Heart Surgery Innovation: New Approach to Pain Management
Written By: Adam Pick, Patient Advocate & Author
Medical Expert: Dr. Marc Gerdisch, Chief of Cardiac Surgery at Franciscan Health
Published: September 22, 2021
One of the important questions patients have prior to heart surgery is, “How painful is it?”
The great news for patients is that many surgeons and medical companies have developed new innovations, techniques and devices to reduce and/or eliminate pain.
To learn about pain management after heart surgery, we interviewed Dr. Marc Gerdisch, the Chief of Cardiac Surgery at Franciscan Health in Indianapolis, Indiana. During his 25+ year career, Dr. Gerdisch has performed over 6,000 cardiac procedures and more than 4,000 heart valve operations. At HeartValveSurgery.com, Dr. Gerdisch has successfully treated over 100 patients.
Key Learnings About Pain Management
The key learnings that Dr. Gerdisch shared during our interview are actionable and could be very helpful for patients who may want to discuss these innovations with their medical teams.
- Dr. Gerdisch and his team have developed a unique “Enhanced Recovery After Cardiac Surgery Program” that takes a holistic approach to pain management. The program includes recovery considerations including nutrition, breathing techniques, and stretching to diminish patient discomfort and immobility following heart surgery.
- Today, most of Dr. Gerdisch’s procedures use a minimally-invasive approach to heart valve repair and heart valve replacement. Smaller incisions often result in less pain for the patient, shorter stays in the hospital, and enhanced recovery. However, Dr. Gerdisch may use a traditional sternotomy (chest incision) for complex cases (e.g. multiple valve) and re-operations.
- Given concerns related to the “Opioid Crisis”, Dr. Gerdisch developed patient recovery protocols to minimize patient use of opioids in the hospital and after discharge. Dr. Gerdisch states, “There’s been a very strong push nationally to get away from the use of opioids. We’ve never liked using opioids because not only are they addicting, but they cause constipation, obstipation, and foggy head.”

- Nerve blocks (cryoanalgesia) and rigid sternal fixation are two innovations that Dr. Gerdisch use to reduce patient pain. As a result, Dr. Gerdisch has decreased the use of opioids by 87% for sternotomy patients. Today, only 10% of Dr. Gerdisch’s sternotomy patients are discharged with an opioid prescription. And, 0% of Dr. Gerdisch’s minimally-invasive patients are discharged with an opioid prescription.
 Nerve block (Cryoanalgesia)
Nerve block (Cryoanalgesia)
- Rigid Sternal Fixation is “changing the game” specific to pain management during patient recovery after heart surgery. Dr. Gerdisch states, “People who have rigid sternal fixation are much more comfortable and we can let them use their arms. The day after surgery, patients can lift 15 pounds. Patients can lift 20 pounds when they leave. Patients go home and are able to get in-and-out of their chair, and in and out of their – whatever they need to do.”
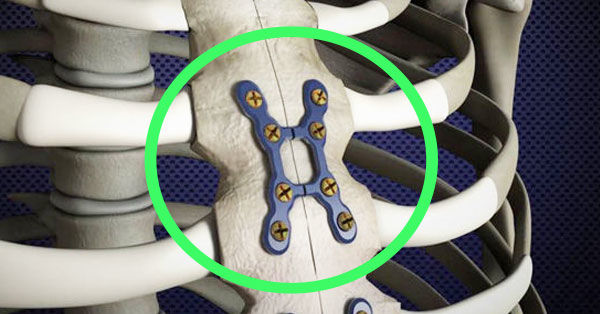 Rigid Sternal Fixation (SternaLock Blu)
Rigid Sternal Fixation (SternaLock Blu)
- Frail patients are also benefitting from the Enhanced Recovery After Cardiac Surgery Program. According to Dr. Gerdisch, “Where 30% of frail patients used to go to some type of extended care facility after discharge… Now, now only 10% need to go.”
- Unfortunately, about 20% of patients who have a traditional sternotomy experience some form of long-term consequence – pain, instability, poor healing. Using these new innovations, the chest and the ribs are stabilized immediately. Specific to this new approach to pain management, “Patients are golfing, bowling, and hitting fast pitch in a few to several weeks. We are changing the recovery process entirely.”
Here is an insightful video of Dr. Gerdisch’s patients just a few days and/or weeks after heart surgery. As you will see and hear, these patients are not experiencing pain.
This Just In! No Pain or Opioids for Layman Boyd!
Now, here’s an amazing coincidence…
As I am posting this story, I just received a video from Dr. Gerdisch about Layman Boyd’s experience with pain after a major cardiac procedure. Layman, 57, had a minimally-invasive mitral valve repair surgery performed by Dr. Gerdisch yesterday.
You will see and hear that – just one day after heart surgery – Layman’s early recovery has been pain-free. It should also be noted that Layman is not taking any opioids. Amazing!!!
Many Thanks to Dr. Gerdisch & Franciscan Health!!
On behalf of our entire patient community, many thanks to Dr. Gerdisch for sharing his clinical experience and research with our community! Also, many thanks to the Franciscan Health team for taking such great care of heart valve patients.
Related links:
- See 120 Patient Reviews for Dr. Gerdisch
- Cryoanalgesia & Heart Surgery Pain: What Should Patients Know?
- Top 5 Facts About Dr. Gerdisch’s Rapid Recovery Protocol
- What Is Rigid Sternal Fixation?
Keep on tickin!
Adam
P.S. For the hearing impaired members of our patient community, I have provided a written transcript of this video below.
Video Transcript:
Adam Pick: Hi, everybody. It’s Adam with heartvalvesurgery.com, and this is a very important surgeon question-and-answer session all about pain management after heart valve surgery. I’m thrilled to be joined by Dr. Marc Gerdisch, who is the chief of cardiac surgery at Franciscan Health in Indianapolis, Indiana. During his fantastic career, Dr. Gerdisch has performed over 6,000 cardiac procedures of which more than 4,000 involved some form of heart valve repair or heart valve replacement.
Dr. Gerdisch, I am really excited about this conversation because one thing I know as a patient and talking with thousands of patients over the years is that pain and the concern of pain after a heart valve surgery is front and center to most patients’ mind. I understand that you are doing some fascinating things there at Franciscan Health in Indianapolis, Indiana, specific to pain management. Can you talk about that?
Dr. Marc Gerdisch: We have really focused on pain management. It’s been a journey over several years actually and part of our entire Enhanced Recovery After Cardiac Surgery program, where we address everything from nutrition to breathing techniques, and part of that for us was how do we take the barrier of discomfort and immobility out of heart surgery?
When you think about it, the difference between something that’s done up with a catheter versus having open heart surgery is the incision, so – and the incision, most people aren’t that concerned about the length of the incision or whatever. In fact, as you know, most of our valve operations we do through a small incision between the ribs, but when we have to do a re-operation, when we have to do multiple valves, when you have to do really big operations, we have to do that through a sternotomy. We went at this as a topic of absolute necessity that we would change the experience post-operatively for people.
This dovetails into – as you know there’s been a very strong push nationally to get away from the use of opioids. We’ve never liked using opioids because not only are they addicting, but they cause constipation, obstipation, foggy head. We have actually made incredible progress in this. Using our techniques for minimally invasive with nerve block, for sternotomy with what we call erector spinal blocks and rigid sternal fixation, we have driven our use of opioids down 87% for inpatient use for sternotomy patients, 87%, and only 10% of those patients go home with an opioid prescription, and with minimally invasive, it is zero. We don’t use opioids for them. They don’t have them at discharge, so we have completely changed the game. Not only does it mean they’re not getting the opioids, it means that they’re more comfortable, because the drive to decrease opioids, the premise should really be how do we get rid of the pain? How do we get rid of the problem?
In addition to that, mobility has dramatically improved, so people who have rigid fixation of their sternum not only are much more comfortable, but we can let them use their arms. The day after surgery, they can lift 15 pounds. They can lift 20 pounds when they leave. People go home and are able to get in and out of their chair, and in and out of their – whatever they need to do. Now, a downstream consequence of that was for the frailer patients who might otherwise go to an extended care facility. We cut that by two-thirds. Where 30% of patients used to go to some type of extended care facility, now only 10% go. Even our frailer patients, the folks who really want to be home, but they have to go to an extended care facility, they go home.
All of those things come together, and really at the center of it was pain management. How do we make the pain go away? As a consequence, how do we improve mobility and give people back their lives faster, and as a consequence, all of the great psychological impacts that go along with just going back to your life? We’ve been super enthusiastic about it. We have so enjoyed it, and our patients have enjoyed it.
Adam Pick: Dr. Gerdisch, it almost sounds unbelievable, the results that you’re getting there. Can you talk about the results that your patients are seeing because of this new approach to pain management?
Dr. Marc Gerdisch: It does seem unbelievable. Sometimes I can’t believe it, but patients show me all the time. What they get out of it is they get their lives back. It’s really important that we understand not only on the short end but on the long end. When people have a sternotomy, about 20% of people have some long-term consequence. It might be pain, instability, something related to that, so what we do is an orthopedic repair of the bone to ensure that it fully heals. In doing so, the bone is completely stabilized from day one, which means they can use their arms and go back to their full activities, and so patients are golfing, bowling, hitting fast pitch in a few to several weeks. It has changed the recovery process entirely.
Adam Pick: Dr. Gerdisch, I cannot thank you enough for your dedication to thinking about this from the patient’s perspective, in particular to pain management. I can tell you, as a patient, that was not the fun part of heart surgery, so thanks for getting your patients back on their feet in the short term and the long term. This goes out to your entire team there at Franciscan Health in Indianapolis, Indiana. Thank you so much.
Dr. Marc Gerdisch: Thank you, Adam, and you’re right. It is a team. We have everybody involved, physical therapy, respiratory therapy, the nursing staff. They all understand this early mobilization and getting people out and back to their lives. Thanks for having me.





