Stroke Risk Reduction for Heart Valve & Atrial Fibrillation Patients
Written By: Allison DeMajistre, BSN, RN, CCRN
Medical Expert: Dr. Patrick McCarthy, Executive Director of the Bluhm Cardiovascular Institute at Northwestern Medicine
Reviewed By: Adam Pick, Patient Advocate
Published: August 22, 2023
Atrial fibrillation is the most common abnormal heart rhythm diagnosed. The Centers for Disease Control and Prevention estimates that up to 6.1 million people have atrial fibrillation in the United States alone.
Also known as AFib, atrial fibrillation can lead to severe and sometimes fatal complications from blood clots, heart failure and… stroke. According to the American Heart Association, patients with Afib are 5 times more likely to have a stroke. Unfortunately, heart valve disease increases the likelihood that patients will develop atrial fibrillation by 35%. The good news is that both heart valve disease and atrial fibrillation are treatable conditions during one operation, known as a concomitant procedure.
To learn more about atrial fibrillation, heart valve disease, treatment options, and a new clinical trial designed to minimize stroke risk, we met with Dr. Patrick McCarthy at the Mitral Conclave Conference in New York City. Dr. McCarthy is the Executive Director of the Bluhm Cardiovascular Institute at Northwestern Medicine in Chicago and has performed thousands of cardiac surgeries, including more than 5,000 heart valve procedures. In our community, Dr. McCarthy has successfully treated over 175 heart valve patients.
Key Learnings About AFib & Stroke Risk
Here are key insights shared by Dr. McCarthy during our interview:
- Atrial fibrillation is very common in patients with mitral valve disease. “When your valve leaks or if it’s tight, the pressures in the left atrium (the upper heart chambers) are very high. The high pressures cause the chambers to stretch out, and that’s what causes atrial fibrillation,” says Dr. McCarthy. “Instead of beating, the atria are just quivering, which causes blood clots to form, which could cause a stroke.” Patients with these blood clots must go on a blood thinner to help prevent a stroke because the clots formed in the heart from atrial fibrillation are usually large and often fatal or seriously debilitating.
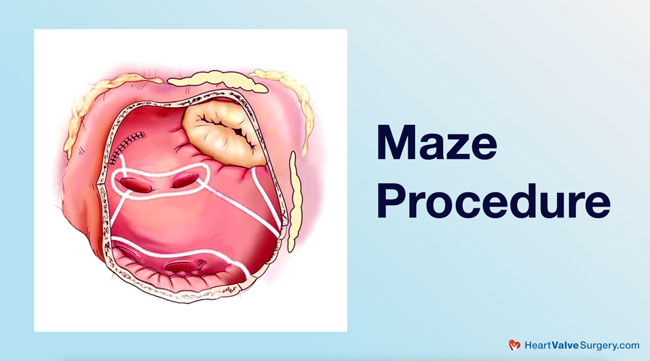
- Only about 60% of patients in the United States, and sometimes less worldwide, receive surgical treatment for atrial fibrillation. However, Dr. McCarthy treats 100% of his patients with atrial fibrillation. “Jim Cox, who invented the Cox-Maze Procedure, works with me at Northwestern. We use this procedure, which is an ablation, to ablate or eliminate the area where atrial fibrillation begins. This reduces the chance that patients will go back into AFib,” says Dr. McCarthy.
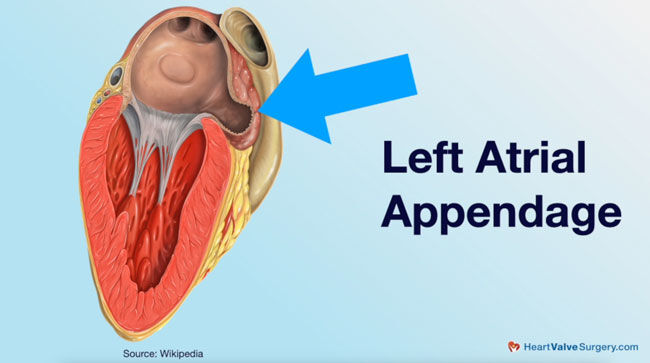
- The left atrial appendage is the most common site for blood clots to form when a patient is in atrial fibrillation. Dr. McCarthy emphasized how important it is to close that area during ablation to reduce the risk of stroke.
- Clinical trials are evaluating therapies that may reduce stroke risk. “A new study called LAAOS III Clinical Trial is about patients that have atrial fibrillation and are going through heart valve surgery, coronary bypass, or any kind of open-heart operation. During the study, patients were followed for a year. They closed the left atrial appendage on half of them and reduced the risk of stroke by 35%. If a patient is listening to this and they have atrial fibrillation and going in for open heart surgery, they should be having a discussion with their doctor about treating it while they’re there,” said Dr. McCarthy.

- Dr. McCarthy believes the key takeaway for patients with atrial fibrillation having surgery to repair or replace a valve is to have them both fixed simultaneously. “What I tell patients is if it’s broken when we’re working under the hood, we’re just going to fix it whatever it is. If they have atrial fibrillation, it doesn’t add much to the surgery these days to treat it, and the data is more evident it has a long-term benefit. It’s the gift that keeps on giving,” Dr. McCarthy said.
Thanks Dr. McCarthy and Northwestern Medicine!
On behalf of our patient community, many thanks to Dr. Patrick McCarthy for sharing his knowledge and expertise about atrial fibrillation, heart valve disease, and the treatment options available to help reduce stroke risk. We also need to thank the Northwestern Medicine team for continuing to take great care of heart valve and atrial fibrillation patients.
Related Links:
Video Transcript:
Adam Pick: Hi, everybody, it’s Adam with heartvalvesurgery.com, and we are at the Mitral Conclave in New York City, and I’m thrilled to be joined by Dr. Patrick McCarthy who is the executive director of the Bloom Cardiovascular Institute at Northwestern Medicine in Chicago. Dr. McCarthy, we’ve known each other for a long time.
Dr. McCarthy: Long time.
Adam Pick: Ten years. You’ve performed thousands of mitral valve operations, which brings you to New York, but it’s not just about mitral valve disease why people are here. There’s related cardiac diseases that may require concomitant procedures, like atrial fibrillation. I feel like it’s almost a state of the union with Dr. McCarthy. What is the connection between AFib and mitral valve disease, and does it get treated often?
Dr. McCarthy: Yeah, so first of all, it’s very common in patients with mitral valve disease. When your valve leaks or if it’s tight, the pressures in the left atrium, the upper chambers, are very high, and it gets stretched out, and that causes atrial fibrillation, so instead of beating, the atria are just quivering, and they form blood clots that could cause a stroke, so patients have to go on a blood thinner, so serious business. If you have a stroke from atrial fib those are much more likely to be fatal because they’re big clots or leave people disabled, so you want to get it treated.
Adam Pick: By treatment, can you explain what you do in the operating room, and getting back to that question, is this something that’s always treated?
Dr. McCarthy: Couple of things. It’s not always treated. With the guy, Jim Cox, that invented the Cox-Maze Procedure – he’s with me at Northwestern now. We treat 100% of patients that have it, so we always treat it, but if you look around the country, it’s more like 60%, maybe even less around the world, so – but we are seeing an increase in adoption that people are doing this more. How do we do it is called the Maze Procedure. It’s an ablation, so we know where atrial fib begins, and then we ablate that area to reduce the chance that patients will go back into atrial fib. A really important part is we close the left atrial appendage where the blood clots form, and that is what reduces the strokes.
Adam Pick: I’ve heard there’s some research going on about the left atrial appendage and maybe a clinical trial. What can you share with the patients about some new research?
Dr. McCarthy: Yeah, a new study came out. It’s called LAAOS III. It is about patients that have atrial fib that are going through heart valve surgery or even coronary bypass, any kind of open-heart operation, they did a big study, followed the patients for a year. Half of them, they closed that left atrial appendage. It reduced the risk of stroke by 35%. It was really effective at reducing the risk for a stroke. If a patient is listening and they have atrial fib and they’re going in for open heart surgery, they should be having this discussion with their doctor about treating it while they’re there.
Adam Pick: For the patients, would you say that’s the big takeaway is to fix it all?
Dr. McCarthy: Yes. What I tell patients is that if it’s broken when we’re working under the hood, we’re just going to fix it whatever it is. If they have atrial fib, it really doesn’t add that much to the surgery these days to treat it, and the data is more and more evident that it has a long-term benefit. It is the gift that keeps on giving.
Adam Pick: Dr. McCarthy, you have fixed a lot of patients from the heartvalvesurgery.com community, many patients watching, and I just want to thank you and your team at Northwestern Medicine in Chicago. Thanks so much for being here.
Dr. McCarthy: Thanks, Adam. Great to see you again.






