Atrial Fibrillation: A Concern for Heart Valve Patients?
Medical Expert: Dr. Marc Gerdisch, Chief of Cardiac Surgery at Franciscan Health
Page Last Updated: June 3, 2025
The realities of atrial fibrillation are often misunderstood. People with AFib are 5 times more likely to have a stroke, according to the American Heart Association. AFib can greatly compromise a patient's quality of life with debilitating symptoms including heart palpitations, chest pain, dizziness and fatigue. AFib is transforming into a global epidemic with a projected 300% growth rate of new AFib cases by 2030.
When it comes to heart valve disease... The sobering realities of AFib are amplified. According to research from Northwestern Medicine, only 38% of patients with mitral valve disease get their AFib treated during heart surgery. As a result, AFib is often ignored, under-treated and mis-treated.
To raise awareness to AFib for our patient community, we interviewed Dr. Marc Gerdisch, Chief of Cardiac Surgery at Franciscan Health in Indianapolis, Indiana. So you know, Dr. Gerdisch is a heart valve and AFib expert who has successfully treated over 100 patients from HeartValveSurgery.com. In addition, Dr. Gerdisch teaches cardiac surgeons - all over the world - how to perform a successful Cox-Maze IV procedure, also known as a surgical ablation, during heart valve surgery to treat atrial fibrillation.
Key Learnings About AFib and Heart Valve Disease
Here are several important points that Dr. Gerdisch shared during our interview:
Dr. Gerdisch is a heart valve and AFib expert having performed over 6,000 cardiac procedures including more than 4,000 heart valve procedures.
AFib is an irregular heart rhythm where the atria can move in a "chaotic" fashion. The consequences of atrial fibrillation are stroke due to a lack a normal blood flow through the atria. More specifically, the left atrial appendage is often responsible for the formation of blood clots in the heart.
Other consequences of AFib are a decrease of cardiac output and symptoms.
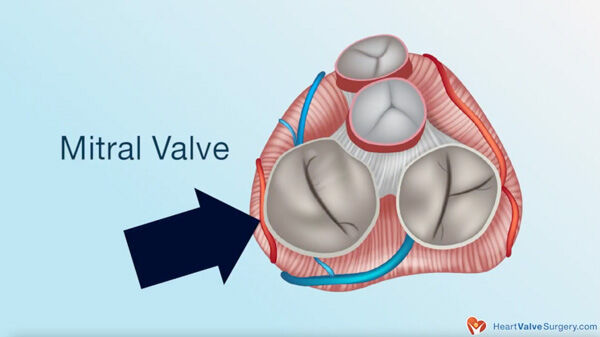
There is a higher incidence of atrial fibrillation for patients with heart valve disease. Dr. Gerdisch states, "The reason for that is largely because of the increased pressures in the atria, especially in the left atria - for example, with mitral valve disease. As the atrium expands, it becomes fibrotic, and as it fibroses, it becomes susceptible to atrial fibrillation. Atrial fibrillation is this irregular heart rhythm when there is substrate change in the muscle."
People who have atrial fibrillation can also induce changes in heart valve structures that ultimately results in cardiac disease. Dr. Gerdisch states, "For example, when the atrium enlarges - as a result of the atrial fibrillation - there are changes in the size of the mitral valve, and that valve will start to leak."
In addition to the mitral valve, the tricuspid valve is susceptible to becoming regurgitant (leaky) due to atrial fibrillation because the tricuspid valve structure is thinner, lighter and less strong.
AFib can and should be treated during heart valve surgery. (It is rare that AFib will resolve and "go away" if only the heart valve is fixed during surgery.)
The Cox-Maze IV procedure is the best form of treatment for patients, according to Dr. Gerdisch. The benefits of the Cox-Maze IV procedure include decreased risk of stroke, cardiac output efficiency, lower risk of future valve disease, and decreased use of medications.
Unfortunately... AFib is under-treated when people are having heart valve and coronary artery bypass graft (CABG) surgery. Reasons for under-treatment include: the Cox-Maze IV procedure adds some complexity to an operation and a lack of physician education / adoption. To help educate cardiac surgeons about the benefits of the Cox-Maze IV procedure, Dr. Gerdisch has trained cardiac surgeons - around the world - on how to perform a successful heart valve and AFib treatment (which is referred to as a "concomitant" procedure).
Dr. Gerdisch acknowledges several cardiac surgeons - Dr. James Cox, Dr. Ralph Damiano and Dr. Niv Ad - for their leadership in developing surgical techniques for successful AFib treatment.
Many Thanks to Dr. Gerdisch & Franciscan Health!!
On behalf of our entire patient community, many thanks to Dr. Gerdisch for sharing his clinical experience and research with our community! Also, many thanks to the Franciscan Health team for taking such great care of heart valve patients.
Related links:
Keep on tickin!
Adam
P.S. For the hearing impaired members of our community, I have provided a written transcript of my video interview with Dr. Gerdisch below.
Written by Adam Pick
Patient & Website Founder

Written by Adam Pick - Patient & Website Founder
Adam Pick is a heart valve patient and author of The Patient's Guide To Heart Valve Surgery. In 2006, Adam founded HeartValveSurgery.com to educate and empower patients. This award-winning website has helped over 10 million people fight heart valve disease. Adam has been featured by the American Heart Association and Medical News Today.
Video Transcript:
Adam Pick: Hi, everybody. It's Adam with heartvalvesurgery.com, and this is a very important surgeon question and answer session all about atrial fibrillation and heart valve disease. I'm thrilled to be joined by Dr. Marc Gerdisch who's the chief of cardiac surgery at Franciscan Health in Indianapolis, Indiana. During his fantastic career, Dr. Gerdisch has performed over 6,000 cardiac procedures of which more than 4,000 involved some form of heart valve repair or heart valve replacement. Dr. Gerdisch, as always, thanks so much for being with us today.
Dr. Gerdisch: Always a pleasure, Adam. Great to see you.
Adam Pick: Yeah, so let's get to this topic of atrial fibrillation, which is one of your specialties there at Franciscan Health in Indianapolis, Indiana. Can we just start to help the patients answer this important question of what is AFib?
Dr. Gerdisch: Atrial fibrillation is an irregular heart rhythm where the atria are firing in a chaotic fashion. I'm always slow to use the word chaotic because there is some organization to the electrical activity that underlies it, but the atria are moving chaotically. The consequence – there's a few. The one that people see the most of, of course, is the risk of stroke. The risk of stroke is related to the lack of normal flow through the atria, normal dynamic flow through the atria. The atria should be doing this. Instead, they're doing this. There is a stasis of flow, and that stasis happens the most in the left atrial appendage, which is a vestige from your embryonic heart. It's actually your left atrium when you're an embryo. People form clot in that appendage, and that clot can break off and go to the brain and cause strokes, so that's why you see all the advertisements for blood thinner.
That's not the only consequence of atrial fibrillation, though, and that's important for people to understand. When people are in atrial fibrillation, their cardiac output goes down. The very earliest studies looking at atrial fibrillation were done in Ireland when they figured out how to cardiovert people, and they looked at the cardiac output before and after and they saw people's cardiac output go up transiently when they got them back into rhythm. The point is that your efficiency is changed when you're in atrial fibrillation. It's diminished by atrial fibrillation.
Adam Pick: I've heard that there is a commonality of AFib with heart valve disease. Is that true, Dr. Gerdisch?
Dr. Gerdisch: That's true, Adam, and it actually is a bi-directional highway. Of course, people with valve disease, we know they have a higher incidence of atrial fibrillation. The reason for that is largely because of the increased pressures in the atria, especially in the left atria for example with mitral valve disease. As the atrium expands, it becomes fibrotic, and as it fibroses, it becomes susceptible to atrial fibrillation. Atrial fibrillation is this irregular heart rhythm when there is substrate change in the muscle. The muscle is electrically active. When it starts to change its substrate, it becomes vulnerable to this chaotic seeming electrical activity in the atria, and once the atrium tips over into it, it's more likely to keep happening, so it's called electrical remodeling, and it goes along with the remodeling of the atrium, so once it happens, it's more likely to happen again and eventually become permanent. We have this effect of the valves causing the increase in pressure in the atria, the enlargement, the fibrosis, and the atrial fibrillation.
The other side of it is that people who have atrial fibrillation – let's say someone has atrial fibrillation already. There are conditions where atrial fibrillation induces changes in the valve, so that's atrial fibrillation induced mitral valve disease, for example, whereas the atrium enlarges as a result of the atrial fibrillation, there are changes in the size of the mitral valve, and that valve starts to leak. That's also true on the other side of the heart, on the right side, where it – and that actually becomes more obvious sooner, usually, because the annulus of the tricuspid valve is a thinner, lighter, less strong structure, so as the right atrium enlarges, the tricuspid valve can be radially tethered as well and leak, so it's in both direction, and they're both important.
Adam Pick: Dr. Gerdisch, if I'm a patient and I've heard about these risks of AFib, I've heard now about how valve disease and AFib can be hand in glove. The big question can AFib be treated during a heart valve surgery?
Dr. Gerdisch: Yes, atrial fibrillation can be treated during heart valve surgery and in fact should be treated. The vast majority of folks going to operating room with valve disease having surgery who have atrial fibrillation should be treated for their atrial fibrillation, and the best treatment for that is going to be a Cox Maze operation. People have to recognize that these are dual pathologies that are related, but the atrial fibrillation generally does not go away just by fixing the valves. It happens sometimes. For example, if someone has had one brief episode of atrial fibrillation, it's true that when they have their mitral valve repair, there's a good chance they won't see that atrial fibrillation again. It's not perfect, but it's a reasonable chance, but everybody else who's had multiple episodes of atrial fibrillation or who has continuous atrial fibrillation, who've had atrial fibrillation on and off for a long time, even if they're not symptomatic, that atrial fibrillation will be back unless somebody addresses is.
Adam Pick: For the patients out there, what are the main benefits that they might experience after a Cox Maze?
Dr. Gerdisch: The benefits of the Cox Maze procedure – there's actually several, but first, it has to be an actual Cox Maze procedure, so it's super important that patients are working with a surgeon that really understands that operation, that knows how to do the entire procedure and do it well. Performed well, it has a very, very good track record of getting rid of atrial fibrillation, and with that then the risk of stroke going down, the cardiac output improving, patient having better aerobic capacity, the risk of other valvular disorders, tricuspid valve insufficiency for example, developing later in life goes down, and if they stay in sinus rhythm and their other risks are low, then they can come off their blood thinners in general, and most importantly to many people is to stop taking antiarrhythmic medications which are fairly toxic. They're great drugs because they do help restore rhythm, but they're fairly toxic medications.
Adam Pick: Dr. Gerdisch, I've been fortunate to actually meet some of your patients who have had a successful Cox Maze valve surgery. Linda Staples comes to mind, how great she's doing after that procedure, but I've heard that sometimes AFib is undertreated during valve surgery. Is that true, and what could be done to help eradicate this problem?
Dr. Gerdisch: It is true that atrial fibrillation is under-treated when people are having heart surgery. There's a few different reasons for it. Some of it is – it does add a little bit of complexity to the operation, so a surgeon may or may not be comfortable with it. It has to be put into the framework of the entire operation for the patient, but the vast majority of the time, if a person goes to the operating room with atrial fibrillation, they're better off being treated with a Cox Maze, and there's plenty data to show that now, so the barriers are related a little bit to education and adoption, which we've been working really hard on for several years to improve the knowledge base for the surgeons in general who are treating atrial fibrillation, and then the other thing is how patients are followed and treated after the operation because it's important after you have a Cox Maze that you are followed, that your rhythm is ensured, that you have the right kind of follow-up. It turns out there's good data to show that people who have good follow-up are more likely to stay in normal rhythm potentially for the rest of their lives, so those components are important, I think, to the success of the operation.
Adam Pick: Dr. Gerdisch. I want to thank you for your leadership. I know all about the trainings you've been doing around the country, around the world for the Cox Maze procedure and helping physicians learn about it, and now taking time out of your busy practice there to educate the patients all about the benefits of having AFib treated during a heart valve surgery, so important. Thank you so much.
Dr. Gerdisch: Thank you, Adam. I would have to say that I have to mention that I have profited from great mentors as well including Jim Cox who originated the operation, Ralph Damiano, Niv Ad, folks that have really invested a great deal of their lifetime in treating atrial fibrillation, and so my success is on the shoulders of giants, but I appreciate it, and it has been a wonderful endeavor for us. Thank you.
Adam Pick: Fantastic. Thanks again, Dr. Gerdisch. Take care.
New Patient Posts
Surgeon Spotlight
Dr. Christopher Heid is a leading cardiac surgeon at UT Southwestern in Dallas, Texas who specializes in heart valve repair and replacement operations.