Valve Clinic Tour: Dr. Patrick McCarthy Returns Home To Lead The Bluhm Cardiovascular Institute At Northwestern Memorial Hospital
By Adam Pick on November 9, 2011
In 2004, one of the leading heart valve surgeons came home.
In the midst of his 30-year career, which includes time at Stanford University, The Mayo Clinic and The Cleveland Clinic, Dr. Patrick M. McCarthy returned to Chicago, the city of his birth, to lead the Bluhm Cardiovascular Institute at Northwestern Memorial Hospital.
Given Dr. McCarthy’s clinical achievements, research, cardiac inventions, publications and patient recommendations, I was thrilled to receive an invitation to tour Northwestern prior to the Heart Valve Summit.

Dr. Patrick McCarthy – Chief, Division of Cardiac Surgery
Bluhm Cardiovascular Institute, Northwestern Memorial Hospital
During the tour, which included several meetings with medical and administrative teams, I quickly came to understand four reasons why so many patients within our community are enthusiastic about this program – which is currently ranked by US News and World Report at:
- No. 16 for cardiovascular care across the nation; and
- No. 1 for cardiovascular care in the Chicago-metro area.
Reason #1: Northwestern’s Cardiac Surgeons Are Heart Valve Specialists
Dr. McCarthy has assembled a team of dedicated cardiac surgeons with sub-specialties to treat cardiac disorders including aortic stenosis, mitral regurgitation and atrial fibrillation. For example, Dr. Chris Malaisrie has an extensive, clinical interest in aortic valve disease. Dr. Richard Lee has an extensive clinical and research background specific to atrial fibrillation. Then, there is Dr. McCarthy who has performed over 10,000 cardiac procedures including more than 2,000 mitral valve surgeries.

Over the next few weeks, we will be posting several videos filmed with Dr. McCarthy’s heart valve surgeon team. So, stay tuned!
Reason #2 – Northwestern Offers A Unique, Patient-Centric Approach To Cardiac Surgery
Northwestern has developed a patient-centric approach to cardiac care that considers each phase of the surgical cycle.
- Before surgery, Northwestern offers patients access to extensive, educational materials located in its cardiac library. In addition, Northwestern recognizes the important role of caregivers in the surgical process. I was surprised when Georgeanne Barileau, the heart valve clinic coordinator, showed me a document designed exclusively for the caregivers. Amazing!
- After surgery, patients are provided their own, private room. These “rooms” feel more like newly renovated, hotel suites furnished with flat panel televisions, Internet access, spacious bathrooms and a television channel dedicated to cardiac care. Interestingly, I learned that private rooms lead to decreased rates of post-operative infection, which is below 1% at Northwestern.
- During recovery, Dr. McCarthy’s team closely monitors the physical and emotional recovery of their patients. Specific to the often-overlooked issue of cardiac depression, Dr. McCarthy shared with me, “We hired two clinical psychologists at the Bluhm Cardiovascular Institute to better manage this post-operative issue.”
Dr. Kim L. Feingold, PhD, who runs this program, recently launched SMART Heart (Stress Management and Recreational Therapy). Through a host of activities like playing board games, watching comedies and listening to music, the Bluhm Cardiovascular Institute uses SMART Heart as a way to help patients manage stress and reduce what can be for many a heavy emotional burden following surgery.

Northwestern’s S.M.A.R.T. Heart Room
“When we think about heart surgery, most people think you go into the hospital, have surgery and then start to work on the physical recovery,” said Feingold. “Few people recognize the significant psychological burden associated with heart surgery. Two out of every five cardiac patients are clinically depressed.”
The SMART Heart program centers around a specially-designed room where patients and their families can spend time together, engaging in relaxing activities like watching television, reading books or simply talking.
Reason #3: Northwestern Achieves Superior Surgical Outcomes
The result of Northwestern’s approach to cardiac care has resulted in surgical outcomes that deserve attention. As you can see in the chart below, Northwestern’s cumulative, 5-year mortality rates are superior to the national average reported by The Society of Thoracic Surgeons. It should also be highlighted that, during 2010, the clinic reported 0% in-hospital mortality for mitral valve procedures.
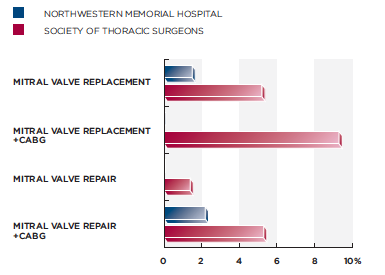
Specific to isolated aortic valve procedures, Northwestern’s surgical outcomes continue to shine. In-hospital mortality for isolated aortic valve replacement, during 2010, was only 1.3% compared to the national average of 2.7%. To learn more, I encourage you to download “Northwestern’s 2010 Surgical Outcomes Report”.
Reason #4: Northwestern’s Team Is Anything But… Complacent
Even with the above-referenced results, Dr. McCarthy, who is the youngest of eight children (all boys), is anything but complacent. “We feel good about our accomplishments, but there is more we can do,” Dr. McCarthy shared with me. “For example, we are now launching a bicuspid aortic valve program. I believe we can improve our understanding, research and treatment of that disease.”
Specific to bicuspid aortic valves — which led to my own aortic valve replacement surgery in 2005 — I used my time with Dr. McCarthy to learn more about the genetics of the disorder. In this video, Dr. McCarthy answered Cindy’s question about the heredity of bicuspid aortic valves.
For the hearing impaired members of our patient and caregiver community, I have provided a video transcript below for your review.
Many Thanks To The Bluhm Cardiovascular Institute At Northwestern!
As the tour came to a close, I was inspired by Northwestern’s pursuit of healthy hearts. I want to thank each person I met during my time at the Bluhm Cardiovascular Institute. In particular, I would like to thank Georgeanne Barileau for coordinating this incredible visit. In addition, I would like to thank Dr. Malaisrie and Dr. Lee for filming several video responses to your questions — which will be posted shortly at my blog.
Finally, I want to extend a special thanks to Dr. Patrick McCarthy for his extraordinary contributions to heart valve therapy. It was incredible to learn more about this surgeon who is one of the most patient-recommended physicians in our community.
- To learn more about Dr. McCarthy, please click here.
Keep on tickin!
Adam
P.S. For those of you who are hearing impaired, a written transcript of my video interview with Dr. McCarthy is provided below.
Adam: Hi everybody, it’s Adam, and we are at the Bluhm Cardiovascular Institute at Northwestern Memorial Hospital in Chicago, Illinois. I’m thrilled to be here with Dr. Patrick McCarthy who’s the chief of cardiothoracic surgery, and we’re answering your questions that were submitted at HeartValveBlog.com. This is a question that came in from Cindy, and she writes, Dr. McCarthy, “Two years ago I was diagnosed with a bicuspid aortic valve and underwent surgery to replace it. As a mother and grandmother, I want to know if this type of problem can be passed to my daughter and granddaughter. I have attempted to research but have found conflicting answers regarding heredity.
Doctor McCarthy: So it’s a good question Adam, and it’s also very timely. So the data now is that about 1 out of 4 it runs in a family, so about 25%. And 75% therefore, it doesn’t; so it’s not that common. But when I sit there and I talk to patients that have a bicuspid aortic valve, I always ask them, does it run in the family, is your uncle, brother, anyone like that have it. And it’s pretty common that you find that, or an aortic aneurism, because the two are related. The reason that it’s timely, this year in particular, the medical societies have come up with a recommendation that first degree relatives of someone with bicuspid aortic valve should have an Echo. First degree relatives refers to someone directly related. For instance, you mentioned her daughter, her parents, her siblings (brothers and sisters), doesn’t have to be your second or third cousin at all. On the other hand, in general, if someone has a heart murmur they should get an Echo. I’m always surprised at people that had a heart murmur for twenty years but have never had an Echo, and finally it’s done and they pick up a bicuspid valve or mitral valve prolapse. But Cindy asked a good question, her daughter should have an Echo, even though she doesn’t have a heart murmur. If her parents are still alive they should have it. Her brothers and sisters, they should have it. And that’s a new recommendation coming from the societies; and it’s actually changing the way we practice, for instance here we set up a bicuspid aortic valve program and I asked Dr. Jyothy Puthumana to be in charge of this to help, because there are so many patients that we see with this, and now so many family members, and they have questions about, “is this going to be a problem for me in the future?”. They’re twenty years old, and their valve is functioning fine; but it’s bicuspid. So they need a lot of information about that. For instance one other thing they want to know is that if you do have a bicuspid aortic valve, only about 1 out of 3 will eventually need surgery for it at some point in their life. But if you’re twenty, it’s important to know that kind of information.
Adam: As always, thanks for your help and thanks for your support, and I know that’s going to help Cindy and I know it’s going to help all of the other viewers out there that are watching this. So again, thanks for all you’re doing here at Northwestern.
Dr. McCarthy: Thanks Adam.
|
Lynda Knopf BS/RN says on November 9th, 2011 at 6:17 pm |
|
THANK YOU AGAIN ADAM for another informative, supportive blog. SPECIAL ATTENTION should be paid to possible depression, which after heart surgery, is an insightful and assuring comfort. I was fortunate to experience thrilling “survival elation” upon awakening from aortic valve replacement surgery — making my recovery an easy feat! |
 |













