Bacterial Endocarditis: What Should Heart Valve Patients Know?
Written By: Adam Pick, Patient Advocate, Author & Website Founder
Page Last Updated: February 15, 2026
If you – or a loved one – were diagnosed with bacterial endocarditis, I imagine you have questions about this rare, but potentially life-threatening infection. You will likely want to know, “How is it caused?”, “What are the symptoms?”, “How do you prevent it?” and “How is it treated?”
What Is Bacterial Endocarditis?
Bacterial endocarditis (BE), (also known as infective endocarditis), is an infection in the endocardium, which is the inner lining of your heart chambers and heart valves. You might be interested to know that the word endocarditis comes from (“endo” meaning inner, “cardio” meaning heart, and “itis” meaning inflammation of an organ).
If you have BE, your heart valves may not be able to work properly. Cedars-Sinai notes that this can force your heart to work harder to get blood out to the body. Over time, the heart can become enlarged (dilated) due to the ongoing strain on the cardiac muscle. According to the Mayo Clinic, if endocarditis is not treated quickly, it can damage or destroy your heart valves and can lead to life-threatening complications.
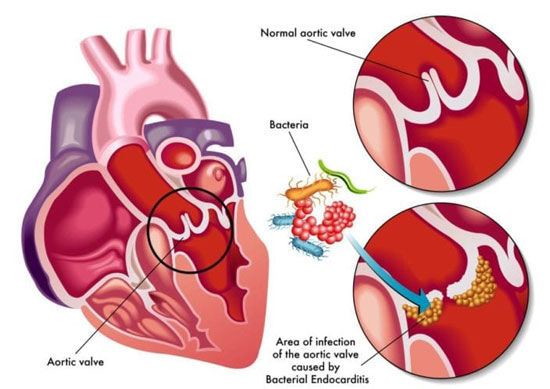
How Is It Caused?
As noted by the American Heart Association, bacterial endocarditis generally occurs when bacteria or other germs from another part of your body spread through your bloodstream and settle in the heart lining, a heart valve or a blood vessel. BE also affects the valves and often affects the muscles of the heart causing inflammation of the heart lining, heart muscles, and heart valves.
According to Medical News Today, the infection is normally caused by streptococcal or staphylococcal bacteria. Rarely, it can be caused by fungi or other infectious micro-organisms.
So, you might ask, how does this bacteria get into your bloodstream? It is usually from an infection through normal activity such as tooth-brushing that ends up causing minor injury to the lining of your mouth or your gums.
Normally, our immune systems can destroy these unwanted micro-organisms, but if you have any damage to your heart valves, it can make you more prone to having the bacteria get to the heart and attack the heart tissue.
You may be thinking, “Is everyone at risk of getting bacterial endocarditis?” Potentially. But there are certain factors such as heart health and risky behaviors that make some people more susceptible to getting BE. These factors are detailed in the “Who is at Risk?” section below, so keep reading. Besides brushing your teeth, or other dental procedures that results in an infection, other surgical procedures such a colonoscopy or a procedure that affects your windpipe or urinary tract can spread the bacteria.
Injecting drugs with unclean needles can cause BE and any surgical or medical tools used in treatment, such as a urinary catheter or long-term intravenous medication can increase the risk of contracting endocarditis.
Who Is At Risk?
According to the Mayo Clinic, if your heart is healthy, you are less likely to develop BE, although it is still possible. Bacteria that causes infection tends to stick to and multiply on damaged or surgically replaced heart valves, or on heart lining that has a rough surface.
According to the American Heart Association, those most at risk include anyone with birth defects of the heart such as malformed valves or a hole in the septum. Risk factors for adults include an abnormal heart. The Mayo Clinic also notes that germs are more likely to attach to an artificial heart valve than to a normal heart valve.
As you might guess from the “How is it Caused” section above, if you have not-so-good dental health or you bleeds when brushing your teeth, you have a higher risk of developing bacteria in the blood. Additionally, if you’ve had an artificial heart valve replacement, and you need to go to the dentist, Family Doctor suggests you may want to take an antibiotic first before a cleaning or a cavity filling to prevent getting BE. It can help keep bacteria from getting into your bloodstream.
Risky activities can also place a person at risk. A history of intravenous (IV) drug use can cause BE as the needles may be contaminated with the bacteria. Sexually transmitted diseases such as chlamydia or gonorrhea make it easier for bacteria to enter the bloodstream and get to the heart. So certain life choices can mitigate your risk.
Is Bacterial Endocarditis Common?
According to the American Heart Association, endocarditis affects about 3 to 7 people out of 100,000.
Medical News Today reports that BE is twice as common in men as in women. In the United States, over 25 percent of cases affect people aged 60 years or above.
Cedars-Sinai’s research suggests that BE is very rare in people with normal hearts who have no other risk factors. It is much more common in people with certain heart conditions or other risk factors detailed in the “Who is at Risk” section.
What Are The Symptoms?
Bacterial endocarditis may develop slowly or suddenly, depending on what germs are causing the infection and whether you have any underlying heart problems. While BE symptoms can vary, the Mayo Clinic lists common ones as:
- Flu-like symptoms, such as fever or chills
- A new or different heart murmur
- Fatigue
- Aching joints and muscles
- Night sweats
- Chest pain when you breathe
- Swelling in your feet, legs or abdomen
And, in addition to those, Cedars-Sinai includes others such as:
- Trouble breathing with exertion
- Shortness of breath while lying down
- Cough
- Nausea or Vomiting
- Headaches
- Blood in the urine
- Swelling of the feet, legs, or abdomen
How Is It Diagnosed?
Your doctor may suspect you have BE based on your symptoms and health history. Cedars-Sinai notes that tests such as the following may also be needed:
- Echocardiogram (uses ultrasound to view the valves and blood flow through your heart)
- Transesophageal echocardiogram (detailed view of the heart from the esophagus)]
- Blood tests (checks for bacteria and signs of inflammation)
- Electrocardiography (ECG) (analyzes your heart rhythm)
- Chest x-ray (examines your lungs)
Other tests include a Cardiac CT, if more information is needed about your heart, and urine tests to check for kidney damage.
What Are The Risks And Complications?
Bacterial endocarditis causes clumps of bacteria and cell fragments to form in your heart and on the heart valves.
These clumps, called vegetations, can break loose into the bloodstream and travel to your brain, lungs, abdominal organs, kidneys or limbs. They can cause damage by blocking other blood vessels and even spread the infection to other organs.
According to the Mayo Clinic, endocarditis can cause several major complications, including:
- Heart problems, such as heart murmur, heart valve damage and heart failure
- Loss of the ability to move part of all of your body (paralysis)
- Pockets of collected pus (abscesses) that develop in the heart, brain, lungs and other organs
- Stroke
- Seizures
- Pulmonary embolism – an infected vegetation that travels to the lungs and blocks a lung artery
- Pneumonia
- Kidney damage
- Enlarged spleen
Can Endocarditis Kill You?
According to Family Doctor, a possible side effect of BE is heart failure. The Mayo Clinic states that BE is a serious condition, and if it isn’t treated right away, it can lead to death.
Acute bacterial endocarditis can happen quickly and can get worse fast. If left untreated, it can be life threatening. Symptoms of acute BE usually begin with fever (102°–104°F), chills, fast heart rate, fatigue, night sweats, aching joints and muscles, persistent cough or swelling in the feet, legs or abdomen.
If you develop symptoms of BE, see your doctor as soon as possible – especially if you have risk factors for this serious infection, such as a heart defect.
How Do You Prevent It?
The Mayo Clinic states that knowing the signs and symptoms such as a fever that won’t go away, unexplained fatigue, any type of skin infection, or open cuts or sores that don't heal properly should be a red flag.
Good dental health and hygiene helps prevent heart infection – brush and floss your teeth and gums regularly, and have regular dental checkups. If you're at risk of BE – such as if you have a prosthetic heart valve, congenital heart disease, or a history of endocarditis – let your dentist know to see if you need antibiotics before any dental procedures.
Avoid procedures that may lead to skin infections, such as body piercings or tattoos, and don’t use IV drugs.
What Is The Treatment?
Most patients with bacterial endocarditis receive antibiotics, and according to the American Heart Association, treatment of BE usually consists of two to six weeks of antibiotics given intravenously, so the patient will need to stay in the hospital. Regular blood tests will monitor the effectiveness of the medication.
The type of antibiotic depends on several factors. These include the type of bacteria, and if you have an artificial valve. Medical News Today notes that the most commonly used antibiotics are penicillin and gentamycin. Patients can usually go home when symptoms have subsided, but most will continue to take antibiotics after they return home.
After that, you may be able to have IV antibiotics at home, and later in your treatment, you may be able to take oral antibiotics. Severe cases of BE, or if BE has damaged the heart, surgery may be necessary. If the damage to your valves is severe, you may need heart valve surgery. Or you might need surgery to help clear the endocarditis. Surgery may repair a heart defect or damaged heart valves, replace them with artificial ones, or drain the abscesses that have developed within the heart muscle.
You Might Also Like
To help you learn more about your heart, bacterial endocarditis and surgical treatment, you may like:
- Endocarditis: Top 7 Facts Patients Shoud Know
- Rheumatic Fever & Heart Valve Disease: 8 Important Facts
- What is a Heart Murmur?
- Enlarged Hearts: What Should Patients Know?
- Explore the Heart Valve Learning Center
References:
Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/endocarditis/symptoms-causes/syc-20352576
Cedars-Sinai Medical Center: https://www.cedars-sinai.org/health-library/diseases-and-conditions/b/bacterial-endocarditis-adult.html
American Heart Association: https://www.heart.org/en/health-topics/heart-valve-problems-and-disease/heart-valve-problems-and-causes/heart-valves-and-infective-endocarditis
Medical News Today: https://www.medicalnewstoday.com/articles/151016.php
Family Doctor: https://familydoctor.org/condition/bacterial-endocarditis/
American Heart Association Journals: https://www.ahajournals.org/doi/pdf/10.1161/CIR.0000000000000296
MSD Manuals: https://www.msdmanuals.com/en-gb/home/heart-and-blood-vessel-disorders/endocarditis/infective-endocarditis