Mitral Valve Repair: Different Approaches for Different Patients
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Medical Expert: Joanna Chikwe, MD, Chair of Cardiac Surgery at Cedars-Sinai Medical Center
Page Last Updated: July 9, 2025
It’s no secret.
If you have severe mitral regurgitation, the recommended procedure for most patients is a mitral valve repair. Compared to a mitral valve replacement, patients who undergo a repair benefit from long-term durability, freedom from re-operation, no prolonged use of blood-thinning medications, and a normal life expectancy.
However… In 2025, patients seeking a highly-skilled medical team capable of performing a mitral valve repair are often confused by the different surgical and transcatheter approaches currently available.
To answer your questions about the different types of mitral valve repair operations, I just interviewed Dr. Joanna Chikwe, the Chair of Cardiac Surgery in the Smidt Heart Institute at Cedars-Sinai Medical Center in Los Angeles. Dr. Chikwe is a long-time supporter of HeartValveSurgery.com who has successfully treated many patients in our community including Joey Nakazawa, Chris Fager and Patricia Reuter. Here are the highlights from this important interview:
Key Insights About the Different Types of Mitral Valve Repair Surgery
Dr. Chikwe shared several important points during this interview that I want to highlight for our patient community:
- Dr. Chikwe has specialized on heart valve surgery in her practice because valvular procedures have a profound and positive impact on the quality of life for her patients. Heart valve surgery, according to Dr. Chikwe, is challenging, demanding and rewarding.
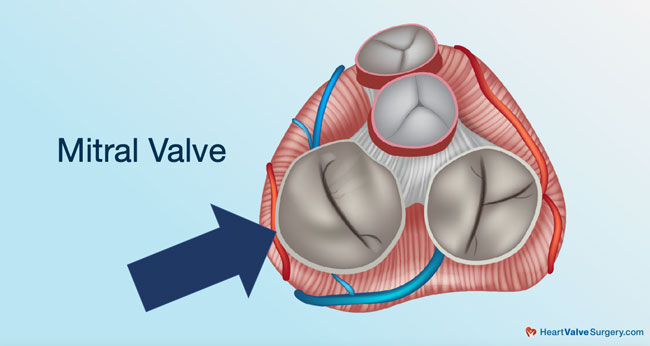
- Mitral valve repair operations are typically reserved for patients who have mitral regurgitation, a leaking valve. There are two causes of mitral regurgitation including (i) functional mitral regurgitation in which the valve leaflets pull apart and (ii) floppy mitral valve regurgitation (mitral valve prolapse) which impacts up to 7 million people.
- Dr. Chikwe believes there are “5 things” patients with mitral regurgitation should know about symptoms related to this disease. Patients may be asymptomatic (without symptoms). Patients may feel “winded” and short of breath. Patients may experience heart palpitations caused by atrial fibrillation. Patients may have chest tightness. And, patients can be fatigued.
- Life expectancy is a big consideration for mitral regurgitation patients who need a mitral valve repair. According to Dr. Chikwe, if a patient receives a great mitral valve repair, there is a very good possibility they will have a normal life expectancy. Unfortunately, if a patient waits to get treatment for mitral regurgitation, that delay can negatively impact their life expectancy.
- Dr. Chikwe considers a sternotomy (an incision through the chest), which is a very effective approach during open-heart surgery, to be the “old gold standard” for mitral valve repair.
- The “new gold standard” for Dr. Chikwe uses robotic assistance for reconstructing the mitral valve through minimally-invasive incisions near the ribs. Benefits of robotic surgery for Dr. Chikwe’s patients include tiny incisions and accelerated recoveries.

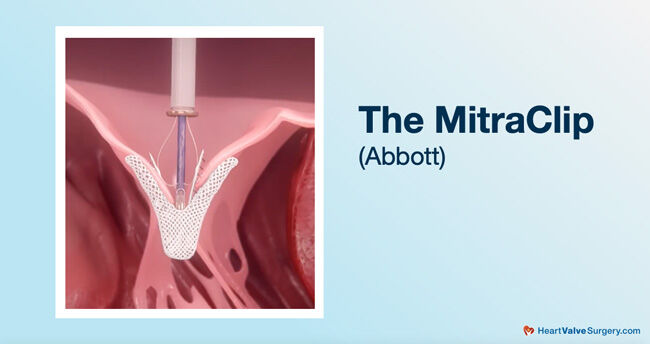
- According to Dr. Chikwe, the MitraClip is a “Game Changer” for patients with functional mitral regurgitation who did not have many surgical options available to them prior to the development of transcatheter mitral valve repair (TMVR) devices. There is no incision to the patient’s chest or ribs during this TMVR procedure. The MitraClip “clips” the mitral valve leaflets together to prevent back-flow of blood. Patients who get a MitraClip implanted often leave the hospital the next day.
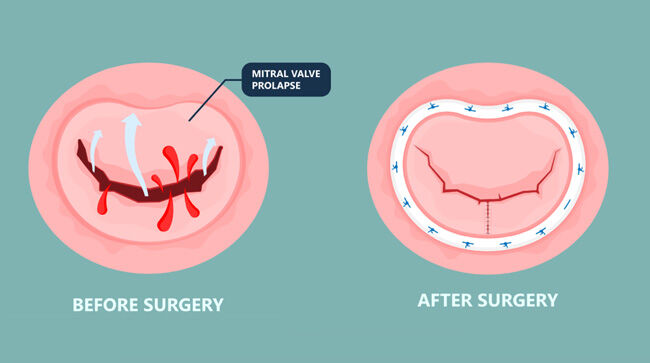
- Dr. Chikwe leverages several techniques to repair a mitral valve including (i) triangular reduction of floppy mitral valve leaflet tissue, (ii) annuloplasty ring implantation to support the mitral valve and bring it together, and (iii) implantation of mitral chords.
- For patients suffering from atrial fibrillation (AFib), Dr. Chikwe uses the Maze Procedure to minimize the risk of stroke caused by AFib. Other concomitant procedures during mitral valve repair include fixing the tricuspid valve, PFO closure, coronary bypass graft and additional heart valve therapies.
- In the future, Dr. Chikwe sees a continued and rapid evolution of minimally-invasive techniques for mitral valve repair techniques. According to Dr. Chikwe, randomized clinical trials will help evaluate the success or failure of these new devices.
- It is very important for patients to discuss mitral valve repair approaches with their cardiologists and their surgeons. Certain surgical procedures are better suited for younger patients needing mitral valve repair surgery while the MitraClip could be a viable option for older, higher-risk patients.
- Dr. Chikwe’s top advice specific to mitral valve repair is that patients should ask their potential doctors, “How many repairs have you done successfully in patients that look like me with my valve anatomy?” According to Dr. Chikwe, patients want the answer to that question to be “hundreds” of mitral valve repairs.
Thanks Dr. Chikwe & Cedars-Sinai!!!
On behalf of our patient community, I would like to thank Dr. Chikwe for taking the time to share her clinical experiences and research specific to mitral valve repair. I would also like to thank all of the great people at Cedars-Sinai who have helped so many patients from HeartValveSurgery.com.
Related Posts:
- See 75+ Patient Reviews for Dr. Joanna Chikwe
- Patient Video: Leila’s Robotic Mitral Valve Surgery Success
- Mitral Valve Leaflets: 7 Important Facts to Know
Keep on tickin!
Adam
P.S. For the hearing impaired members of our community, I have provided a written transcript of my interview with Dr. Chikwe below.
Video Transcript
Adam Pick: Hi, everybody, it’s Adam with heartvalvesurgery.com. This is a special surgeon question and answer session all about traditional, robotic, and transcatheter mitral valve repair surgery. I am thrilled to be joined by Dr. Joanna Chikwe, who is not just the Chair, she’s the Founding Chair of Cardiac Surgery at the Smidt Heart Institute at Cedars-Sinai in Los Angeles, California. Dr. Chikwe, are you there?
Dr. Joanna Chikwe: Yes, I am, Adam. Great to see you.
Adam Pick: Great to see you, Dr. Chikwe. For the folks out there who may not know you, you are a long-time supporter of heartvalvesurgery.com, and you’ve performed a lot of successful mitral valve surgery on folks like Joey Nakazawa, or Arthur Hill, or Patricia Reuter. On behalf of all of us here, thanks for your support over the years.
Dr. Joanna Chikwe: It’s an absolute pleasure. I think heartvalvesurgery.com is a really phenomenal website, an amazing resource. It’s full of really helpful patient-centered information and feedback, so genuine privilege and a pleasure to be here.
Adam Pick: Wow, thanks so much for the kind words. It means a lot. Let’s get to the topic at hand. Just before we get there, I want to ask you a question all about you, Dr. Chikwe. There’s a lot of things available to cardiac surgeons out there to focus on, but valve therapy – and we’ve known each other for a long time, maybe ten years or so – has always been a big part of your practice. Can you talk about why repairs and replacements are so important to you in your practice there at Cedars?
Dr. Joanna Chikwe: We do what we love doing. There’s something very special about repairing a mitral valve, repairing an aortic valve, or tricuspid valve. Every single valve is different. It’s incredibly great. It’s very demanding. Most importantly, it makes such a profound difference to patients if you can repair it and repair it well rather than replacing it.
Adam Pick: You have repaired, and you have replaced lots of valves over your lifetime. Today, we’re talking about repairs. Maybe we can start though, and just help the patients understand repairs are typically done for mitral regurgitation. Correct?
Dr. Joanna Chikwe: That’s absolutely correct. The commonest causes of mitral valve regurgitation, so that’s a leaking mitral valve, the heart pump may have stretched. It just pulls the mitral valve leaflets apart, so they don’t come together so well, so the valve leaks. That’s called functional mitral valve regurgitation. Then the mitral valve regurgitation that is really rewarding to repair because it’s one of the things that helps that patient have a normal life expectancy is mitral valve rotation due to a floppy valve. That’s really common. Maybe 7 million Americans walking around with a floppy mitral valve.
Adam Pick: Dr. Chikwe, we’ve heard that this disease can often be under-diagnosed and under treated. If people are just hearing about the buzz term, mitral regurgitation, what symptoms might they be experiencing if anything?
Dr. Joanna Chikwe: I think there are probably five things that you might want to think about. The first one is you may feel nothing. You may feel perfectly fine. Somebody’s put a stethoscope on your chest, and they’ve heard what we call a heart murmur. That’s probably one of the commonest things that we hear. The next thing is people feel winded when they’re doing their normal activities. You’re walking upstairs. Suddenly you find yourself having to stop halfway up and catch your breath. You might feel winded in bed at night and feel that you need to sit up to catch your breath or get up and walk around.
That’s a really important symptom. That makes us worry that you’re starting to suffer from heart failure. Feeling palpitations is really common, that can be caused by atrial fibrillation, and occasionally chest tightness. One really common symptom, and I wouldn’t tell people to worry about this because we all feel this, but one of the commonest is just fatigue. I feel exhausted all the time. It’s amazing how often after mitral valve surgery that feeling of fatigue goes away. I never promise that to patients because it’s not always their valve, but it’s really interesting how that can be a real hallmark sign.
Adam Pick: I’m sure that patients are thinking, God, if I can move past those symptoms for a better quality of life, that’s what I’m looking for. Life expectancy is a really big question for patients. If they were to have a mitral valve repair, can they get back to a normal life expectancy?
Dr. Joanna Chikwe: Okay, that is such an important question. Really, that’s central to the surgical treatment of mitral valve regurgitation. We are all about trying to get a patient back to a normal life expectancy. If you have a floppy mitral valve that leaks, and you can get that repaired really well before you start having symptoms, that’s what’s going to get you a normal life, a normal life expectancy, and a normal quality of life.
If you wait until you start to feel symptoms, or until your heart has started to stretch on an echocardiogram, that’s already dropping your life expectancy. If you end up with a valve replacement instead of a valve repair, that really starts to impact your life expectancy. A replacement is better than nothing, but a valve repair done surgically that last’s, well, that’s the best of all.
Adam Pick: There’s nothing better than hopefully getting the patients back to a full and normal life expectancy. Dr. Chikwe, let’s talk about how you and your team at Cedars-Sinai get the patients there. Let’s first talk about an access point that you use, which is known as a traditional approach, which is the sternotomy. What happens when you use that approach with patients?
Dr. Joanna Chikwe: The traditional way of doing this around America would be an incision probably about some places that size. My approach is about that size. Through the middle gives you great access. All I can say is – and I tell the patients this, this hurts so much less than you think. Your nerves come together here. There’s a little gap where there’s not a lot of nerves. This is a relatively pain-free approach. It’s super safe. It’s the old gold standard.
Adam Pick: I’ve also heard that surgeons can access the mitral valve through the ribs. Is that right?
Dr. Joanna Chikwe:That’s absolutely right. While I would talk about sternotomy as the old gold standard, for me, the new gold standard is through the ribs. It’s again, it’s a small incision. The way that we can do that safely and get you a beautiful mitral valve repair is we use a robotic to assist us. The reason that is so important is that instead of me looking at your mitral valve, which is about that size down a deep dark hole in the distance, I have a huge, 3D color screen. I’ve got beautifully delicate, precise instruments. That allows me to do a super precise incision and a super precise repair. The benefit for patients is they have a tiny incision. They’re going to recover quickly. Pretty similar to a sternotomy, but so many people prefer it.
Adam Pick: That sounds really neat, a robot assisting you through a surgery. Now, maybe we can talk about what’s come from the horizon to reality, which is the transcatheter. How does something like that – how do you access the heart using a catheter?
Dr. Joanna Chikwe: MitraClip, which is one of the transcatheter options, is a total game changer for many patients with mitral valve disease. I think we have to be really clear, though, which patients. Right at the beginning, we talked about functional mitral regurgitation. Your heart muscle has stretched. Your valves don’t quite meet together. That’s why it’s leaking. The mitral clip is a great option because there weren’t terrific surgical options for that.
Adam Pick: Dr. Chikwe, this Mitral Clip sounds fantastic. Can you explain how you use this technology?
Dr. Joanna Chikwe: Absolutely, but full disclosure, I do not do the MitraClip. That’s done at Cedars by interventional cardiologists who do hundreds and really just specialize in that. If you were a patient having a MitraClip, essentially, you’re going to spend a couple of hours on a table in a laboratory. They’ll get a tiny, little catheter into the vein in one of your legs, thread that up to the right side of your heart, puncture the little wall that’s between the right and left side of your heart, so that it’s no on the left side of your heart. That wire delivers a clip.
The goal of the MitraClip is to – as your leaflets come together with every single heartbeat, 60. 70, 80 times a second, that clip is just going to capture those leaflets as they come together and hold them together. For some patients, that’s enough to prevent regurgitation. Some patients need a second clip. That, because it’s just a puncture in your groin in one of the veins, allows you to go home within a few hours or occasionally the next day.
Adam Pick: Wow, so there are – there’s no incision to the sternum. There’s no incision to the ribs. The patient’s not even on the heart lung machine. It seems like for the right patient, this could be a really good solution for them. Yeah?
Dr. Joanna Chikwe: You’re absolutely right. This is a complete paradigm shift and a game changer for the right patients. The patients with functional MR, the frail patients with leaky mitral valves, and definitely the prohibitive risk patients, this is transformative. It remains to be seen. We’re all watching intensely. Is this also going to be a game changer for those surgical patients that could benefit from surgery?
Adam Pick: You talked about clipping the leaflets with the MitraClip. I’m real curious to know what other techniques might you use to fix the mitral valve?
Dr. Joanna Chikwe: That’s where this becomes just a joy for a surgeon. You have this spectrum of techniques that you can use to get a really challenging valve back into the shape that it needs to be. The commonest approach we use is to literally do a little triangle that gets rid of the piece of the mitral valve that’s floppy, join the edges together, and suddenly the whole thing just sits there looking like a perfect smile again. We bring the whole thing together with a ring because that stabilizes it long-term.
Oftentimes, that’s all you need. For patients that have got a couple of extra pieces of floppy valve, often if it’s their anterior, the front leaflet, that we can reconstruct with cords that are a bit like parachute cords. Usually when we’re in there, if you have atrial fibrillation, we will correct that with a Maze procedure and close off a little pocket in the heart called the appendage to reduce your risk of stroke.
Adam Pick: Dr. Chikwe, that was my next question all about the concomitant procedures for patients who have cardiac conditions in addition to valve disease. You mentioned afib. What else can you do during an operation on the valves?
Dr. Joanna Chikwe: Atrial fibrillation is really important. We used to regard it as a benign arrhythmia. We know it isn’t. It causes stroke. It reduces life expectancy. In any patient that has a history of atrial fibrillation, we would want them to be in the operating room with a procedure to correct that. Part of that is closing off this little pocket that I referred to, the left atrial appendage. Other things that we do at the same time as mitral valve surgery when we’re doing it through the side, fixing a tricuspid valve. That’s the mirror image of your mitral valve, but on the right side of your heart.
Oftentimes, that’s a little bit stretched. It leaks. We can fix that very easily with a ring. The other piece of the jigsaw is the little wall between those two right and left-sided chambers that often has a hole called a PFO. We can close that at the same time, very straightforward. If we’re going through a sternotomy, and sometimes it’s the reason to choose a sternotomy. Other operations we can do at the same time are coronary bypasses and aortic valve surgery. Those could be the commonest.
Adam Pick: Dr. Chikwe, you’ve talked about a lot of technology today. You talked about robots. You talked about catheters, clipping leaflets together. What do you see as the future?
Dr. Joanna Chikwe: That’s a really exciting question. I genuinely see the future as a continued focus on getting less, and less, and less invasive. You’re going through smaller incisions but achieving the same excellent long-term results. This is not about compromising the quality of the result for the patient in the short-term or the long-term. I think some of the really exciting things involve going through little punctures, and tiny incisions in the front of the chest, and placing those parachute cords without stopping the heart.
That’s a wonderful way to fix prolapse. I intuitively feel that’s a superior way to fixing prolapse and trying to clip two leaflets together. Essentially, what will tell us is a randomized trial. One of the exciting things in this area right now is there are two, three, four randomized trials comparing MitraClips and punctures through veins to surgical approaches for repairing the valve. That will tell us what’s the right answer for each individual patient that has this problem.
Adam Pick: Dr. Chikwe, with all these techniques available for mitral valve repair, I’m sure the patients are wondering, can I just choose one technique over the other?
Dr. Joanna Chikwe: That’s a really important question. For patients that are low risk, you’re young, you’re in your 60s, you’ve got nothing wrong with you, right now the best option for you is mitral valve repair done surgically. The key thing that you’re doing is choosing the surgeon that can deliver you the safest and best repair. Then there’s a group of patients that are older, maybe a little bit more wrong with their heart. We call those intermediate risk. The only way that you should be getting a MitraClip at this point in time is through one of those trials. Generally, it’s not clear that a MitraClip will give you that good, long-term outcome.
Then there’s a population of patients that are so sick, so they’re very elderly, they’re very frail, and they would have a high chance of having a bad outcome with surgery. We call that prohibitive risk. Those patients are probably best suited to a MitraClip. That’s the only indication for a MitraClip, right now, for floppy mitral valve disease. In summary, it’s a really careful discussion with your cardiologist, and the cardiac surgeon, and making the best choice with all of the information that’s tailored to you and not just Dr. Google.
Adam Pick: Yeah, Dr. Google, Doc, I’ve not heard that before. You bring up so many great points right there, which is it’s this heart team approach and bringing the patient into the decision making process along with the criteria that you so – you and your team have been working on and teams around the country, around the world, to get the best results for the patients. I’ve got to ask as we wrap up here, one of the most important questions for any patient going through this process, I’m sure they’re always collecting advice from leading clinicians like yourself. What advice do you have for a patient out there who might be considering a mitral valve repair right now?
Dr. Joanna Chikwe: I think it’s essential that you do your research. I think it’s essential that you partner with your cardiologist who has a really good understanding of the surgeons that have the expertise to give you the best outcome. One question that you should take to every visit and every consultation with a surgeon is a very simple one. It’s about how many repairs have you don’t successfully in patients that look like me with my valve anatomy. You want that number to be in the hundreds.
You want the chances, the percentage chance of you having a mitral valve repair successful, if your mitral valve prolapse would be well above 95, 99%. That’s essential. It’s very difficult to get that information just by going through Google. that’s really why partnering with your cardiologist is essential. Talking to colleagues, going online, websites like heartvalvesurgery.com, that will give you a really great insight. At Cedars, we pride ourselves. Over 1000 robotic mitral repairs, well over 99.9% repair rate.
Adam Pick: Dr. Chikwe, I can’t thank you enough for sharing that so succinctly for our patients. I know, as a patient, how challenging it can be when you’re in the office with a clinician and you forget the important questions. I hope everybody takes a moment to write down the questions that Dr. Chikwe just laid out. It really can make a big difference in who you decide to select for your procedure.
On that wonderful note, Dr. Chikwe, I cannot thank you enough for your ongoing support of heartvalvesurgery.com, and more importantly your pursuit of wonderfully functioning hearts and heart valves. You’ve been an incredible resource over the years. On behalf of all of our community, I just want to say thank you and your team at Cedars.
Dr. Joanna Chikwe: Thank you so much, Adam. I really appreciate that. It’s a genuine pleasure to join you today. Thank you very much.




