibit symptoms often have a severe form of this condition.
What are the Symptoms of Pulmonary Valve Regurgitation?
Patients with a serious case of pulmonary regurgitation may experience the following symptoms:
- Fatigue
- Difficulty breathing, especially when exercising or engaging in other intense physical activity
- Fainting or dizziness
- Heart murmur
- Arrhythmia
- Palpitations, or rapid or irregular heartbeats
- Chest pain, including pressure, squeezing and tightness
- Swelling in the feet or legs
- Bluish lips or nails
How is Pulmonary Valve Regurgitation Diagnosed?
Doctors are often keyed into the possibility that a patient might have pulmonary regurgitation if they notice abnormal sounds in the chest, an enlarged liver, fluid retained in the ankles or a distended jugular vein in the neck.
While doctors begin a diagnosis by checking a patient's symptoms, medical history and performing a physical exam, certain tests must be done to confirm pulmonary regurgitation. It can be revealed through a chest X-ray; a cardiac MRI, which creates a 3D image of a heart; an echocardiogram, which uses sounds waves to map the heart; or an electrocardiogram, which records the heart's electrical activity. Other diagnostic methods include pulse oximetry, which painlessly monitors oxygen levels in blood, and cardiac catheterization, in which a thin tube is guided into the leg or belly button and through a blood vessel into the heart.
How is Pulmonary Regurgitation Treated?
Trivial cases of pulmonary regurgitation do not require immediate treatment, and some doctors feel that these cases don't even need regular checkups. Moderate or severe pulmonary regurgitation, though, needs monitoring, and if it worsens, surgery might be necessary.
Currently, there are no medications that treat the root problem of pulmonary regurgitation, but some drugs can alleviate its symptoms and help the heart beat more normally. These medicines are often diuretics that flush extra water from the body or drugs that help hearts beat more regularly in conditions such as palpitations and arrhythmia.
In severe cases, doctors might determine that the valve needs to be replaced or repaired and its function improved through a surgical procedure called valvuloplasty. At this point, a patient's options include having the pulmonary valve removed and replaced with a new one or having an artificial conduit placed between the pulmonary artery and right ventricle.
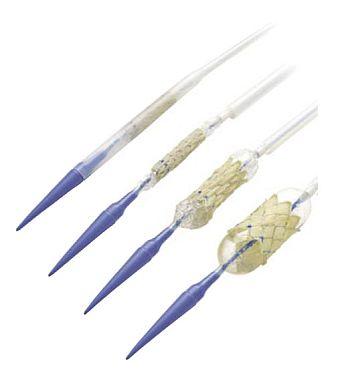 Melody Pulmonary Valve Replacement
Melody Pulmonary Valve Replacement
One of the newest types of valves, the Melody valve, is a transcatheter procedure that does not cause any trauma to the patient's chest or ribs. Instead, the valve is put into a patient through a catheter in a leg blood vessel. For children, one of the best choices is a pulmonary homograft. This donated pulmonary valve and artery can grow with the child.
In the future, doctors might be able to harvest a patient's cells and use them to grow a new valve on a biodegradable mesh. This treatment is still being worked on and isn't performed yet.
You Might Also Like
To help you learn more about pulmonary regurgitation, here is additional information and patient updates:





