Guest Blog: 25 Tips To Prepare Women For Heart Surgery
By Adam Pick on March 27, 2014
Every so often, I receive a patient email that makes me think, “Holy Moly! I need to share this with our community!”
The email below from Christine Wagner triggered that exact reaction. So, for that reason, I am featuring Christine’s story as a special “Guest Blog” because I believe her patient tips are going to help so many patients in our community — especially the women!
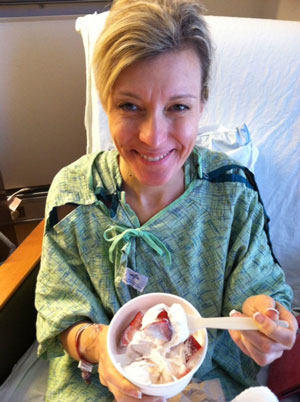
Christine’s Story
My name is Christine Rekash Wagner and I am 42 weeks post-op from a mitral valve repair performed by Dr. Patrick McCarthy and his surgical team on June 13, 2013 at Northwestern Memorial Hospital in Chicago. I have been a patient of Dr. Robert Bonow since March 2, 2006 with a mitral heart valve disorder. After several years of yearly echocardiograms and a watchful eye, in October of 2009, I was diagnosed with a leaky mitral valve. Most recently, in October of 2012, I was advised that the results of my yearly echo demonstrated that my mitral valve regurgitation was becoming severe enough that I should consider surgery while I was a young and healthy 41 year old female.
The irony of the situation is that externally I wasn’t feeling anything but what I had grown accustomed to as part of my daily living – heart palpitations and fatigue which I attributed to the overall stresses of everyday life. However, internally, I began to exhibit signs on my echocardiogram that my left ventricle was becoming dilated as result of the heart working harder to pump the blood that was regurgitating backward, thus not pumping efficiently throughout my body.
While I struggled with the concept of having surgery at such an early age, especially being in optimal health, I was advised that a repair to the valve is more advantageous than a replacement. As a female contemplating if pregnancy would ever be an option with this disease, I was advised several years early on that child bearing would be very high risk and I would need to be closely monitored by a team of cardiologists both during pregnancy and in delivery. The most difficult pill to digest was the fact that my disease would only get worse as time progressed. The heart would become weaker and the ventricle would continue to enlarge, pressure in the lungs continue to increase, chordae become weaker, possibly rupture and cause irreversible damage overall. I continuously struggled with the thought that while I maintained a healthy weight of 125 lbs, over all healthy diet, moderate exercise and no matter how many antioxidant glasses of wine I consumed, genetics simply ruled this disease.
Operation “Backward Blood” Begins…
With all of this being said, on January 16, 2013 my husband and I met with Dr. Patrick McCarthy. After many questions and answers, hesitations, fears of the unknown and all the “what if’s“, I scheduled the surgery for June 13, 2013. I chose to have the traditional open heart sternotomy incision even though I was an optimal candidate for the robotic minimally invasive procedure. I was not overly concerned about the cosmetic appearance of the scar post surgery as much as I wanted to minimize any risk during the minimally invasive procedure. In my opinion, sometimes the old fashioned ways are the best ways. Open heart surgery has become so advanced that I was comfortable with the traditional sternotomy being in the hands of world renown surgeons and cardiologists at Northwestern.
Operation “Backward Blood” was the moniker that I chose to refer to my surgery. In preparation for Operation Backward Blood, my surgical team recommended I read Adam’s book, The Patients Guide to Heart Valve Surgery for patients and caregivers to dispel my anxiety, uncertainty and fears of what I was about to encounter. Looking back, I can truly say that the anxiety of the surgery was the most stressful for me and I would have been even more anxiety ridden without having read his book and his experiences, as well as the input from Doctors across the country. With this in mind, I would like to share with you some tips and tricks for my preparation of “Operation Backward Blood” pre-op, post – op and recovery from a female’s perspective.
If you are fortunate as I was to have some time to schedule the surgery, you will also be fortunate to organize and delegate work assignments, household chores and shopping lists. While I do not recommend scheduling 6 months in advance as I did, as anxiety levels just intensify, I found that it was extremely helpful to make notes and deadlines for myself as the operation date drew closer. I also applied this tactic to my job. I took copious notes of where I left off before enacting FMLA re: my workload as a paralegal and I found this extremely helpful when returning to work. Additionally, I began to keep track of common items, as well as favorites that I would purchase at the grocery store so that my husband or caregivers would be able to streamline their trips to the grocery store. I even made meals ahead of time and froze them for when I would return home, with the intention to making of cooking a little easier for my husband and caregivers. There’s nothing quite like homemade chicken soup to help you feel better instantly. I am very fortunate that I have a very close knit family and had fresh homemade ” meals on wheels” delivered to me by my parents and sisters post – op.
Lastly, I scheduled a few days off prior to surgery to clean my house from top to bottom one last time, a final trip to the grocery store, pay bills, organize my legal documents needed for the hospital, prepare for my recovery, pack for the hospital and enjoy time with my family and friends.
Make Pre-Op Lists & Check Them Twice!
In terms of packing, listed below are a few items that I found to be tremendously helpful and comforting while recuperating in the hospital. While it is true that “There’s No Place Like Home”, and at times all you will want to do is click your red high heels together, unfortunately the reality is that you will be hospitalized for a short time. I was hospitalized for seven days due to some complications with fluid around my heart, lungs and low blood pressure. These items will help you feel somewhat at home while you recover in the hospital.
- Your own pillow. Hospital pillows are the most uncomfortable ever. All the nurses commented that it was smart of me to bring my own pillow as I was able to use it to prop up to a more comfortable position. At night it came in handy to put alongside while trying to reach a comfortable sleeping position. Even though the hospital beds recline, they only recline to a point. Pillows can double as that extra comfort level that the reclined bed position cannot provide.
- Dry Shampoo. After days of not being able to wash your hair, this was a life saver! While I was unable to shower until my 5th day, I at least felt somewhat put together with the ability to spray my hair clean. I used GLO Essentials RE-Energizing provided to me by hair stylist. If you cannot find a dry shampoo that you like, baby powder also does the trick to absorb the excess oil.
- IPAD or other device with some form relaxation or nature sounds music. This helped drown out the continuous beeping sounds of the heart monitor, nurses station and general traffic. This was also especially helpful at night when going to bed.
- Tampons and/or pads. Regardless of whether or not you are able to plan your surgery around your menstrual cycle, if you are of menstruating age, you WILL get your period post – op. Five days after surgery I thought that perhaps my chest tube ruptured or something else was hemorrhaging. I certainly did not think it was my period since I just had it a week before surgery. Sure enough when a nurse confirmed that it was my period, I wanted to cry. As if going through open heart surgery wasn’t enough. She advised me stress can and does cause amazing things to our body and any major surgery is one of those stresses.
- Desitin cream for any burns or reactions to the leads from EKG and heart monitors. I have very sensitive skin and broke out in blisters from the gel adhesive in theses patches. Cortisone or Benadryl cream did not work for me. My brother in law paramedic firefighter recommended that it is the zinc oxide compound that helped me gain relief. A bit of caution, this can stain and ruin your undergarments and is difficult to remove from your hands, but it worked wonders for me! As always, check with your doctor or nurse first before using.
- Boxer shorts . Hospital gowns are notoriously uncomfortable and one size fits none. As a result do not expect too much privacy in terms of covering up your assets. I did find that boxer shorts provided me with enough coverage for when I was walking around the hospital on my daily rounds. Additionally, I also had to have Lovenox shots in my abdomen. Boxer shorts did not feel constricting around the area of my shots especially when your chest tube drains and wires from the heart monitors will also be near.
- V-Neck Nightgown. While you will be in a hospital gown the entire length of your stay, you will eventually leave it behind when you go home. I packed a regular v neck nightgown that doubled as a dress for when I was discharged. The v neck is helpful in that it will not irritate your surgical site. I threw a scarf around my neck and slipped on flip flops. For me, I was retaining some water and my feet were very swollen. Pack a shoe that will easily slip on, even if they are house slippers with a sole. You may not be able to fully bend down to tie your laces on your shoes right away.
Some items you may want to consider orchestrating or inquiries made before you head into surgery:
- Nails. If you have acrylic or gel nails, consult your surgical liaison as to whether or not the surgical team prefers at least one nail free from gel or acrylic for an accurate read of the pulse ox meter. The same holds true for a pedicure and if you should arrive without polish on both your feet and hands.
- Bed Wedge for recovering at home. I found that I alternated between sleeping in a recliner my first week to using the bed wedge while in bed. You will find at first, that getting in and out of bed will be very difficult, yet alone trying to lay flat or propped up carefully with pillows. The bed wedge is available in various inclinations and provides a sturdy surface by which you can remain propped up without sinking into your pillows. I found my bed wedge during post – op recovery at a local medical supply store. It was not until I was recovering post -op, having my first cardio version, with many sleepless nights under my head, that I discovered this through the kind mercy of a cardiac nurse.
- Shower chair. I did not anticipate having any post – op issues, low blood pressure being one of them. As a result, I could not stand in the shower for the entire duration, especially when washing my hair without getting dizzy. The shower chair allowed me the comfortability and stability needed to confidently shower. This item can also be found in a medical supply store, or you may inquire from the hospital occupational therapist or discharge planner who will visit you during your post – op recovery.
- A watch that measures your heart rate and walking distance for when you begin your journey recovering at home with daily walks and increased activity. It is also helpful in cardiac rehabilitation in terms of monitoring your heart rate even though you are hooked up to a telemetry monitor.
- Color treated hair. If you have color treated hair, you may want to schedule your final color 4 weeks before surgery. Keep in mind that the anesthesia and medications post – op may affect the pigmentation of your hair, not to mention the overall processing of your hair color in terms of whether it will take longer or faster. Also beware that during recovery your skin and hair could become dry and brittle. You may even experience some hair loss and this is normal over time as the anesthesia works its way out of your system. Before your surgery, talk to your stylist to see what he or she recommends in terms of specifics. There’s nothing more disappointing than going through major surgery, wanting to feel good about your self-image only to find that your hair color is not quite how it’s suppose to be post – surgery.
- Undergarments. I found it extremely comfortable to wear a tank top with a built in shelf bra while I recovered at home. Initially, I needed some assistance while heeding my sternal precautions, but I found that this was something that I could easily transition into from day to night while minimizing my overhead movements. In a few weeks I was able to maneuver a sports bra that hooked in the front. Shop for these items prior to your surgery.
- Distribution List. Many friends and family will no doubt want to monitor your progress. From the caregiver’s perspective your open heart surgery will be just as stressful on them. I was blessed to have my husband, parents and sisters in the recovery room waiting for me. Every minute that passes while you are in surgery is agonizing for them. Designate one person to send an email or text update to your distribution list to update your loved ones on your progress. This will also come in handy once you have been moved to the cardiac unit to keep in touch with them.
- A journal or notebook. This will be very useful when doctors, nurses, occupational therapists, discharge planners and medical staff come to visit you while in the hospital. I found this very helpful in monitoring my vitals, medications and taking notes on my progress. For me, I lost all concept of a time frame and found that by writing things down, I could easily communicate with doctors and nurses how I was feeling each day. Expect that each day you recover will be a new feeling, whether positive or negative. I also found this tremendously helpful when I recovered at home, as I would always take my black book with me to each follow up doctor visit and have all my information at my fingertips when discussing my progress. (See Heart Valve Journals.)
Post-Op Recovery In Your Room
If there is one tip that I can provide, it is that your nurses will be your angels with hidden wings. They truly are the heartbeat of healthcare. If you are able ahead of time, coordinate a basket of candy for your caregivers to bring when they come to visit you in the hospital. A small token of appreciation will go a long way when you push the nurse call light at 2:00 am.
While my post – op recovery in my room was filled with daily x-rays, a lung tap to drain fluid, endless blood tests, echocardiograms to measure the fluid retention around my heart, and a never ending cocktail of meds, I somehow managed to keep a positive outlook. While it’s hard to stay positive and motivated while in pain, the entire experience is a life altering escapade. Feelings of being scared, lonely, nerve wrecking, heart breaking and an overall drawn out experience emotionally and physically to say the least permeate your thoughts. Then you realized you survived it all and you smile! You think to yourself, It can’t get much worse than open heart surgery and now that you survived this, you’re ready for anything that lies ahead.
I found that establishing a routine in the morning, helped me prepare for my day. I would wash my face, brush my teeth, spray my hair with shampoo and transfer to the chair to await my breakfast. I would keep current with my spirometer exercises and I would try my best to walk. The key is to keep moving as permitted by your nurses. While you will not be able to walk a block, celebrate your small victories one heartbeat at a time. You may only be able to walk to and from the door at first. As you become stronger each day you will be able to walk farther and farther. Try to stay positive. You WILL get there with each step of the way. If your diet permits, find something that you enjoy and celebrate your small victories. Remember when you were a child and ice-cream seemed to take away all the pain? For me it was fresh strawberries and vanilla ice-cream.
On June 21, 2013 I was finally discharged! I traded in my hospital gown for my clothes, turned in my id bracelet for some bangle bracelets, said my goodbyes to nurses and other patients, threw on my shades and was ready to “roll”.

Post-Op Recovery At Home
Looking back at my overall recovery, the one tip that I can provide is to be patient with yourself. It sounds so much easier said than done. I consider myself to be a type “A” personality and became very easily frustrated when it took me so much longer to complete tasks. I would become very angry and bitter that I was not able to do things as quickly as I used to pre-surgery. I felt helpless like a toddler. Accept the help when it is given. This is where having notes and lists for your spouse or caregivers became really handy. Expect that you will not be able to do things on your own right away. Remember that while you are physically recovering, your spouse and caregivers are going through this with you. Be patient with them. It may feel like you are learning how to walk all over again because essentially you are. But remember, put one foot in front of the other and eventually you will get there.

AND don’t forget to celebrate the small victories!! An example of this feeling for me was the first time post – op that I had the ability to make myself an omelet for breakfast. I became very upset that it took me ten minutes to make, but the fact is, I made it myself and was making progress! I also wanted to start vacuuming my second week that I was home. I highly recommend NOT doing this as it will go against your sternal precautions, however, with time, I was able to get back into the cleaning mode. Below are a few tips that I found helpful, overall with my post – op recovery at home.
- Establish a routine . Even though you may find yourself at home recovering, it is important that you establish a daily routine. For me it was getting up each morning and having breakfast, showering and getting dressed for the day. Whether or not I went anywhere during the day didn’t really matter. Overall, I felt a sense of accomplishment by getting up each morning and getting my day underway, even if it meant that I would only be walking to the end of the driveway and back.
- Washing and drying your hair. While I had my operation during the summer, I was fortunate that I did not have to dry my hair all the time. I previously mentioned that your skin and hair could become brittle and dry as a result of the anesthesia. I found that it was helpful for me to not wash my hair everyday because I did lose some hair during my initial recovery. While it did not come out in “clumps” it was a noticeable amount when I would brush my hair after shampooing. I did find the shower chair very helpful in the sense that when I was ready to wash my hair, I would do so sitting down. I also found that washing my hair forward instead of backward was much more comfortable. You will have sternal precautions to adhere to and this method worked best for me. That being said, expect that you may need some assistance at first drying your hair. For me, my hairdryer is on the heavier side. The inability to raise my hands at first presented a small hurdle in drying my hair. This is where my sisters and I reminisced about playing “beauty shop” when we were younger as they assisted me with drying my hair. I certainly didn’t even entertain the idea that a simple task of blow drying your hair would be a bit of a challenge after surgery.
- Change up the scenery. Daily walking will be your ticket to freedom. While you may not be motivated to get up and move, you will find that the more you move, the more you feel a sense of accomplishment in your overall recovery. At first you will only be able to walk in small increments but as you become stronger and stronger each day, you will be able to walk farther and farther. For me, I became bored with walking around my neighborhood. My father came up with a great idea and I pass this on to you. He suggested taking my daily walking to a nearby park or the local zoo. While I was still not able to drive, I thought this was a great idea as it mixed up the scenery a bit. It provided me with some variety in my recovery. The first time out of my house and back into the hustle and bustle of everyday life with other people, I suddenly felt so small and the world seemed so big. How could this be when I felt like I was making so much progress around my neighborhood? Well I thought about it for a bit and that’s when it hit me. I discovered a whole new outlook in terms of my recovery. Our family trip to the zoo was a milestone achievement. Mentally, I felt a sense of accomplishment as I was able to walk the entire east side of the zoo and realize how much progress I made. Physically, I did so in about three hours without being winded. That being said, I quickly began to enlist the chauffeur services of my husband and family and began to tag along with them to small trips to the grocery store and the mall. A whole new world opened up to me! Thanks Dad
- One side note: keep your scar covered when out in the sun and adhere to prescription warnings regarding sun exposure.
- Wheelchair access. If you have the opportunity to take advantage of access to a wheelchair I highly recommend doing so. While I was not always seated in the wheel chair on my outings, there were times in the early stages of my recovery where I would be walking in a store and become lightheaded because I battled low blood pressure. The wheelchair came in handy as I would have a safe place to immediately sit to regain my balance. The upswing to this is that since most public facilities have wheel chair access, you are not limited in terms of your destination. Lastly, by pushing the wheelchair yourself while walking, you are building your endurance level.
- Post-op pedicures and manicures. If you are on Coumadin and chances are you will be, be very cautious when getting pedicures and manicures. Tell your nail tech to be very gentle since you are taking Coumadin and if cut, could bleed very easily.
- Practice run when ready to return to work. When I was ready to return to work, I found it helpful to take a practice run a week before returning. For me particularly, I have to commute via a train and then walk seven blocks to work. Taking a practice run allowed me the ability to calculate how long it would take me to walk to work once my train arrived. This practice run also serves as a great physical barometer in terms of whether or not you are up to returning to work, or need any additional time to recuperate.
- Leave the Kitchen Sink at Home. I would recommend traveling light in terms of just essentials. Women’s purses tend to get weighed down and initially you will want to carry a lighter load as your muscles are still recovering. I personally found that any additional weight from my purse or tote bags pulled at my chest and shoulders and would cause me to be sore around my incision sight. Leave the kitchen sink at home, and if you find that you truly need it, then carry it on wheels temporarily.
- Strike a Pose! Vogue. In the words of Lady Madonna … “You try everything you can to escape the pain of life that you know … All you need is your own imagination So use it that’s what it’s for. ” This couldn’t be more true than when you return to work and reassess your wardrobe. As a note of caution, you may find yourself standing in front of your closet, choosing your outfit for the day and realize that what you chose to wear revealed too much of your scar. Ladies, this is where your imagination comes into play. Keep in mind that scarves (whether summer or winter) necklaces and the like are great accessories while you are in a transition period. Do not feel discouraged. Embrace your scars. Know it is only a temporary speed bump in the big picture. Soon you will be back in the driver’s seat and living life.

After enduring open heart surgery, three post – op cardio versions, 36 sessions of cardiac rehabilitation and most recently a cardiac cather ablation, a childhood memory from the animated Christmas classic Santa Clause is Coming to Town sung by the voice talents of Mickey Rooney and Keenan Wynn is what kept me going.
Put one foot in front of the other
And soon you’ll be walking cross the floor
Put one foot in front of the other
And soon you’ll be walking out the door
You never will get where you’re going
If you never get up on your feet
Come on, there’s a good tail wind blowing
A fast walking (wo)man is hard to beat
(Chorus)
If you want to change your direction
If your time of life is at hand
Well don’t be the rule be the exception
A good way to start is to stand
(Chorus)
If I want to change the reflection
I see in the mirror each morn
You mean that it’s just my election
To vote for a chance to be reborn
Don’t give up, keep moving and you will get there, one heartbeat at a time. You WILL make it across that finish line!
Christine Rakesh Wagner
Chicago, Illinois
|
Susan Smith says on March 27th, 2014 at 7:15 pm |
|
Talk about good timing. I am in my last 30 days before surgery and Christine gave so many good tips that I started make a list of things to do and get. Some things I already had and some things will need to be obtained. Thanks Adam, once again you come in like a knight in shining armor and save the day or one might say that you hit the mark or the bulls eye on the target. I am going to make a copy of it and use it along with your book for my guide. The Journals the patients have written have given me the boost and the courage to face this life changing event. It is bringing my family together as they are all over the USA. One is in Portland, Oregon, One in Middletown, Connecticut and the other in the foothills out of Denver, Colorado and I am in Florida. Thank you very very much. Most sincerely Susan Smith |
 |
|
Suzanne Kosakowski says on March 27th, 2014 at 7:25 pm |
|
Thanks so much for sharing your experience. I will be going to the Cleveland Clinic on April third for a second opinion on when to have aortic and mitral valve replacement surgery. Needless to say I am scared to death to find out it needs to be done sooner rather than later. Having someone like yourself provide so much valuable insight into what’s ahead is comforting to me. Again thank you! |
 |
|
Sandra Graham says on March 27th, 2014 at 7:43 pm |
|
I am nearly 20 years post-aortic valve replacement. I was 42 when my bicuspid valve was replaced with a St. Jude’s mechanical valve. Your tips are wonderful. The more you know what to expect, the better you feel. One thing I remember reading is that when waking up on a respirator, it is better to relax and let it breathe for you. The instinct is to fight it, which causes you to feel like you are choking. Once I remembered to relax, I realized I was not choking. I have had a wonderful life since the surgery. My children are grown now, and I am 62 years old, but I am in excellent health. |
 |
|
Pat Hitchens Bonow says on March 28th, 2014 at 5:42 pm |
|
These tips are great! Lots of valuable info for a woman facing ANY type of inpatient hospital time. |
 |
|
Angela Creason says on March 28th, 2014 at 11:44 pm |
|
Great tips! |
 |
|
Carol Jackson says on March 29th, 2014 at 3:59 pm |
|
Good ideas. I mentioned many of the same things in my journal. I had surgery October 8, 2013. If you want, you can search for Carol Jackson in the journal section of this site and go to the Nov. 22, 2013 entry. |
 |
|
Jan Arabas says on March 30th, 2014 at 10:31 am |
|
Really great to read other woman’s perspectives–the suggestions are right on. My heartfelt best wishes to all, |
 |
|
Christine Walters says on March 31st, 2014 at 12:10 am |
|
If possible I would like to talk with or email Angela who had her surgery at Stanford. I will be having surgery there in July. |
 |
|
Angela Creason says on March 31st, 2014 at 8:20 am |
|
Christine, search for me in the patient community, my journal should help, but if you leave a guest book comment with your email address, I can delete it from the guest book, or I can reply with mine and delete, just so our email addresses aren’t floating out there, and I’d love to answer any questions you may have! 🙂 |
 |
|
Angela Creason says on April 2nd, 2014 at 6:33 am |
|
Hi Christine! |
 |
|
DVB says on April 5th, 2014 at 10:12 pm |
|
Fantastic! Working through a list like this is just the ticket to give yourself control and keep pre-op anxiety at bay. |
 |
|
Deb Bialecki says on April 9th, 2014 at 3:49 pm |
|
Hi Christine. |
 |
|
Johnna says on April 28th, 2014 at 11:49 am |
|
Thank you! I am 3 days before my OHS to repair aortic valve stenosis and aortic aneurysm – which was diagnosed 2weeks ago. This blog post (and your blog in general!) has been amazing – I feel better about the surgery and the recovery! I am a triathlete and knew I had a binary aortic valve but was never told it needed monitoring. I did a half ironman race and struggled with fatigue on the run and chest pain during my attempts to run the following week. So thankful for your info! Take care, |
 |
|
Joanna Prisiajniouk says on May 19th, 2016 at 4:35 pm |
|
This was so thoughtful of you to go into this sincere and lengthy detail! Thank you so much, God bless you and all who are soon going through this surgery or who are recovering! I too will be seeing Dr. McCarthy next month. I was wondering if you too gained much water weight from the bypass machine? |
 |
|
Christine says on May 19th, 2016 at 9:08 pm |
|
Hi Joanna – my heartfelt wishes for a very successful meeting with Dr. McCarthy next month. It is my pleasure to be able to share this valuable information with my heart sisters and caregivers. Yes, I did gain a ton of water weight post surgery but truthfully, I had no idea that it was from the bypass machine. I attributed it to the medications and overall trauma of the operation. What I can tell you is that once I was discharged home and with the lasix for a few weeks thereafter (oh and those horrible compression stockings) I was able to see my ankles once again. This is why I recommend a slip on shoe when going home. Even if I wanted to wear a full shoe, there’s no way it would fit. Slippers w a good sole or flip flops is what I would recommend. Feel free to reach out if you have any follow up questions after your visit with Dr. McCarthy and team. Happy to help. |
 |
|
Joanna Prisiajniouk says on May 19th, 2016 at 9:59 pm |
|
Thanks again Christine! It feels so good to know that there is this forum and folks like you who share what we worry about. I feel blessed that you and all here provide help for so many. I did not get Adam’s book yet. I wonder if this water weight is mentioned as an after effect of the surgery? Does it effect everyone? Anyway, please let me know if you suffered any temporary memory loss or depression post op as this weighs on my mind a lot reading other forums on this side effect of the heart/lung machine of which can linger for quite some time. Of course many things like weaning off the medications can factor into this but depression is quite common. |
 |
|
Eliza Hadjisotiriou Wilson says on May 19th, 2016 at 11:45 pm |
|
Many thanks for sharing all this info with us…i am a moderate mitral valve patient and very worried of what will happen to me…since i was diagnosed my pschycology is to a very low level……this experience of yours makes me feel much better …God bless |
 |
|
Christine says on May 20th, 2016 at 7:32 am |
|
Good morning. Thank you for your kind words. I remember far too well the day of the consult and then being told to schedule my surgery. I immediately broke down in tears. The first thing I asked for was was there anything they had in terms of me reviewing first in how to prepare for my surgery? Can I digest this first and then schedule a date? Out came Adam’s book. I thought they were giving it to me. Lol. I immediately took note of it and upon arriving home the first thing my husband did was order two copies. One for us and then one for my family. I highly recommend you read his book, as well as pass on to your caregivers. Adam does a phenomal job hands down portraying the process and what to expect. It is a must read for all. That being said, one element that is very different from his journey, is the preparation and process from a females perspective. I am very thankful that he has featured my tips and tricks from the journal that I kept during my journey from start to finish. There are many things that may affect women differently than men. Given this difference, here is my pearl of wisdom to you re recovery. I, like you, and others was very concerned about the effects of the heart and lung machine. I also read about the possibility of cardiac depression. Looking back, I now know what it meant when doctors could not give me a concrete answer when I asked, how long will it take for my recovery. Every body is different. While I was very healthy going into surgery, I endured a ton of post surgical complications that I had no idea even existed. I did not suffer from cardiac depression. While I had my moments of one complication after the next, I was very fortunate to have a strong support structure of my husband, family and friends. I feel, that by preparing as much as possible beforehand, reduced any anxiety that could have been presented post surgery. I was fortunate to have time to prepare. Some are not, and I think that is where a majority of depression may settle in. Suffering from a cardiac event vs knowing that you have a little time to prepare for surgery is a major difference in my opinion. As a result of my strong support structure, I have made it my personal goal to pay it forward to others by providing my tips and tricks to those such as yourself. Very best wishes from my heart to yours. Please don’t hesitate to reach out as your date draws closer if you have any other concerns. |
 |
|
debbie pauley says on May 20th, 2016 at 8:46 am |
|
I am 60 and scared to death. I had my aortic valve replaced in aug.5th,2015 and now it leaks and my mitral valve leaks as well. Dr. wants me to make appointment with heart dr. in Houston,tx to have both fixed. please give me something good to hear about this. |
 |
|
Joanna Prisiajniouk says on May 20th, 2016 at 11:02 pm |
|
Thanks so much Christine! Indeed this is overwhelming and I cannot help but worry about everything. I’m sure everyone wonders if they will be the same post op. Trying to stay positive is truly a task. We all have to prepare that complications arise and all we can do is hope that our surgeons/cardiologists keep us at bay from these various issues to get us through it all. There are days I feel better and strangely calm and other days is nothing but pure anxiety. My cardiologist told me I have a lot of calcification on my aortic bicuspid valve so a pacemaker might be a result if my natural pacemaker gets damaged in surgery by removing all calcified areas. I read the chances are not that high but nonetheless, just this alone is really nerve racking. Have you or anyone here know more about this that all go through surgery that is always watched for as a possible outcome from surgery? |
 |
|
Christine says on May 21st, 2016 at 7:09 pm |
|
Hi Joanna – I can relate to the ups and downs of preparing for the surgery. Some days I was super strong looking forward to getting this behind me and other days I needed to expect to prepare for the worst. A very tough pill to swallow at best. For me, I found that removing myself from all the external factors of everyday life and spending a day in reflection at a local retreat center, gave me the much needed strength to prepare. Ironically, I came across St John of God, a Catholic Saint for those suffering from heart disease in the gift shop. Upon leaving the center, I was calm and at peace with the pending surgery. in God we trust! Trust that what you are about to face, will be what is meant to be to make you stronger and healthier. Re your question.. I am unsure re the exact content of your question. Can you expand? |
 |
|
Joanna Prisiajniouk says on May 21st, 2016 at 7:24 pm |
|
I’m worried about the possibility of a pacemaker if the heart is too slow after the surgery. It has been explained by Dr McCarthy that the space they work in between the aortic and mitral valve to sew in your new valve is the area where our natural pacemaker resides and it might get damaged while they work around there…has he explained this to you? |
 |
|
Christine says on May 21st, 2016 at 7:35 pm |
|
Thank you for the clarification. Unfortunately I did not encounter the aortic valve issue and subsequently the pacemaker concerns and cannot offer any input. I am sure though, if you post your concerns re pacemaker and aortic valve – you will receive more specifics that I cannot offer. |
 |
|
Christine says on May 21st, 2016 at 7:40 pm |
|
Hi Debbie – while I can only imagine your freight re the current heart valve issues – I would recommend making that appointment and seeing what the team has to offer. Remember, also seek a second opinion upon meeting with initial team. You can then compare notes and feel comfortable with your selection. Hope this helps – |
 |
|
Christine says on May 21st, 2016 at 7:47 pm |
|
Thank you Eliza – All the best from my heart to yours- |
 |
|
Joanna Prisiajniouk says on May 21st, 2016 at 8:10 pm |
|
Thanks Christine! I wholeheartedly appreciate all your replys! Whether it is a mitral or aortic valve, this issue is a possible need of a pacemaker after surgery. I will talk to the surgeon more about this. Thank goodness you had no issues with it to even worry about! |
 |
|
debbie pauley says on May 21st, 2016 at 9:55 pm |
|
Can anyone tell me some great, kind, nice, and dr. That will come visit more than one time after surgery. I need a good doctor to redo the mechanics Calvary in my arotic and do what they have to to my mitral valve at the same time |
 |
|
Eliza Hadjisotiriou Wilson says on May 22nd, 2016 at 3:18 am |
|
Many thanks Christine…I will keep up with your advice…my next appointment for my echo is scheduled for June 17, 2016…..every six months he said…..very stressed about the results….i will keep you posted ….lovely weekend to all xxxx |
 |
|
Joanna Prisiajniouk says on May 22nd, 2016 at 10:23 am |
|
Hi Christine, What was the name of the retreat center? |
 |
|
Christine says on May 22nd, 2016 at 6:55 pm |
|
What area are you in? You may want to check out Adam’s surgeon section. There are a variety of top notch hospital and surgeons that are featured depending on where you are geographically located. |
 |
|
Christine says on May 22nd, 2016 at 7:13 pm |
|
Hi Joanna – Dr Mc Carthy did not go into any detail re the pacemaker issue as it sounds like you may have an additional valve issue that may need to be addressed. What I can say is that rest assured he is very knowledgeable in his arena. As a result, I am confident he will cover all details with you. Re the retreat center there are quite a few depending on where you are located. Portincula Center Prayer is the center that I found. |
 |
|
Joanna Prisiajniouk says on May 22nd, 2016 at 7:46 pm |
|
Hi Christine, Thanks for your help! No, I do not have another valve issue. I have found that if you don’t ask questions, a lot of things are not mentioned or explained whether it pertains to you directly or not. I had my cardiologist instead of answering one of my initial surgery questions he said, “What does it matter when you need to have surgery anyway?”A sign of bad bedside manner in my opinion…sometimes I honesty feel many do not like questions. Very aggravating! |
 |
|
Lori Phillips says on May 24th, 2016 at 3:16 am |
|
On June 13, 2016 I will be reporting for surgery to replace or repair my tri-cuspid valve regurgitation. Your story and tips could not have come at a better time. You lifted my spirits and shaved off a little anxiety. Wow! Thank you so much Christine. You’ve given me some pre-op chores, a month away from my surgery to keep my mind occupied. I have heard from friends that had open-heart surgery that post-op and/or fully recovered, they suffer major depression. Is this common? How do you fight that to get up in the morning and get dressed when you know you won’t be going anywhere? Trying to stay positive now. The anxiety is high, though hearing your experience has helped! I will be buying that book! Thanks again! Lori 47 years-young! |
 |
|
Jane says on August 15th, 2017 at 5:18 am |
|
Thank you so much Christine for sharing your experience. Your positivity and determination have inspired me to find the same sort of courage when my aortic valve replacement and aorta repair happens within the next year. I am 51 so a bit older than you were but I’m now reassured that post-op won’t be as difficult as I feared (not easy though by any means!). Your pre-op prep tips were really practical, thank you! I hope you are in good health and enjoying life to the full. |
 |